Managing and preventing hip pathology in trochanteric pain syndrome
Greater trochanteric pain syndrome shares painpatterns with other musculoskeletal conditions, complicatingthe diagnosis and treatment. Many advances in evaluating andmanaging hip pathology have resulted in improved outcomes.Conservative treatment includes the use of NSAIDs for reducing pain.Physical therapy is combined with stretching of the iliotibial band andhip external rotators. Successful relief of trochanteric compartmentpain has been achieved with local anesthetic and corticosteroidinjections. Surgical management often results in significant improvementin refractory pain. There are several ways to work towardpreserving the integrity of the joint, especially maintaining anappropriate biomechanical relationship between the acetabular fossaand the femoral head. A diversified strength-training program isrecommended. (J Musculoskel Med. 2008;25:521-523)
Because greater trochanteric pain syndrome (GTPS) shares pain patterns with other musculoskeletal conditions, the diagnosis may not be made for several years. Patients may experience considerable pain and not see improvement in spite of having received several therapies. However, many advances in the evaluation and management of hip pathology have taken place in recent years, resulting in improved outcomes.
Painful hip conditions are being seen in increasing frequency in all age groups, usually in women after the fourth decade. Treatment often is directed toward conservative measures, with physical therapy and NSAIDs and, when appropriate, therapeutic injections into the trochanteric bursa. Pain not relieved by conservative means or not improved by injection of local anesthetic and corticosteroids should prompt the physician to the possibility of an incorrect diagnosis and a more thorough investigation into the source of pain. Pathologies often can be managed successfully with arthroscopic and open surgical approaches based on the patient's specific condition.
This 2-part article describes the diagnosis and management of hip pathology in GTPS. In the first part ("Evaluating hip pathology in trochanteric pain syndrome," The Journal of Musculoskeletal Medicine, September 2008, page 428), we focused on patient evaluation and the differential diagnosis. This second part discusses approaches to disease management and prevention.
MANAGEMENT
Nonsurgical management
Management of hip pathology centers on conservative treatment. NSAIDs may be of benefit in reducing pain. Icing the joint can provide some degree of relief. Physical therapy-in the form of strengthening of the hip abductors, adductors, and internal and external rotators; back extensors; and abdominals (the core)-is combined with stretching of the iliotibial band (ITB) and hip external rotators. The goal of stretching out the tissues is to relieve tension in the structures surrounding the greater trochanter and, as such, reduce friction. Local diathermy, iontophoresis, and pulsed ultrasonographic therapy for calcific tendinitis also have been successful in the management of trochanteric bursitis.1 Although pulsed ultrasonography has been used with success, there is concern about disruption to the tendon insertion during therapy.
Successful relief of trochanteric compartment pain has been achieved with local anesthetic and corticosteroid injections.2-5 Significant relief may be achieved with 1 or 2 injections.
The purpose of injection for trochanteric pain typically is to deposit the medication into the largest bursa between the overlying ITB and the underlying gluteus maximus tendons and the converging fibers of the gluteus medius and fascia along the lateral aspect of the trochanter. Specific injections into the smaller gluteal bursae have not been described.
Correct placement of the injection into the region also should take into account the possibility of direct injection into a tendon and the potential that this creates for tendon rupture because of intratendinous corticosteroid deposition. Pain not relieved by no more than 2 properly placed injections, significant weakness on testing, or a lack of success with physical therapy should raise suspicion of underlying pathology that requires more aggressive management or, more significantly, an incorrect diagnosis.
Surgical management
This often results in significant improvement in refractory pain (Figure). Open surgical management has been described. Division of the ITB is performed over the region of the greater trochanter. When indicated, partial tendon tears of the gluteus medius and minimus can be debrided and repaired. The primary bursa and the lesser bursa lying beneath the ITB can be evaluated and debrided. The cystic areas of the trochanter are debrided and the tendon or tendons reattached. Reduction osteotomy of the greater trochanter also has been described.6,7
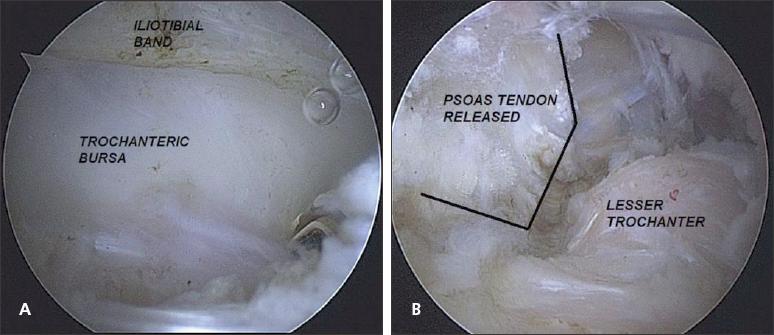
Figure –
In surgical management of trochanteric pain syndrome, the trochanteric bursa is released from the lateral aspect with small arthroscopic incisions (A).The psoas release is done from inside the hip joint after a hole is opened in the capsule (B).
