OARSI Debates Whether to Focus on Tissue or Pain in OA
At the OARSI annual meeting in Philadelphia, two osteoarthritis experts tacklde the issue of whether to focus first on structural abnormalities or pain, and merged toward a consensus.
That doctors lack satisfactory solutions for osteoarthritis (OA) pain is an subtext in many of the presentations at the Osteoarthritis Research Society International meeting, now under way in Philadelphia. Is the prominent focus in OA research on correcting structural and tissue malfunction a trip up a blind alley, or at least in the wrong direction? Should the bulk of research be reoriented toward pain relief?
That was the thrust of a scheduled debate at the conference, assigned to two heads of rheumatology divisions: Steven Abramson MD of NYU Langone Medical Center and Marc Hochberg MD PhD of the University of Maryland Medical Center. An artificial dichotomy, perhaps, but an audience vote at the outset seemed to favor the focus on structure, and the speaker assigned to defend a focus on pain had to concede the role of damage in causing it.
Disillusionment and Setbacks for DMOADs
Abramson, assigned to defend the current focus on joint structure, spoke of a disillusionment with pain treatments that derives from the inadequate effect sizes and the adverse effects of existing medications used for OA pain, as well as from the failure of randomized trials of disease-modifying OA drugs (DMOADs). At OARSI in 2000, he remarked, pain researcher Jean-Pierre Pelletier MD of the University of Montreal heralded the coming "Decade of the DMOAD." By the end of that decade, many pharmaceutical firms had dismantled their DMOAD programs to focus instead on analgesia, "to the detriment of the field." Lacking good alternatives for severe OA pain, he said, many rheumatologists now turn to opioids.
The recent disappointment with tanezumab, whose development was temporarily halted by the FDA due to concerns about bone necrosis, was followed by another setback, he added: Analysis of data from the Agency shows that however effective as an analgesic, tanezumab does not ultimately decrease the likelihood of total joint replacement.
Targeting OA in Space and Time
"All patients come to us because they have pain," said Abramson early in his remarks, "but only some progress to dysfunction and total joint replacement." The important research of the future, he
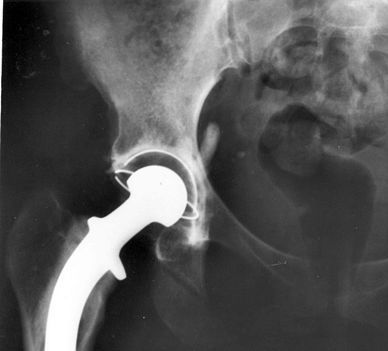
predicted, will "target OA in space and time," looking for ways to identify the molecular targets unique to early phases of pre-osteoarthritis that work to reduce the joint space, to initiate treatments early in the course of disease, and to identify "rapid progressors". DMOADs that are effective in animal models may fail in human trials, he suggested, because by the time humans are recognized as having OA it is too late to modify the disease.
Is it even necessary to treat the pain, he went on, in order to develop effective DMOADs? Analagous to the use of bone-modifying drugs against osteoporosis, he added, it may become possible to use DMOADs to prevent later joint failure, in the absence of any pain.
There are obstacles, he said, such as the lack of quantitative definitions of progression and of good biomarkers. But Abramson predicted that this may in fact be the decade of the DMOAD, as robust new clinical databases and bio-repositories and international collaboration lead to a better understanding of osteoarthritis incidence and progression.
"We should not let looking for pain medications impair our development of new drugs," he said.
Several Questions With the Same Answer
Hochberg, defending the alternate position, provoked the same loud response of "Pain!" as he challenged the audience with several questions:
Why do people with structural OA seek medical care?
Why do people with structural knee OA develop functional limitations?
Why do people with OA of the lower limbs undergo total joint replacements?
Noting some of the ample data documenting a "wide discordance between radiographic knee osteoarthritis and knee pain," Hochberg pointed out a study that showed a dose-response relationship between functional status and arthritis symptoms, in which symptomatic OA, not asymptomatic OA detected
radiologically, was associated with functional limitations. An abstract at the current OARSI meeting, he added, showed that after adjusting for factors such as age, gender, and BMI, the best predictors of future total knee replacement are pain, functional limitations, and quality of life.
Furthermore, he added, even eradicating the faulty structure may not solve the problem. He cited a recent study that found that about half of patients who underwent total joint replacement (38% of those with hip replacements and 53% with knee replacements) reported pain persisting up to a year postoperatively. This underscores the role of centralization of pain perception in some patients, Hochberg said--an explanation for these results that is now being tested.
Phenotyping Pain
"As an academician," he conceded in response to a later question, "I know that patients are not only coming in with pain, but that it is emanating from damaged tissue. I don't want to ignore the importance of tissue. My focus on treating pain was related to the artificiality of the topic."
A number of presentations at the meeting point to the role of biomechanics, including gait and muscle weakness, in causation of pain, he added. "It's important to phenotype patients and to learn what may be the cause of their pain, in order to target the treatment."