Recognizing and Managing the Musculoskeletal Manifestations of Sarcoidosis
Noncaseating epithelioid granuloma is the histological hallmark of sarcoidosis, which can masquerade as several other disorders, because multiple organs can be affected. This article describes amultifaceted approach to diagnosis, and reviews treatment options.
Originally described by Boeck in the 1870s, sarcoidosis, or "new flesh formation," refers to the histological hallmark of the disease, noncaseating epithelioid granuloma. The noncaseating granuloma of sarcoidosis is a lesion composed of epithelioid cells that surround a central granular zone in a circular or arc pattern without necrosis.1
The respiratory system is thought to be involved at some point in the lifetime of all patients with sarcoidosis (Figure 1).2 However, the protean clinical manifestations (Table) can masquerade as a number of other disorders, because multiple organs-including the muscles, bones,and joints-can be affected.
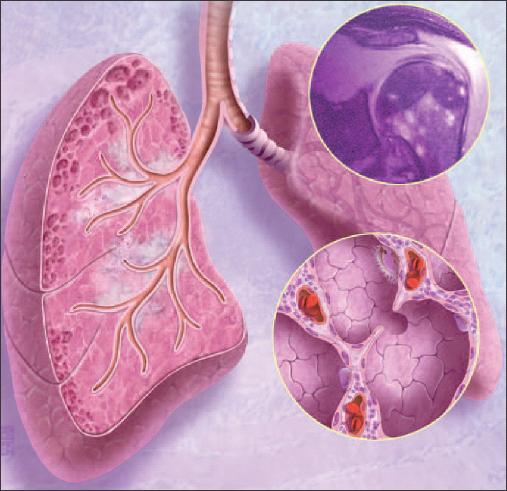
Figure 1 - In a patient with sarcoidosis, the lungs have gross pathology and there is inflammation within the alveoli (lower inset).The respiratory system is thought to be involved in all patients with sarcoidosis at some point in their life. Several other organs may be involved, as seen in a shoulder image of a patient with sarcoidosis (upper inset).

Table
Although musculoskeletal manifestations of sarcoidosis usually are not the presenting clinical feature, they are not rare. When looked for, they may provide clues to sarcoidosis when it presents in other tissues. Corticosteroids remain the most effective therapeutic intervention, but given the toxicity associated with their long-term use, management of sarcoid arthropathy, myopathy, and osseous lesions is best guided by the extent to which these manifestations are symptomatic. In this article, we describe our approach to recognizing and managing the musculoskeletal manifestations of sarcoidosis.
CAUSES AND EPIDEMIOLOGY
The etiology of sarcoidosis remains unknown. Men and women of all ages may be affected, but primarily young adults between the second and fifth decades are affected; there is a slight predominance in women. A second peak has been described in women older than 50 years.3,4
Epidemiological data have demonstrated ethnic and regional variations in the clinical presentations, disease course, and genetic susceptibilities of sarcoidosis; the incidence is higher in African Americans and Northern Europeans.5 Familial aggregation and genome-wide association studies have confirmed the genetic susceptibility. The disease therefore is thought to be induced by environmental factors in genetically susceptible persons.
Airborne particulate, viral, or mycobacterial pathogens and occupational exposures have been postulated as potential triggers in the pathogenesis of the disease. The inflammatory response is a cell-mediated aggregation of CD4+ TH1 phenotype lymphocytes with enhanced production of interleukin-12 and interferon-γ within the granulomatous lesions. The otherwise suppressed immunity reflected in the fascinating anergy phenomenon to tuberculin testing is speculated to occur as a consequence of enhanced activity of circulating CD8+ suppressor T lymphocytes and enhanced TH2 responses. However, the exact immunopathogenetic process that culminates in the clinical presentation of sarcoidosis remains elusive.6
Sarcoidosis may involve any organ system, manifesting a wide spectrum of disease severity. Extrapulmonary manifestations are common; they occur in the context of pulmonary features, except in a small minority of patients. Most notably, among patients with neurological involvement, it is important to recognize that the neurological lesions may be the presenting manifestation.
