Managing Calcium Extravasation–Related Injuries
Extravasation of calcium solutions may result in subcutaneous calcinosis, also known as calcinosis cutis. A patient had rhabdomyolysis followed by acute renal failure and received calcium supplementation for hypocalcemia.
ABSTRACT: Extravasation of calcium solutions may result in subcutaneous calcinosis, also known as calcinosis cutis. A patient had rhabdomyolysis followed by acute renal failure and received calcium supplementation for hypocalcemia. Although his calcium levels normalized, multiple subcutaneous indurated plaques developed over his infusion site, even though there was no evidence of leakage. The patient's lesions improved spontaneously over time, with no specific treatment and no complications. Extravasation of calcium may cause injury to subcutaneous tissue with several mechanisms, and various factors determine the extent of damage. Taking preventive measures is the most important step in avoiding calcium infusion–related complications. If the injury is detected early, the best treatment options are light compression dressing and immobilization and elevation of the limb. (J Musculoskel Med. 2011;28:339-341)
_______________________________________________________________________________________
Extravasation of calcium solutions may result in subcutaneous calcinosis, or calcinosis cutis, the deposition of calcium salt in subcutaneous tissue. Because knowledge about the diagnosis and management of calcium extravasation–related injuries is limited, we offer a case report with discussion. In most cases, calcinosis is associated with hypercalcemia or hyperphosphatemia, but in this case it was related to infusion of calcium chloride.
CASE PRESENTATION
FIGURE
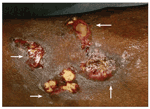
Three days after the patient presented with acute renal failure and rhabdomyolysis, white-yellow plaques with irregular but well-defined borders developed over the infusion site on his left forearm (arrows)
A 37-year-old man presented with acute renal failure and rhabdomyolysis, the rapid breakdown of skeletal muscle fibers, which results in the release of muscle fiber contents into the bloodstream. Some proteins, such as myoglobin, may be toxic to the kidneys and cause acute renal failure.
Because our patient had hypocalcemia, he received 10 mL of 10% calcium chloride twice a day,1 infused over 45 minutes, for 2 days, through an intravenous line placed on the ventral aspect of his left forearm. The patient did not complain of pain or swelling during the infusion. The cannula was patent; intravenous fluids were given through the same cannula for another 24 hours after the calcium infusion.
Three days later, multiple lesions developed over the patient's left forearm (Figure). The lesions were 1- to 3-cm white-yellow indurated plaques with irregular but well-defined borders.2-7
The patient's serum calcium, phosphate, and parathyroid hormone levels were within the normal range. X-ray films revealed calcium in the subcutaneous tissue.
The lesions resolved gradually over 3 weeks with conservative treatment and dressing.5 There were no subsequent complications.
DISCUSSION
These injuries typically can be identified in scenarios similar to the one described in this case. The lesions appear within 2 weeks. They are described as white-yellow papules, plaques, and nodules, often multiple, with or without erythema, necrosis, or ulceration. They tend to resolve without residual deformity within 2 to 6 months with local wound care.
There are several mechanisms by which extravasation of calcium may cause injury to subcutaneous tissue; various factors determine the extent of damage. Damage may vary with the type, osmolality, and nature of the agent; the amount of dose extravasated or deposited in the subcutaneous tissue; and the pressure involved during the infusion.
The extent of damage also varies with tissue characteristics, such as anatomic specificity, toxicity and pressure, and vasospecificity. Some factors that influence the degree of injury are patient-dependent, such as age and the presence or absence of hypoproteinemia, anemia, vitamin deficiency, and electrolyte imbalance. All of these factors act in synchrony and contribute to causing the injury.
Pathogenesis, mechanism of injuries
Calcium may cause damage by multiple mechanisms. The most frequently used forms of calcium solutions are hypertonic solutions, in which the calcium is present in an ionized form. Ionized calcium may induce osmotic imbalance across the cell membranes, which inhibits cell transportation mechanisms, which, in turn, causes intracellular fluid retention, leading to cell death.
