When diagnosis of rheumatologic disease does not "follow the book"
Not all patients with symptoms suggestive of a rheumatologic disease leave their doctor's office with a firm diagnosis in hand.
Not all patients with symptoms suggestive of a rheumatologic disease leave their doctor's office with a firm diagnosis in hand. Although disease classification and diagnosis guidelines are available to help physicians evaluate their patients, a rheumatologic disorder can present atypically, or the patient might not have all of the criteria needed to unequivocally support a given diagnosis. Also, the clinical picture may change as the disease progresses from early to middle and late stages. Consider, too, that many physicians practice in areas where specialists are not available to consult on cases that are especially challenging or questionable.
Thus, the process of arriving at an accurate diagnosis often is an imprecise art. The physician may revisit evidence, assess the patient at intervals, test response to treatment, consult with colleagues, and rely on past experiences rather than primarily on a published list of diagnostic criteria to confirm his or her clinical suspicions.
Scleroderma (systemic sclerosis) is a rheumatologic disorder that can be mistaken for rheumatoid arthritis (RA) or mixed connective tissue disease. Accurate diagnosis influences assessment of the patient's prognosis as well as the choice of management. In this article, we use a scleroderma case study to highlight the potential for misdiagnosis of a rheumatologic condition and demonstrate potential pitfalls the physician might encounter when evaluating patients.
Case presentation
MJ is a 62-year-old man with pulmonary fibrosis. In 2006, he was referred by his primary care physician to the rheumatology clinic with a provisional diagnosis of mixed connective tissue disease and RA. The patient had a 30-year history of the following rheumatologic symptoms: diffuse skin tightness; general fatigue; sicca syndrome; Raynaud phenomenon; and constant, moderately severe bilateral hand pain. The hand pain worsens in the mornings, when MJ's hands are also stiff for about an hour.
Findings
On examination, the patient had no skin tightness. However, Velcro rales were audible at the lung bases. MJ exhibited contractures of his fingers, primarily at the level of the proximal interphalangeal (PIP) and distal interphalangeal (DIP) joints. His fingertips had pitting scars, and his distal finger pads lacked substance.
Laboratory test results completed at this visit were as follows: antiscleroderma (Scl) 70 antibody, 684 U/mL (normal range, 0 to 99 U/mL); white blood cell count, 5000/μL; erythrocyte sedimentation rate, 110 mm/h; C-reactive protein level, 38 mg/L (normal range, less than 5 mg/L); blood urea nitrogen level, 14 mg/dL; creatinine level, 1 mg/dL; rheumatoid factor (RF), positive; and antiribonucleoprotein (RNP) antibody, negative.
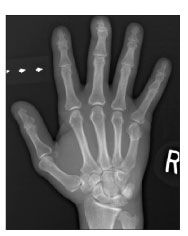
Figure 1 – A radiograph of the right hand of a 67-year-old man with possible scleroderma shows erosive osteoarthritis with degenerative changes in the distal interphalangeal joints and resorption of distal phalangeal tufts, which is highly suggestive of scleroderma and typically not seen in rheumatoid arthritis without an overlap.
Chest radiographs showed a diffuse interstitial pattern predominantly involving the lung bases. Radiographs of the hands showed erosive osteoarthritis; degenerative changes were seen in the DIP joints along with resorption of distal phalangeal tufts, which is highly suggestive of scleroderma. There were no erosive changes to suggest RA (Figure 1). CT of the chest revealed bibasilar parenchymal opacities (Figure 2). It is important to note that the neither the x-ray film nor the CT scan findings are specific for scleroderma. Results of repeat RF testing performed on the day of evaluation were negative.
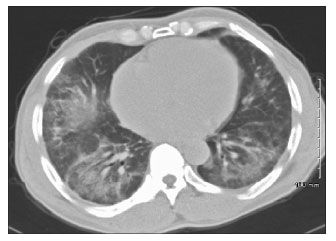
Figure 2 – A CT scan of the patient's chest shows alveolar opacities within the lung bases on both sides, which is not specific for scleroderma or any other rheumatologic disease that could affect the lungs.