Extrapulmonary features, including musculoskeletal involvement, vary by gender and ethnic origin; the prevalence is higher among women and African Americans. Although reports of the rate of musculoskeletal involvement vary, up to 40% of patients with sarcoidosis have documented musculoskeletal findings.1-9 Musculoskeletal system involvement may be asymptomatic. This is important for clinicians looking for signs of sarcoidosis when considering it in the differential diagnosis of disease involving the eyes, CNS, or visceral organs.5
ARTICULAR MANIFESTATIONS
Arthralgia is reported in up to 70% of patients, often predating other manifestations of the disease.2,6 Lfgren syndrome (LS), originally described in 1952, is classically defined as the triad of acute arthritis, erythema nodosum, and bilateral hilar lymphadenopathy (BHL) of the lungs; it may be associated with fever and anterior uveitis. Reported predominantly in 10% to 39% of patients with early-onset sarcoidosis, LS may be the initial manifestation. 6,8,9 BHL and ankle arthritis or periarthritis are the main features of LS, but the necessity of the presence of erythema nodosum for making this diagnosis has been debated.10,11
The most common presentation of acute arthritis in sarcoidosis is an additive symmetrical oligoarthritis that predominantly involves peripheral large joints; symmetrical polyarthritis and asymmetrical transient polyarthralgia have been described less frequently. Although any joint may be involved, the ankles are the most frequently involved, followed by-in descending order-the knees, wrists, elbows, interphalangeal joints, metacarpophalangeal joints, and shoulders.2,8,12 Synovial fluid is inflammatory with lymphocytic predominance and protein elevation. The spontaneous resolution of arthritis within a few weeks up to 6 months indicates a benign course, but relapses have been reported.9,12
Chronic sarcoid arthritis occurs less frequently than the acute syndromes. It may follow a progressive course, resulting in erosive joint changes and deformity in a limited number of joints8,13 or a course characterized by episodic exacerbations and remissions of symmetrical polyarthritis marked by subsequent joint deformities (eg, Jaccoud deformity).12
Elevation of the rheumatoid factor (RF) level is reported in 10% to 47% of patients and may correlate with elevated levels of circulating IgG.7 As such, the combination of symmetrical polyarthropathy and elevated RF can clinically mimic rheumatoid arthritis. Relative sparing of the small joints of the hands and feet and the absence of radiological changes in sarcoidosis have been offered to aid in differentiation of the diseases,2,6 but these may not always be helpful.
Synovial histology may show the typical noncaseating granuloma or nonspecific inflammatory synovitis. 2,6,9,13 BHL is reported in 80% to 90% of patients with chronic arthropathy associated with sarcoidosis. 2,8 A retrospective comparison of patients with LS and patients with chronic sarcoid arthropathy demonstrated a higher frequency of interstitial lung disease in the latter group.8 Sacroiliitis is an uncommon manifestation of sarcoidosis, occurring in only 2% to 6% of patients.2
Periarticular inflammation
Soft tissue swelling, tenosynovitis, and dactylitis are among the periarthritic inflammatory changes in patients with sarcoidosis. These findings may be symmetrical or may present in an asymmetrical oligoarticular pattern. A variant of LS with ankle periarthritis is described in patients with ankle pain and swelling with BHL and maybe with erythema nodosum.This clinical syndrome was reported in 10% of a cohort of patients with sarcoidosis, but none of the 4 biopsies of periarticular ankle tissue revealed noncaseating granulomas.10
Sarcoid myopathy
Muscle involvement with sarcoidosis initially was described by Licharew in 1908. The true prevalence is difficult to ascertain because of limitations in the reported series, such as sample size, study design, and the sectioning methodology that was used, but asymptomatic muscle involvement in reported series occurs in up to 75% of patients.9 Symptomatic muscle involvement is much less common, occurring in only 0.5% to 1.4% of patients who have an established diagnosis of sarcoidosis.9,14,15 Given the high prevalence of positive pathological findings in muscle biopsy, this modality often is considered for diagnostic purposes but may not be used frequently because of patient discomfort.9,12
Muscle involvement in sarcoidosis may exhibit several patterns. Chronic myopathy is the most common manifestation of muscle disease; it involves symmetrical muscle weakness in a central and proximal distribution, predominantly in the lower extremities.The chronic, slowly progressive course of the disease may culminate in muscle atrophy, permanent function loss, and disability.
Myalgia may antedate the development of perceived or demonstrable weakness. Bulbar myopathy is infrequent but presents as difficulty in initiating swallowing. Facial and respiratory muscles usually are spared. Involvement of respiratory muscles may negatively impact measured lung volumes.15
Additional clinical findings include diminished deep tendon reflexes and changes in the consistency of the muscles, but these findings are not universally present.16,17 Symptomatic involvement of distal muscles is less frequent, occurs later in the disease course, and must be distinguished from underlying peripheral neuropathy. Chronic sarcoid myopathy typically follows a gradual progressive course, although some patients experience periodic exacerbations and remissions.
