The Burden of Comorbidities Weigh Differently on PsA and AS Patients
High levels of comorbidity burden are associated independently with poor physical function and increased disability in patients with psoriatic arthritis, however, patients ankylosing spondylitis did not report worse function when comorbidities were present.
(©MedicalIllustrations.com)
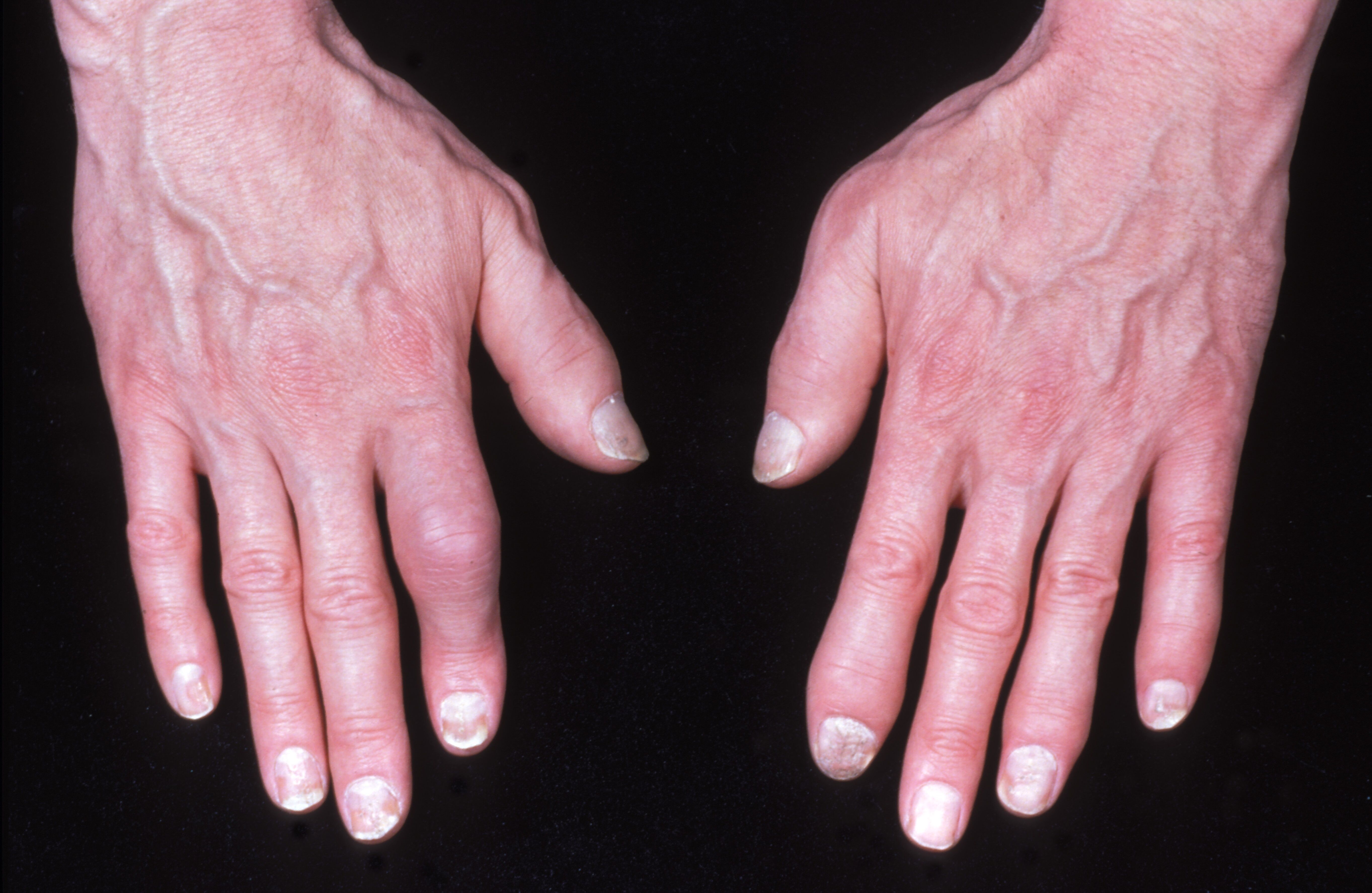
High levels of comorbidity burden are associated independently with poor physical function and increased disability in patients with psoriatic arthritis, however, patients ankylosing spondylitis did not report worse function when comorbidities were present.
“We believe that comorbidity may also exert some negative influence in the physical function of PsA (psoriatic arthritis) patients and our results support this view. In this case, the measurement of physical function would reflect not only the disease process but also other factors related to the patients’ general health,” wrote authors who were led by Miguel Gonzalez-Gay, M.D., Ph.D., of The Hospital Universitario Marqués de Valdecilla in Spain. The findngs appear in the April 29 issue of Arthritis Care and Research.