Arthroscopic debridement of the trochanteric bursa may be accomplished in the supine or lateral decubitus position. Arthroscopic portals are marked at the anterior and posterior aspects of the greater trochanter. Depending on the surgeon's preference, the central compartment or peripheral compartment is entered initially and relevant structures are evaluated.8
Articular surfaces are visualized readily; osteochondral defects, chondromalacia, and the effects of osteoarthritis may be identified. Loose bodies resulting from these conditions can be removed.The fibrocartilaginous labrum and ligamentum teres are identified and, when appropriate, repair is accomplished. Synovitic changes and loose bodies may affect the biomechanical function of the joint. Impingement syndrome may result from these changes.
The lateral compartment lies beneath the ITB and along the greater trochanter. Once the compartment is entered, the ITB is visualized superiorly and the gluteal tendons and lateral trochanteric fascia attachments visualized inferiorly.
Inflamed bursa within the lateral compartment may have an appearance of synovitis or cobweb-like changes. The bursa can be remarkably thickened and may have a whitish to reddish appearance, possibly with synovial proliferation.
The tendon of the gluteus medius is seen along its anatomical insertion onto the greater trochanter, and the musculotendinous junction is clearly visualized. The gluteus minimus is inspected with the leg brought into internal rotation and slight abduction. Debridement of the tendons can then be accomplished or, if formal repair is indicated, a skilled arthroscopist may perform this technically difficult procedure. Complications from surgical treatment are similar to those that are experienced with other procedures.
When indicated, the final compartment with the iliopsoas bursa can be accessed. Inflamed bursa within this compartment may again have an appearance of synovitis or cobweb-like changes. Debridement can eliminate pathological pain resulting from this condition.
Postsurgery patients often can ambulate ad lib with assistive devices as indicated. If repair of the gluteal tendons has been performed, the patient follows a conservative protocol of weight bearing with an assistive device for 6 weeks. Then progressive strengthening of the hip is performed, including core strengthening and ITB stretching.
PREVENTION
What can patients do to protect their hips? Just as there are multiple potential causes of hip pathology, there are several ways to work toward preserving the integrity of the joint.
Foremost is maintaining an appropriate biomechanical relationship between the acetabular fossa and the femoral head. Normalization of postural alignment allows for nominal range of motion.9
Conceptualizing the lower extremities and pelvis as an arch helps illustrate the dynamics. The kinetic chain of the lower extremity functions as the legs of the arch; the pelvis and sacrum serve as the keystone.
From the base to the apex, the components that affect the alignment of that leg also can contribute to preserving the hip joint. When flat feet-congenital or acquired-are supported by an orthosis, the weight distribution through that joint will improve.
When training, patients should keep track of the mileage accumulated in the shoe. Because functional integrity degrades over time, manufacturer recommendations on the life span of the shoe should be heeded.2,10
Using appropriate-fitting footwear is another important prevention measure. If too much heel play is allowed within the shoe, there can be uneven weight distribution through the kinetic chain and subsequent deterioration of the hip joint.
Appropriate core strength and balanced musculature in the proximal leg affect postural stability. Therefore, they affect the alignment between the articular surfaces.9
Many training regimens that have been perpetuated through generations of coaches and personal trainers actually place the hip joint at risk. Correcting training misconceptions and errors would be a valuable prevention measure, but doing so would be a monumental undertaking and is beyond the scope of this article.
Almost any weight-training technique that places excessive force across the joint can result in pathology if performed incorrectly. A diversified strength-training program that includes sufficient cross training is recommended. Patients should train on even surfaces-the better the road, the less likely the fall. Nutritional supplementation with glucosamine and chondroitin sulfate has shown some subjective improvement in intra-articular symptoms in various studies.
References:
References
- 1. Schein AJ, Lehmann O. Acute trochanteric bursitis with calcification. Surgery. 1941;9:771-779.
- 2. Clancy WG. Runners’ injuries, part two: evaluation and treatment of specific injuries. Am J Sports Med. 1980;8:287-289.
- 3. Larsson LG, Baum J. The syndromes of bursitis. Bull Rheum Dis. 1986;36:1-8.
- 4. Crevenna R, Kéilani M, Wiesinger G, et al. Calcific trochanteric bursitis: resolution of calcifications and clinical remission with non-invasive treatment: a case report. Wien Klin Wochenschr. 2002;114:345-348.
- 5. Kagan A 2nd. Rotator cuff tears of the hip. Clin Orthop Relat Res. 1999;368:135-140.
- 6. Glassman AH. Complications of trochanteric osteotomy. Orthop Clin North Am. 1992;23:321-333.
- 7. Zoltan DJ, Clancy WG Jr, Keene JS. A new operative approach to snapping hip and refractory trochanteric bursitis in athletes. Am J Sports Med. 1986;14:201-204.
- 8. Bradley DM, Dillingham MF. Bursoscopy of the trochanteric bursa. Arthroscopy. 1998;14:884-887.
- 9. Willson JD, Dougherty CP, Ireland ML, Davis IM. Core stability and its relationship to lower extremity function and injury. J Am Acad Orthop Surg. 2005;13:316-325.
- 10. Butcher JD, Salzman KL, Lillegard WA. Lower extremity bursitis [published correction appears in Am Fam Physician. 1996;54:468]. Am Fam Physician. 1996;53:2317-2324.