Immunotherapy for Lupus? Here's the Scoop
UK researchers say that having "switched off" autoimmunity in a mouse model of multiple sclerosis holds out new hope for lupus patients, among others. What can you say about it to those who hopefully inquire?
Heat maps of T cell gene action. Credit: U. of Bristol/Bronwen Burton
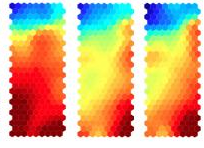
Burton BR, Britton GJ, Fang H, et al.Sequential transcriptional changes dictate safe and effective antigen-specific immunotherapy. Nature Communications (2014) 5:4741 doi:10.1038/ncomms5741
Thisstudy in Nature Communications raised a flutter last week on social media after many news outlets printed verbatim a press release calling this a “breakthrough”for people with multiple sclerosis (MS) as well as systemic lupus erythematosus and other autoimmune conditions.
The study tweaks a dose escalation protocol for myelin basic protein (MBP) in the mouse experimental autoimmune encephalomyelitis (EAE) model of MS, creating tolerance in this model by switching T helper cells into T regulatory cells.
This technique is at least 20 years old (see Regulatory T cell clones induced by oral tolerance: suppression of autoimmune encephalomyelitis, Chen Y et al. Science 1994). What’s new here is administering the MBP subcutaneously rather than intranasally.
The researchers from the University of Bristol UK (the source of the press release) have spun off a company called Apitope to develop the technology.
Besides working in mouse models of MS, allergenic desensitization has sometimes worked in humans. A phase 2 trial published in 2006 treated progressive MS with a fragment of human MBP. For a large subset of patients, MBP increased median time to progression to 78 months rather than 18 months in the placebo group. In another report, intravenous synthetic peptide MBP8298 delayed disease progression in an HLA Class II-defined cohort of patients with progressive MS.
Desensitization has also been effective in some mouse models of rheumatoid arthritis and type 1 diabetes.
As to lupus, in a 2012 review of immune tolerance and similar therapies for autoimmune disease, clinician-authors from the University of California-San Francisco cite one 2008 trial from Bulgaria in which injections of a protein fragment that reduced lupus-like symptoms in mice seemed to have a positive effect among humans. Those researchers have not published further on the topic.
Authors of the review observe the important challenges to this approach:
• lack of knowledge of the dominant antigens that drive most autoimmune conditions;
• differences in these antigens over time and between patients; and
• the possibility that administering them would exacerbate the disease.