Physical function is a key measure in patients with spondyloarthritis with functional improvement being one of the primary goals of treatment. It is well known that patients with ankylosing spondylitis, a form of spondyloarthritis primarily affecting the spine, have increased cardiovascular comorbidities as well as higher rates of osteoporosis.
Similarly, patients with psoriatic arthritis have an increased incidence of cardiovascular disease, diabetes, and depression with greater than half having more than one comorbidity at a time.
While limitations in physical function have been associated with both ankylosing spondylitis and psoriatic arthritis, it is not well understood what portion of the disability is directly related to disease activity and structural damage, and how much is due to other factors including non-rheumatic comorbidities.
The authors sought to determine the impact of comorbidities on physical function in Spanish patients with ankylosing spondylitis and psoriatic arthritis in an effort to understand the relative contribution their rheumatic disease activity influences their perception of physical function.
The authors conducted a cross-sectional study looking at data from the Cardiovascular in rheumatology project (CARMA). 738 patients with ankylosing spondylitis and 721 with psoriatic arthritis were included in the protocol with the primary outcome being physical function as determined by the Bath Ankylosing spondylitis function index and the Health Assessment Questionnaire.
Comorbidities were recorded, and disease activity was determined utilizing established and validated measures including radiographic damage such as spinal radiographic changes for ankylosing spondylitis and the presence of erosions for psoriatic arthritis radiographs.
Patients with ankylosing spondylitis and other comorbidities did not report worse physical function when compared to those without other comorbidities. Psoriatic arthritis patients did report worse physical function with increasing numbers of comorbidities.
Poor physical function was directly associated with increasing age, female sex, longer disease duration, higher disease activity and spinal radiographic damage in ankylosing spondylitis patients. Spondylitis patients taking disease modifying anti-rheumatic drugs, non-steroidal anti-inflammatory drugs and glucocorticoids were more likely to have worse physical function. No association was found between physical function and comorbidity burden.
In the psoriatic arthritis cohort, a significant and independent association was found between comorbidity burden and poor physical function. Female sex, longer disease duration, higher disease activity, the use of disease modifying anti-rheumatic drugs, non-steroidal anti-inflammatory drugs and glucocorticoids were also associated with worse physical function in psoriatic arthritis.
Take-home points for clinicians and final thoughts
Contrary to what one might expect, the presence of comorbidities in patients with spondyloarthritis actually decreases reports of diminished physical function.
Conversely, increasing comorbidity burden in patients with psoriatic arthritis led to greater disability. However, psoriatic arthritis patients were more frequently obese which reduces the chances of achieve minimal disease activity on drug therapy.
Clinicians should encourage patients with psoriatic arthritis and ankylosing spondylitis even more so to quit smoking along with other behavior modifications aimed at reducing the risk and burden of comorbid conditions.
While disease activity and radiographic damage were strongly implicated in physical function deterioration in patients with psoriatic arthritis the authors state, “We believe that comorbidity may also exert some negative influence in the physical function of PsA (psoriatic arthritis) patients and our results support this view.”
With newer remission-inducing therapies available, understanding the different causes of disability in both psoriatic arthritis and spondyloarthritis are even more relevant. Clinicians should strive to recognize and treat the comorbid conditions that overshadow the outcomes of their patients suffering from rheumatic disease.
REFERENCES
Cristina Fernandez-Carballido, Maria A. Martin-Martinez, Carmen Garcia-Gomez, et al. "Impact of Comorbidity on Physical Function in Patients with Ankylosing Spondylitis and Psoriatic Arthritis Attending Rheumatology Clinics. Results from the Cardiovascular in rheumatology (CARMA) study." Arthritis Care Res (Hoboken). 2019 Apr 29. doi: 10.1002/acr.23910.
Bremander A, Petersson IF, Bergman S, Englund M. Population-based estimates of common comorbidities and cardiovascular disease in ankylosing spondylitis. Arthritis Care Res (Hoboken) 2011; 63: 550-6. â¨
Ogdie A, Schwartzman S, Husni ME. Recognizing and managing comorbidities in psoriatic arthritis. Curr Opin Rheumatol 2015; 27: 118-26.
Lupoli R, Pizzicato P, Scalera A, Ambrosino P, Amato M, Peluso R, Di Minno MN. â¨Impact of body weight on the achievement of minimal disease activity in patients with rheumatic diseases: a systematic review and meta-analysis. Arthritis Res Ther 2016; 18: 297. â¨