Clinical laboratory findings in chronic sarcoid myopathy include occasional elevation of the erythrocyte sedimentation rate (ESR), elevated calcium level, and variable elevations in creatine kinase level. Electromyography (EMG) and nerve conduction studies can discriminate myopathic, neuropathic, and mixed causes. False-negative EMG results may occur because of sampling error or granuloma formation outside the excitable units.9,18 MRI often is nonrevealing in chronic sarcoid myopathy; nuclear imaging with gallium scintigraphy has been used for diagnosis with increased uptake in the affected muscle.16,17,19
Nodular tumorous sarcoidosis is characterized by the presence of multiple intramuscular nodules with a longitudinal orientation typically extending along the muscle fibers.This variant of sarcoid myopathy, seen more frequently in men, becomes manifest as palpable mass-like lesions within muscles. MRI findings are characteristic and demonstrate well-demarcated nodules with a central star-shaped area of hypointensity surrounded by areas of increased T2 signal. CT reveals nodules with a central low attenuation area surrounded by a rim of increased opacity. Histopathological examination reveals dense central fibrosis surrounded by granulomatous inflammatory changes with lymphocytes and epithelioid noncaseating granulomas and giant cells. Fine needle aspiration and excisional biopsy can ascertain the diagnosis; the latter could also serve a therapeutic purpose.14,17,18,20
Acute sarcoid myositis is the rarest form of muscle involvement in sarcoidosis; it often is accompanied by acute inflammatory arthritis or periarthritis. Constitutional symptoms,myalgia, and weakness may be indistinguishable from the presentation of chronic idiopathic inflammatory myositis (polymyositis). Muscle biopsy reveals acute inflammation in the muscle fascicle and noncaseating granuloma formation with minimal fibrosis (Figure 2). Bulbar muscle dysfunction and dysphagia and an elevated creatine phosphokinase level are frequently described. EMG demonstrates a myopathic pattern, and MRI findings identify focal areas of muscle edema. Therapeutic response to corticosteroid and immunomodulators is favorable in most cases.14,17-20
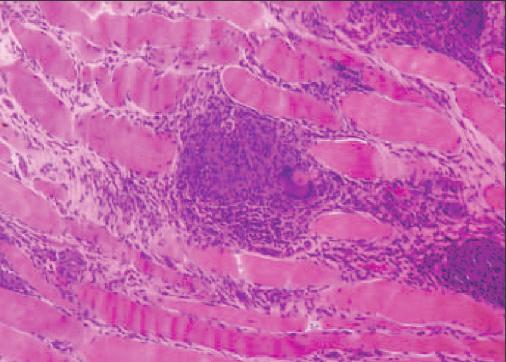
Figure 2 - This muscle biopsy of a patient with active sarcoid myopathy demonstrates fascicular inflammatory infiltrates with multinucleate giant cells. (All images provided courtesy of Dr Gwen Claussen,University of Alabama at Birmingham.)
Osseous sarcoidosis
Reported sarcoid involvement of bone ranges from 31% to 34%, depending on the population described and the diagnostic criteria used.1 Osseous lesions often are asymptomatic and noted as incidental findings. Bilateral involvement of the phalangeal bones of hands and feet with preservation of the periosteum and cortical margins is a hallmark of bone involvement in sarcoidosis. Nasal and vertebral involvement also have been described.1,2,21,22 Osseous involvement often is seen in association with skin sarcoidosis, especially in patients with lupus pernio, in whom nasal and skull lesions are particularly common.1
Bone involvement and associated metabolic abnormalities in sarcoidosis involve multiple processes. The development of hypercalcemia is related, in part, to 1,25(OH)2 vitamin D production by macrophages. Bone resorption is most likely mediated by the increased level of catabolic cytokines elaborated from cells within granulomas that enhance the activity of adjacent osteoclasts. Metabolic bone abnormalities resulting from prolonged corticosteroid use may further exacerbate bone resorption.