Normal serum osmolality is 280 mOsm/L, and osmolality of the 2 most commonly used calcium preparations, calcium gluconate and calcium chloride, is 669.60 mOsm/L and 2040 mOsm/L, respectively, pointing toward the hypertonic nature of calcium solutions. Calcium also causes prolonged depolarization and contraction of capillaries around the smooth muscles, resulting in ischemic necrosis. Precipitation of cellular proteins resulting from the direct toxic effects of calcium also occurs because of its acidic and hypertonic nature, leading to cell death. It has been observed that collagen can trigger calcium phosphate deposition.5
Extravasation at the infusion site causes increased hydrostatic pressure, resulting in increased interstitial pressure, venous compression and, ultimately, arterial compromise. However, it has been observed that transient increases in local calcium concentrations (resulting from the very high concentration of the calcium infusions) and local trauma are sufficient to cause infusion-related injuries.8 Extravasation is not a prerequisite for complications to occur.
Prevention
Taking preventive measures is the most important step in avoiding calcium infusion–related complications. Preventing phlebitis by properly screening intravenous lines to limit mechanical damage to the vein is key. Multiple perforations of the same vein and repeated use of the same vein should be avoided by rotating infusion sites.9 It is also important to check for backflow before infusion is started, avoid injections into an obviously compromised infusion line, and terminate infusion immediately at the earliest sign of infiltration.
Always try to infuse a dilute calcium solution continuously to avoid intravenous push methods and possibly decrease extravasation. Infusion should always be given at a slow rate and without any pressure. Any pressure proximal to the point of cannulation should be avoided.
During prolonged anesthesia and resuscitation, all venipuncture sites should be monitored carefully. Large central veins should be monitored during prolonged resuscitative efforts. When possible, the use of oral supplements is recommended.
Treatment
If the injury is detected early, the best treatment options are light compression dressing and immobilization and elevation of the limb. In cases of arterial compromise or compression syndromes, fascial decompression and debridement are undertaken. In terminally ill patients, debridement is not an option; for these patients, treatment consists of elevation, antibiotics, night splinting, and daily motion exercises.
Wounds are covered using biologic dressings and split-thickness skin grafts and flaps. Treatment may be multistage in debilitated patients.
Rarely used treatment modalities include local injections of sodium sulfate, cellulose phosphate, and triamcinolone acetonide.6,10 However, the effectiveness of these local injections is unclear.
SUMMARY
Subcutaneous calcinosis often occurs as a result of hypercalcemia or hyperphosphatemia, but it may occur as a complication of intravenous calcium administration. Treatment is conservative, and patients usually achieve full recovery.
Comments about/problems with this article? Send feedback.
References:
References
1. Johnson RC, Fitzpatrick JE, Hahn DE. Calcinosis cutis following electromyographic examination. Cutis.1993;52:161-164.
2. Jucglà A, Sais G, Curco N, et al. Calcinosis cutis following liver transplantation: a complication of intravenous calcium administration. Br J Dermatol. 1995;132:275-278.
3. Berger PE, Heidelberger KP, Poznanski AK. Extravasation of calcium gluconate as a cause of soft tissue calcification in infancy. Am J Roentgenol Radium Ther Nucl Med. 1974;121:109-117.
4. Caksen H, Odabas D. An infant with gigantic subcutaneous calcium deposition following extravasation of calcium gluconate. Pediatr Dermatol. 2002;19:277-279.
5. Goldminz D, Barnhill R, McGuire J, Stenn KS. Calcinosis cutis following extravasation of calcium chloride. Arch Dermatol. 1988;124:922-925.
6. Hironaga M, Fujigaki T, Tanaka S. Cutaneous calcinosis in a neonate following extravasation of calcium gluconate. J Am Acad Dermatol. 1982;6:392-395.
7. Kagen MH, Bansal MG, Grossman M. Calcinosis cutis following the administration of intravenous calcium therapy. Cutis. 2000;65:193-194.
8. Leonard F, Boke JW, Ruderman RJ, Hegyeli AF. Initiation and inhibition of subcutaneous calcification. Calcif Tissue Res. 1972;10:269-279.
9. Lynch DJ, Key JC, White RR 4th. Management and prevention of infiltration and extravasation injury. Surg Clin North Am. 1979;59:939-949.
10. Ahn SK, Kim KT, Lee SH, et al. The efficacy of treatment with triamcinolone acetonide in calcinosis cutis following extravasation of calcium gluconate: a preliminary study. Pediatr Dermatol. 1997;14:103-109.
2 Commerce Drive
Cranbury, NJ 08512
All rights reserved.