A Woman With Osteoporosis, Ulcerative Colitis, and NSAID-Resistant Muscle Pain
A 79-year-old white woman presented with ulcerative colitis of 12 years’ duration and osteoporosis. She was referred to rheumatology for severe proximal muscle pain that was unresponsive to NSAID therapy.
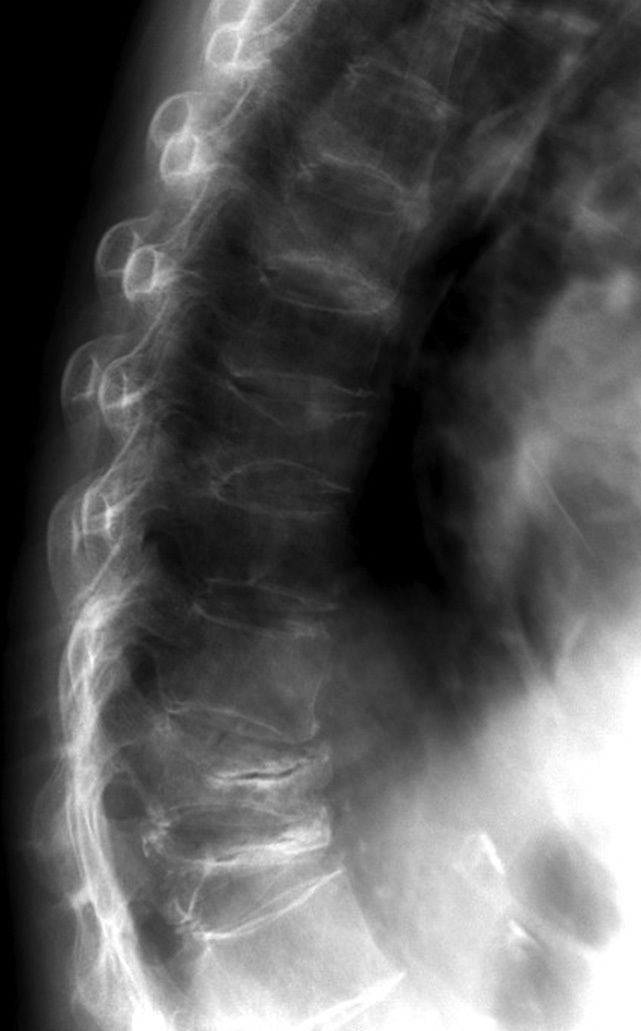
A 79-year-old white woman presented with ulcerative colitis of 12 years’ duration and osteoporosis as identified by dual-energy x-ray absorptiometry (DEXA) (T-scores, _2.3 in the lumbar spine and _2.9 in the total hip). Her ulcerative colitis had been well controlled with a regimen of azathioprine and mesalamine. Before starting this regimen, she had been receiving long-term corticosteroid therapy until about 3 years before presenting to our clinic.
The patient was referred to rheumatology for severe proximal muscle pain that was unresponsive to NSAID therapy. Results of her physical examination showed no synovitis, rash, or weakness.The patient’s erythrocyte sedimentation rate was 85 mm/h (normal, 0 to 20 mm/h).A clinical diagnosis of polymyalgia rheumatica (PMR) was made.
The image at left is an x-ray of her spine taken as part of screening for an institutional corticosteroid-induced osteoporosis program.
What is your diagnosis?
(Find the answer on the next page.)
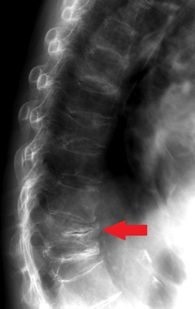
This x-ray film obtained for our patient with corticosteroid-induced osteoporosis showed osteopenia and multiple vertebral compression fractures. In addition, a horizontal lucency of the T12 vertebral body was seen (arrow), showing evidence of osteonecrosis. The findings noted in our patient represent late-stage osteonecrosis.
Early disease might not be appreciated on plain x-ray films, and MRI would be a preferred study for patients in whom early osteonecrosis is suspected clinically.
Osteoporosis is a chronic disease characterized by a generalized loss of bone mass and bone strength. Osteonecrosis is a destructive process that involves disruption of blood flow and alterations in intraosseous pressures that ultimately lead to structurally impaired bone. Although both conditions are associated with longterm use of corticosteroids, they rarely have been reported coincidentally in the vertebrae.4
This case illustrates 2 points: (1) development of significant spinal compression deformities in the setting of corticosteroid therapy may be clinically silent and (2) osteonecrosis may be present in the vertebrae of an asymptomatic patient with osteoporosis.These points emphasize that the absence of pain in osteoporosis or in long-term corticosteroid use is not a good indicator of disease progression or severity and may provide a physician with a false sense of security about a patient’s bone health.