"Bone cysts" is a misnomer used for the sarcoid-mediated osteolytic bone lesions that become manifest as punched-out areas of cortical as well as medullary bone. "Tunneling" of the cortex and shaft of the phalangeal bones leads to the characteristic "lattice-like trabecular pattern" of bone seen on radiographs of the hands or feet (Figure 3).The progression of bone destruction may be complicated by superimposed pathological fracture. In large bones, well-demarcated lesions of variable size may be present with increased signal intensity noted in T2 imaging on MRI (Figure 4). Myeloma, lymphoma, some infectious processes, and metastases to the bone may yield a similar appearance; they should be ruled out to establish the diagnosis of osseous sarcoidosis.
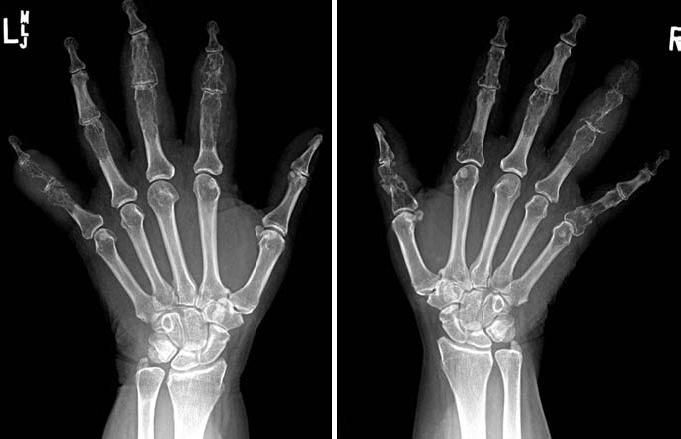
Figure 3 - Left (A) and right (B) hand radiographs of a patient with sarcoidosis show multiple foci of osteolysis as well as a "lattice-like trabecular pattern" in the phalangeal bones.
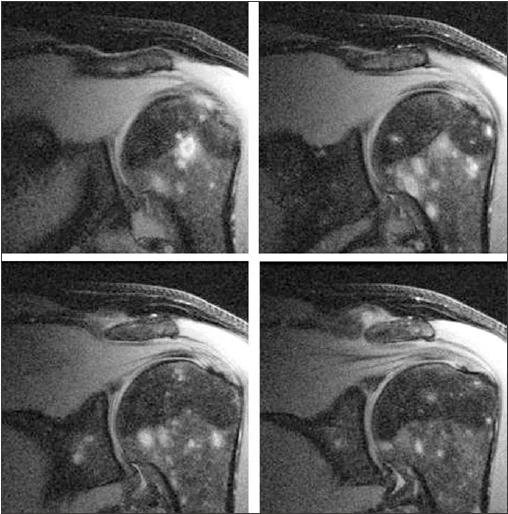
Figure 4 - Coronal MR T2 fat-suppressed shoulder images of a patient with sarcoidosis demonstrate abnormal islands of increased T2 signal within the marrow; biopsy confirmed the presence of noncaseating granulomas. Results of plain radiographs were normal.
DIAGNOSIS
Establishing the diagnosis of sarcoidosis requires a multifaceted approach with attention to clinical, histological, and imaging assessments and the elimination of other causes of noncaseating granulomas. With the possible exception of patients presenting with LS, histological confirmation of the presence of noncaseating granulomas in biopsy material obtained from lymphoid, lung, dermal, salivary/ lacrimal, or muscle tissue is prudent to establish the diagnosis of sarcoidosis.
Clinical laboratory abnormalities are nonspecific and not universally abnormal. They may include an elevated ESR; the serum calcium or alkaline phosphatase level may be elevated as a result of abnormal calcium and vitamin D metabolism. Elevation of angiotensin-converting enzyme (ACE) level accompanies about half the cases of LS or other acute presentations of sarcoidosis, but ACE levels are not reliable for diagnostic purposes or as an indicator of disease activity.2,23 Elevation of C-reactive protein level can be seen in 50% to 80% of patients with active articular or muscular involvement.8,9
Although plain radiographs of the metacarpal and phalangeal bones may reveal characteristic osseous lesions, MRI probably is the most sensitive imaging modality used to detect active noncaseating granulomas in bone, joint, and muscle; the reported sensitivity is 30% to 96%.19,20 Gallium scintigraphy has less sensitivity in detecting and localizing the involved tissue and is used less frequently.20 These imaging modalities may be useful to guide biopsy of appropriate tissue to establish the diagnosis.
MANAGEMENT
Musculoskeletal complaints, such as arthralgia and periarthritic pain, are common causes of discomfort in patients with sarcoidosis. In many patients, NSAIDs can provide relief of these symptoms.
