Nurse Practitioner Q&A: Clues to Psoriatic Arthritis
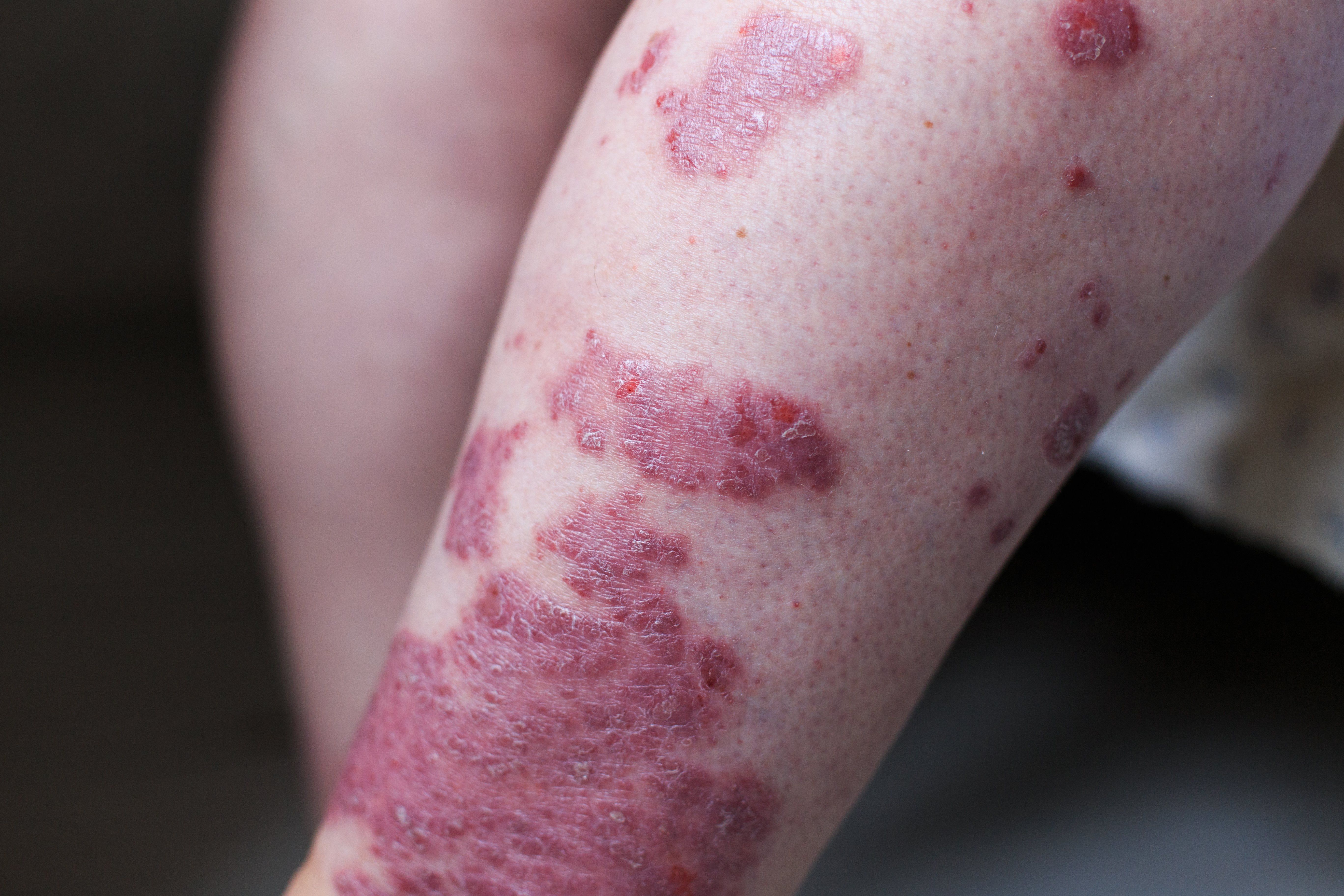
Psoriatic arthritis can manifest in a variety of ways from nail disease to peripheral joint pain. But, there are a few hallmark signs that can point a rheumatologist or rheumatology nurse in the right direction. In a presentation given at the Rheumatology Nurses Society annual meeting in August, Linda Grinnell-Merrick, NP, an allergy, immunology, and rheumatology nurse practitioner at the University of Rochester Medical Center, discussed the treatment of psoriatic arthritis.
