RA Progression and Comorbidities: A Photo Essay
Rheumatoid arthritis can lead to permanent destruction of synovial joints: loss of cartilage and bone, damage to ligaments and tendons, and loss of physical function. Tuberculosis, vasculitis, and pyoderma gangrenosum are among the comorbidities you may recognize in these images.
Rheumatoid arthritis usually involves the MCP, PIP, and MTP joints before the larger joints. In its early stage, RA affects the synovial membranes and periarticular structure of multiple joints, which results in swelling, pain, and inflammation. No destructive changes are seen on radiographic examination at this stage.. Read the full case.
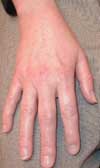
Photo courtesy of Eugene Mochan, DO, PhD
Patients with moderate RA typically have diffuse swelling and limited joint mobility without joint deformities. Extra-articular nodules and tenosynovitis may develop. Radiographic findings include periarticular osteopenia and minor cartilage destruction. The review including these images discusses management of rheumatoid arthritis.
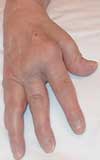
Photo courtesy of Eugene Mochan, DO, PhD
Advanced RA is characterized by severe cartilage and bone destruction (such as marginal joint erosions) that results in joint deformity (eg, subluxation, ulnar deviation, and bony ankylosis). Inflammatory joint symptoms appear to be the main determinants of disability early in the disease, while joint destruction, measured radiographically, dominates late disease. Read here about differential diagnosis of RA.
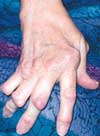
Photo courtesy of Eugene Mochan, DO, PhD
The use of preserved artificial tears several times a day provided little relief to this 54-year-old woman with red and painful eyes. The patient had a history of rheumatoid arthritis and dry eye syndrome; the latter is very common in patients with RA. Read the full case.
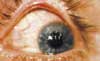
Photo courtesy of Leonid Skorin, Jr, DO
Tuberculosis was diagnosed in this patient with a history of rheumatoid arthritis who had been taking one of the TNF inhibitors (infliximab, etanercept, adalimumab) used to reduce the erosive damage of the RA. Neutralization of TNF significantly suppresses the immune response, and has led to an increased risk of such infections as TB, Pneumocystis infection, and disseminated histoplasmosis. Read the full case.
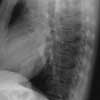
Photo courtesy of Navin M.Amin, MD
This solitary, rapidly expanding, very painful ulcer developed on the pretibial surface of the leg of a 48-year-old woman with seropositive rheumatoid arthritis. The ulcer location, visibly rolled undermined border, and degree of pain are all typical for pyoderma gangrenosum. Read the full case.
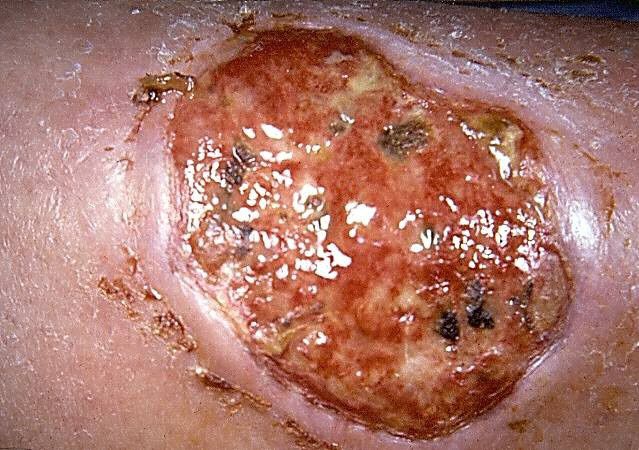
Photo courtesy of Ted Rosen MD
A 55-year-old woman noticed decreased sensation in her feet and a bluish discoloration of her toes that progressed rapidly, along with increasing pain and coldness in both feet. Her seropositive arthritis had been well controlled until about 10 weeks before this photograph was taken. It is a particularly good depiction of the livedo reticularis pattern that often indicates vasculitis. Read the full case.
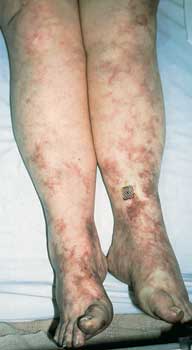
Photo courtesy of David I. Wolf, MD
Rheumatoid nodules are found in approximately one third of patients with rheumatoid arthritis. Usually, they are associated with more severe disease and a high rheumatoid factor titer. Most often located over bony prominences or extensor surfaces-notably on the forearms, elbows, knuckles, feet, and knees-the nodules tend to be deep and asymptomatic. Read the full case.
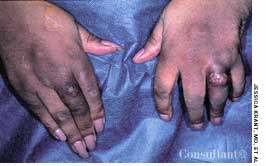
Photo courtesy of Jessica Krant, MD and Yelva Lynfield, MD