However, systemic corticosteroids are still the mainstay of treatment for active sarcoidosis that involves musculoskeletal tissue and visceral organs. Chronic arthropathy and myositis, as well as recalcitrant disease in visceral organs, may require prolonged treatment; in these subgroups of patients, the use of corticosteroid-sparing immunomodulators is advocated.
Drugs that have been used with reported success in limited uncontrolled case series include methotrexate (MTX), antimalarials (hydroxychloroquine and chloroquine), azathioprine, cyclosporine, mycophenolate mofetil, and cyclophosphamide, given in the dose ranges of these agents used to manage rheumatoid arthritis or lupus.The benefits of MTX have been verified in acute forms of arthritis and myositis; however, long-term benefit of MTX in patients with chronic forms of musculoskeletal involvement is anecdotal and prospective clinical trials are lacking.9,24
For osseous sarcoidosis, prolonged treatment with high doses of corticosteroids (0.5 to 1.0 mg/kg/d of prednisone or the equivalent) often is required to achieve a clinical response. The benefits of achieving symptomatic relief with corticosteroids should be weighed against the risks of metabolic bone disease associated with such treatment.16,17,19
Despite receiving long-term treatment with corticosteroids, patients with osseous sarcoidosis may still experience relapses or progression. Other patients may experience remission spontaneously or in the setting of systemic therapy, further emphasizing the need to consider treatment with corticosteroids or other immunomodulating agents probationary.
Given the postulated role of tumor necrosis factor α (TNF-α) in engendering the formation of granulomas, biologic TNF-α inhibitors (eg, etanercept, infliximab,and adalimumab) have been used for patients with refractory or recalcitrant sarcoidosis. In one large multicenter randomized trial of infliximab in the treatment of sarcoidosis, a retrospective analysis indicated fewer and less severe extrapulmonary manifestations in the infliximab-treated group.25 However, the analysis used a nonvalidated instrument for assessing extrapulmonary disease, and insufficient numbers of patients with articular, muscular, or osseous manifestations were reported to draw any definitive conclusions about the efficacy of infliximab in managing the musculoskeletal manifestations of sarcoidosis. Published case reports on the use of etanercept in sarcoidosis do not suggest a consistent beneficial effect.
The utility of TNF-α inhibitors for management of sarcoidosis is further tempered by more recent case reports of the development of disseminated noncaseating granuloma lesions in patients with rheumatoid arthritis or psoriatic arthritis treated with etanercept or infliximab.Thalidomide, an immunomodulating agent that inhibits TNF-α production, has been considered primarily effective in recalcitrant sarcoid skin disease, but there are reports of favorable responses in chronic sarcoid myositis. 26 As more is learned with respect to the aberrant innate and acquired immune responses giving rise to the development of sarcoidosis, a rationale for additional targeted therapies should evolve.
Management of metabolic bone disease associated with sarcoidosis can become challenging when hypercalcemia and low bone mineral density coexist. Use of calcium and vitamin D supplements is discouraged in the presence of hypercalcemia, and patients need regular evaluations with bone densitometry. Use of oral or intravenous bisphosphonates and nasal or subcutaneous calcitonin administration can address both hypercalcemia and bone loss.24,27
In patients for whom musculoskeletal manifestations predominate, vigilance for serious visceral complications, particularly cardiac disease, is important. Cardiac sarcoidosis may be silent until it becomes manifest as a potentially fatal arrhythmia. As such, all patients who have sarcoidosis should be screened periodically with electrocardiography for evidence of conduction system abnormalities, and a low threshold for pursuing MR or PET scan imaging of the myocardium should be operative for patients presenting with palpitations, chest pain, or dyspnea.9,12
References:
References
- 1. Wilcox A, Bharadwaj P, Sharma OP. Bone sarcoidosis. Curr Opin Rheumatol. 2000;12:321-330.
- 2. Erb N, Cushley MJ, Kassimos DJ, et al. An assessment of back pain and the prevalence of sacroiliitis in sarcoidosis. Chest. 2005;127:192-196.
- 3. Costabel U, Hunninghake GW. ATS/ERS/WASOG statement on sarcoidosis. Sarcoidosis Statement Committee. American Thoracic Society. European Respiratory Society. World Association for Sarcoidosis and Other Granulomatous Disorders. Eur Respir J. 1999;14:735-737.