Psoriatic arthritis can manifest in a variety of ways from nail disease to peripheral joint pain. But, there are a few hallmark signs that can poinit a rheumatologist or rheumatology nurse in the right direction. (©ОльгаТернавская,AdobeStock)
Linda L. Grinnell-Merrick, NP

When a patient comes into the rheumatology office with complaints of joint pain and inflammation, the exact diagnosis is rarely immediately evident. Arthritis can take many forms and figuring out which kind an individual patient has can be vital to identifying the proper treatment strategies.
Psoriatic arthritis can manifest in a variety of ways from nail disease to peripheral joint pain. But, there are a few hallmark signs that can point a rheumatologist or rheumatology nurse in the right direction. In a presentation given at the Rheumatology Nurses Society annual meeting in August, Linda Grinnell-Merrick, NP, an allergy, immunology, and rheumatology nurse practitioner at the University of Rochester Medical Center, discussed the treatment of psoriatic arthritis.
In this Q&A, Ms. Grinnell-Merrick discusses some messages from her presentation.
Why is it important to discuss the diagnosis and treatment of psoriatic arthritis?
“Psoriatic arthritis is under the umbrella of spondyloarthropathies. It’s important for nurses, doctors, pharmacists, and advanced practice providers to understand how it’s different from rheumatoid arthritis, as well as how it affects the spine, peripheral joints, nails, and the skin. Patients can have dactylitis, enthesitis, or problems with a variety of domains. It can be overwhelming to healthcare providers who are looking at it.
Psoriatic arthritis can affect anyone. You really have to be on the look out and be aware that it doesn’t always present as psoriasis and joint symptoms. Patients could just have nail disease and enthesitis. Providers hope that patients are easy to diagnose with psoriasis and bad joints, but psoriatic arthritis is a puzzle that you have to put together. But, it can be a fun puzzle when you’re investigating further.”
As a condition that can be easily misidentified, how is it different and what are some characteristics that could point providers in the right direction?
“This condition affects the distal joints of the fingers, particularly the DIP joint - the distal interphalangeal joint. That makes it completely different from rheumatoid arthritis. The only other time that symptom shows up is with osteoarthritis. People can also have axial disease, and they might have some sacroiliac joint inflammation. Dactylitis is a ‘bingo.’ If a patient presents with a complete digit that’s completely swollen so that it looks like a little sausage, that helps with diagnosis. You know you can identify psoriatic arthritis immediately that way.
Even a small amount of psoriasis or presentation with prolonged stiffness or joint pain can be a good clue, particularly if it affects a larger joint in a lower extremity. Those are probably the easiest to identify more so than if someone presents with more enthesitis symptoms.”
Even with a few red flags, what challenges remain when tackling psoriatic arthritis, and how can they be met?
“Diagnosis itself can be challenging if patients aren’t presenting in an easy format. But, the patients themselves can sometimes present a challenge. Maybe they’re not having their psoriasis followed followed by a primary care physician. Or, in many cases, they might not think about talking to their primary care physician or a dermatologist about their joint symptoms. That can create significant issues because they end up coming to someone in rheumatology a little bit too late.
Even still, if you suspect an inflammatory arthritis, you’re probably not going to go wrong with initiating treatment because some of our drugs overlap. It’s not that you’ve done someone wrong because you didn’t get the exact diagnosis, and you’re not going to do harm.
Providers need to be as familiar as they can be with the different domains and the different areas that can be affected by psoriatic arthritis. If you’re treating these patients, you need to consider that there might be some treatments that are more effective for skin diseases and some that are more effective for joints. You need to match your treatment with what the patient is actually presenting that’s most obvious. Treatment matching can be tough, though, because it comes from knowing the research and what’s behind it. You have to read up on the drugs and what might help certain symptoms.”
What are your take-away messages?
“The No.1 thing that we’re all probably hoping for is to initiate treatment for early recognition so we can possibly prevent long-term joint damage. But, it’s not always easy because it can take forever to get into a rheumatology practice these days. Overall, it’s important to be aware of all the domains that can be affected by psoriatic arthritis. Look for them and be sure to ask patients questions regarding it. And, be on the look out for associated co-morbidities, such as depression and high-risk cardiovascular disease. Ask patients how long they’ve had their symptoms, what joints bother them, how long it takes them to get moving in the morning, and how it might impact their daily activities. Ask about other symptoms they might not have already shared or if they’ve had recent infections.
I really just want people to understand about this disease, the domains, and the parts of the body that it affects. Do what you can to make sure you’re getting the right treatment for the patient whether it’s NSAIDs or getting them physical therapy. Just make sure they’re getting in front of a rheumatology provider and that we’re monitoring them.”