In other reports, up to 60% of vertebral fractures in patients with osteoporosis are asymptomatic.3 These fractures, in turn, carry an associated increase in mortality, which ranges from 19% to 60% compared with the nonfractured population.2 In addition, 1 in 5 persons with vertebral fractures go on to experience another fracture within 1 year (a 4-fold increased risk compared with the general population).3
The sequelae of these osteoporotic vertebral fractures may be dramatic.There may be a loss of height, compression of abdominal and thoracic contents, respiratory dysfunction , and decreased mobility. The diagnosis of vertebral fractures-the most common osteoporotic fractures- presumably is made in only a few cases, possibly because of their painless nature and the confounding high prevalence of low back pain in the general population. Further complicating the diagnosis is a lack of radiographic evidence of osteoporosis until about 20% to 30% of total body calcium is lost.2 Although the presence of osteopenia is a subjective assessment, it should prompt further investigation.
Suggestive of more long-standing osteoporosis are objective measures of osteoporosis, such as biconcavity or anterior wedging of vertebral bodies and, as in this case, the radiographic finding of a central lucency within a vertebral body. These findings should prompt consideration of further investigation and initiation of therapy.
The pathophysiology of osteoporosis and subsequent fracture risk are a function of bone strength, which is found in the lamellar arrangement of collagen fibers and horizontal and vertical cross connections (struts). During a lifetime, bone continually is remodeled in a process of osteoclastic resorption, which is matched by osteoblastic deposition. With age, however, the remodeling process changes to favor the osteoclasts, leaving less bone over time and, thereby, more potential for fracture. For every standard deviation reduction in bone mineral density (BMD), fracture risk approximately doubles.1 Other factors influence fracture risk independent of BMD; these include age, family history, fracture history, body weight, cigarette smoking, and corticosteroid use.
Spinal osteonecrosis is a rarely reported complication of advanced osteoporosis. Previous studies have suggested that the fractures that are associated with osteoporosis could themselves predispose patients to osteonecrosis of the vertebrae by interrupting blood flow. Conversely, others have suggested that fractures could be the consequence of osteonecrosis.5,6
Although the exact chronology is difficult to assess in any given case, our patient’s case lends credence to a correlation among corticosteroid use, osteoporosis, vertebral fracture, and even vertebral osteonecrosis. Because vertebral fracture and osteonecrosis are not reversible phenomena, this case illustrates that the best therapy for osteoporosis is prevention. This requires optimal monitoring with BMD testing (given the silent nature of the disease) and pharmacologic intervention at an early stage.
In our patient’s case, we could see the degree of damage that is possible in the absence of clinical warning signs. As a result, we can see the importance of diligent assessment and attention to risk factors, especially in corticosteroid users.
Pharmacologic intervention will not reverse our patient’s current condition, but it has been shown to retard corticosteroid-induced bone loss and reduce fracture risk.7-13 Medications that have been used for osteoporosis include bisphosphonates (alendronate, risedronate, and ibandronate), selective estrogen receptor modulators (raloxifene), hormone replacement therapy, calcitonin and, most recently, teriparatide. Physicians should screen patients for subclinical vitamin D deficiency, especially older and corticosteroid-treated patients. Appropriate intake of calcium, weight-bearing exercise, and avoidance of cigarette smoking and alcohol intake form the cornerstone of a comprehensive treatment strategy. Assessing fall risk and the use of walking aids also is important.1-3,7-9
Our patient was placed on anabolic therapy with teriparatide; she also received calcium and vitamin D supplementation. She has not sustained any new fractures to date, and her T-scores on repeated DEXA scanning have shown improvement. However, she has continued to experience back pain. She has used acetaminophen and short-acting opioid analgesics and has had only moderate success.
This case was reported by David Pugliese, DO, and Thomas Olenginski, MD. Dr Pugliese is a fellow and Dr Olenginski is associate staff in the department of rheumatology at Geisinger Health System in Danville, Pennsylvania.
References:
1. Eastell R. Pathogenesis of postmenopausal osteoporosis. In: Favus MJ, ed. Primer on the Metabolic Bone Diseases and Disorders of Mineral Metabolism. 4th ed. Philadelphia: Lippincott Williams and Wilkins; 1999:260-262. 2. Russell G. Pathogenesis of osteoporosis. In: Hochberg MC, Silman AJ, Smolen JS, et al, eds. Rheumatology. 3rd ed. London: Mosby; 2003: 3. Delaney MF, LeBoff MS. Metabolic bone disease. In: Ruddy S, Harris ED Jr, Sledge CD, eds. Kelley’s Textbook of Rheumatology. 6th ed. Philadelphia: WB Saunders Co; 2001:1635-1652. 4. Resnick D, Niwayama G, Sweet DE, Madewell JE. Osteonecrosis. In: Resnick D, Niwayama G, eds. Diagnosis of Bone and Joint Disorders. Philadelphia: Saunders; 1981:959-978. 5. Dupuy DE, Palmer WE, Rosenthal DI. Vertebral fluid collection associated with vertebral collapse. AJR. 1996;167:1535-1538. 6. Antonacci MD, Mody DR, Rutz K, et al. A histologic study of fractured human vertebral bodies. J Spinal Disord Tech. 2002;15:118-126. 7. Homik J, Cranney A, Shea B, et al. Bisphosphonates for steroid induced osteoporosis. Cochrane Database Syst Rev. 2000;(2): CD001347. 8. Homik J, Suarez-Almazor ME, Shea B, et al. Calcium and vitamin D for corticosteroid induced osteoporosis. Cochrane Database Syst Rev. 2000;(2):CD000952.