- 4. Hosoda Y, Sasagawa S, Yasuda N. Epidemiology of sarcoidosis: new frontiers to explore. Curr Opin Pulm Med. 2002;8:424-428.
- 5. ACCESS Research Group. Design of a case control etiologic study of sarcoidosis (ACCESS). J Clin Epidemiol. 1999;52:1173-1186.
- 6. Barnard J, Newman LS. Sarcoidosis: immunology, rheumatic involvement, and therapeutics. Curr Opin Rheumatol. 2001;13:84-91.
- 7. Oreskes I, Siltzbach LE. Changes in rheumatoid factor activity during the course of sarcoidosis. Am J Med. 1968;44:60-67.
- 8. Thelier N, Assous N, Job-Deslandre C, et al. Osteoarticular involvement in a series of 100 patients with sarcoidosis referred to rheumatology departments. J Rheumatol. 2008;35:1622-1628.
- 9. Zisman DA, Shorr AF, Lynch JP 3rd. Sarcoidosis involving the musculoskeletal system. Semin Respir Crit Care Med. 2002;23:555-570.
- 10. Grunewald J, Eklund A. Sex-specific manifestations of Lofgren’s syndrome. Am J Respir Crit Care Med. 2007; 175:40-44.
- 11. Perruquet JL et al. Sarcoid arthritis in a North American Caucasian population. J Rheumatol. 1984;11:521-525.
- 12. Awada H, Abi-Karam G, Fayad F. Musculoskeletal and other extrapulmonary disorders in sarcoidosis. Best Pract Res Clin Rheumatol. 2003;17:971-987.
- 13. Torralba KD, Quismorio FP Jr. Sarcoid arthritis: a review of clinical features, pathology and therapy. Sarcoidosis Vasc Diffuse Lung Dis. 2003;20:95-103.Â
- 14. Le Roux K, Streichenberger N, Vial C, et al. Granulomatous myositis: a clinical study of thirteen cases. Muscle Nerve. 2007;35:171-177.
- 15. Wirnsberger RM, Drent M, Hekelaar N, et al. Relationship between respiratory muscle function and quality of life in sarcoidosis. Eur Respir J. 1997;10:1450-1455.
- 16. Moore SL, Teirstein AE. Musculoskeletal sarcoidosis: spectrum of appearances at MR imaging. Radiographics. 2003;23:1389-1399.
- 17. Otake S. Sarcoidosis involving skeletal muscle: imaging findings and relative value of imaging procedures. AJR. 1994;162:369-375.
- 18. Otake S, Ishigaki T. Muscular sarcoidosis. Semin Musculoskelet Radiol. 2001;5:167-170.
- 19. Moore SL, Teirstein A, Golimbu C. MRI of sarcoidosis patients with musculoskeletal symptoms. AJR. 2005;185:154-159.
- 20. Judson MA. The diagnosis of sarcoidosis. Clin Chest Med. 2008;29:415-427, viii.
- 21. Yanardag H, Pamuk ON, Kiziltan M, et al. An increased frequency of carpal tunnel syndrome in sarcoidosis. Results of a study based on nerve conduction study. Acta Medica (Hradec Kralove). 2003;46:201-204.
- 22. Shorr AF, Murphy FT, Gilliland WR, Hnatiuk W. Osseous disease in patients with pulmonary sarcoidosis and musculoskeletal symptoms. Respir Med. 2000;94:228-232.
- 23. Mana J. Magnetic resonance imaging and nuclear imaging in sarcoidosis. Curr Opin Pulm Med. 2002;8:457-463.
- 24. Baughman RP, Winget DB, Lower EE. Methotrexate is steroid sparing in acute sarcoidosis: results of a double blind, randomized trial. Sarcoidosis Vasc Diffuse Lung Dis. 2000;17:60-66.
- 25. Judson MA, Baughman RP, Costabel U, et al; Centocor T48 Sarcoidosis Investigators. Efficacy of infliximab in extrapulmonary sarcoidosis: results from a randomised trial. Eur Respir J. 2008;31:1189-1196.
- 26. Walter MC, Lochmüller H, Schlotter-Weigel B, et al. Successful treatment of muscle sarcoidosis with thalidomide. Acta Myol. 2003;22:22-25.
- 27. Sharma OP. Hypercalcemia in granulomatous disorders: a clinical review. Curr Opin Pulm Med. 2000;6:442-447.