The patient's physician made a diagnosis of scleroderma with positive anti-Scl 70 antibody based on the following findings from the history and physical examination: the presence of diffuse cutaneous scleroderma in the early stages; nonerosive arthritis with tendinopathy and contractures; severe Raynaud phenomenon, with fingertip ulcerations, pitting scars, and substance atrophy in the distal finger pads; sicca syndrome; and pulmonary fibrosis. The patient was taking prednisone, 20 mg/d, and oral methotrexate (MTX), 10 mg/wk, a regimen he had followed for the past 5 years. Because the arthritis appeared to be degenerative and MJ's pulmonary fibrosis was stable, medications were discontinued according to standard protocol (eg, MTX was stopped and prednisone was tapered).
It is possible that MJ had an active alveolitis or inflammatory nonerosive arthritis in the earlier stages of his disease and fulfilled, at least partially, the diagnostic criteria for RA or mixed connective tissue disease. He also might have benefited clinically from the previously prescribed therapies. However, an overlap syndrome-when a patient has a diagnosis of more than 1 rheumatologic disease at the same time-is considered rare.
Diagnostic/classification criteria
As this case exemplifies, diagnosis of rheumatologic disorders is not always accurate. These conditions can present a confusing picture-especially to physicians who might be practicing in a community setting and lack access to rheumatologists, rheumatology clinics, or other specialized resources.
The American College of Rheumatology (ACR) has established criteria for classifying RA.1 Although these criteria were developed to ensure that the diagnosis of RA is made according to standardized guidelines in research participants rather than in clinical patients, clinicians now use these criteria widely to make a diagnosis in individual patients. Keep in mind, however, that these criteria are empiric and are not meant to include or exclude a particular diagnosis in any given patient.1
According to the ACR criteria, a person is considered to have RA if he has satisfied at least 4 of the following 7 findings (criteria 1 through 4 must have been present for at least 6 weeks)1:
•Morning stiffness for at least 1 hour.
•Arthritis of at least 3 joints occurring simultaneously, with swelling or fluid accumulation (not bony overgrowth alone) observed by a physician. Areas of involvement are right or left PIP, metacarpophalangeal (MCP), wrist, elbow, knee, ankle, and metatarsophalangeal joints.
•Arthritis of the hand joints, with swelling in at least 1 of these areas: wrist, MCP joint, or PIP joints.
•Symmetrical arthritis, with simultaneous involvement of the same joint areas (see second bullet) on both sides of the body.
•Subcutaneous nodules present over bony prominences or extensor surfaces or in areas near the involved joints and observed by a physician.
•Positive RF, demonstrable by any method showing a positive result in fewer than 5% of controls.
•Radiographic features typical of RA on posteroanterior hand and wrist x-ray films. Films must show erosions or unequivocal bony decalcification localized in or most evident in areas adjacent to the involved joints.
MJ met only 3 of the 7 diagnostic criteria. Therefore, he did not qualify for a diagnosis of RA.
The Alarcon-Segovia2 diagnostic criteria for mixed connective tissue disease include a positive anti-U1 RNP hemagglutination titer of greater than 1:1600 and at least 3 of the following clinical features:
•Hand edema.
•Synovitis.
•Myositis.
•Raynaud phenomenon.
•Acrosclerosis.
MJ was negative for RNP. Therefore, he did not meet the criteria for mixed connective tissue disease.
The diagnostic criteria for scleroderma are a mixture of major and minor criteria. Patients must have the sole major criterion, proximal scleroderma, and 2 or more of the following minor criteria3:
•Sclerodactyly.
•Digital tip pitting.
•Loss of substance in the distal finger pads.
•Bibasilar pulmonary fibrosis.
Our patient clearly met these criteria. The Table compares the diagnostic criteria for RA, scleroderma, and mixed connective tissue disease.1-3
Discussion
Anti-Scl 70 antibodies are very useful for distinguishing systemic sclerosis from other connective tissue diseases; they are present in 15% to 20% of patients with systemic sclerosis.4 The specificity of this antibody in systemic sclerosis has been reported at 93%.5
Systemic sclerosis–RA overlap syndrome is a rare clinical phenomenon. Szucs and colleagues6 suggested that this may be a distinct genetic immunological and clinical entity. They found that RF and anti-Scl 70 antibodies are positive in 72.7% and 25% of their patients with systemic sclerosis–RA overlap syndrome, respectively. RF can be positive in up to 40% of patients who have scleroderma without RA overlap features.7
Our patient complained of dry mouth and dry eyes. These symptoms are common in scleroderma and may be related to fibrosis of the exocrine glands or concomitant Sjgren syndrome, which can occur in 20% of patients with systemic sclerosis.4 Of this patient subgroup, 30% to 50% have anti-Ro antibodies.4 The loss of RF during the later stages of Sjgren syndrome can predict the emergence of lymphoma years after the diagnosis of Sjgren is made.8
Consequences of misdiagnosis
They can be profound for patients. Although high-dose corticosteroid therapy has been shown to be beneficial in the management of RA,9 its use in patients with systemic scleroderma has been shown to be associated with the development of scleroderma renal crisis.10 Thus, we strongly discourage the use of high-dose corticosteroids in patients with early systemic scleroderma.
MTX administered weekly in low doses is a mainstay of RA management.11 However, its efficacy for managing arthritis or pulmonary fibrosis related to scleroderma is inconclusive.12
Conclusions
Diagnosis of rheumatological conditions can be confusing for those who lack extensive experience in rheumatology because there may be similarities in presentation among the various conditions. Familiarity with distinct diagnostic criteria for the diversified conditions is necessary, as this case demonstrates. Failure to recognize a condition can lead to misdiagnosis or a significant delay in diagnosis or initiation of the inappropriate therapy, possibly resulting in complications. Disease-modifying antirheumatic drugs are not indicated unless there is an active disease process with a favorable risk/benefit ratio.
References:
References1. Arnett FC, Edworthy SM, Bloch DA, et al. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum. 1988;31:315-324.
2. Alarcon-Segovia D, Cardiel MH. Comparison between 3 diagnostic criteria for mixed connective tissue disease. Study of 593 patients. J Rheumatol. 1989;16:328-334.
3. Subcommittee for Scleroderma Criteria of the American Rheumatism Association Diagnostic and Therapeutic Criteria Committee. Preliminary criteria for the classification of systemic sclerosis (scleroderma). Arthritis Rheum. 1980;23:581-590.
4. Ho KT, Reveille JD. The clinical relevance of autoantibodies in scleroderma. Arthritis Res Ther. 2003;5:80-93.
5. Aeschlimann A, Meyer O, Bougeois P, et al. Anti-Scl-70 antibodies detected by immunoblotting in progressive systemic sclerosis: specificity and clinical correlations. Ann Rheum Dis. 1989;48:992-997.
6. Szucs G, Szekanecz Z, Zilahi E, et al. Systemic sclerosis-rheumatoid arthritis overlap syndrome: a unique combination of features suggests a distinct genetic, serological and clinical entity. Rheumatology. 2007;46:989-993.
7. Pope JE. Musculoskeletal involvement in scleroderma. Rheum Dis Clin North Am. 2003;29:391-408.
8. Stobo JD, Traill TA, Hellmann DB, et al. The Principles and Practice of Medicine. 23rd ed. Stamford, CT: Appleton & Lange; 1996: 213.
9. American College of Rheumatology Subcommittee on Rheumatoid Arthritis Guidelines. Guidelines for the management of rheumatoid arthritis: 2002 update. Arthritis Rheum. 2002;46:328-346.
10. Steen VD, Medsger TA Jr. Case-control study of corticosteroids and other drugs that either precipitate or protect from the development of scleroderma renal crisis. Arthritis Rheum. 1998;41:1613-1619.
11. Cronstein BN. Low-dose methotrexate: a mainstay in the treatment of rheumatoid arthritis. Pharmacol Rev. 2005;57:163-172.
12. Pope JE, Bellamy N, Seibold JR, et al. A randomized, controlled trial of methotrexate versus placebo in early diffuse scleroderma. Arthritis Rheum. 2001;44:1351-1358.