Managing hip pain in athletes
Hip injuries are common in dancers, runners, and soccer players. Knowledge of the mechanism of injury and the sport can help uncover the diagnosis. Muscular strength testing should be performed on the cardinal movements of the hip joint.
Hip injuries are fairly common, accounting for roughly 5% to 6% of musculoskeletal complaints in adults and 10% to 24% of complaints in children.1 These injuries are particularly common in certain athletes, such as dancers, runners, and soccer players, because their sports activities involve a high degree of increased force and extremes of movement across the hip.
A wide variety of disorders can result in hip pain in athletes. Evaluation of hip injuries varies significantly with the patient's age and activity and the type of injury and its severity.
In this 2-part article, we discuss the evaluation, possible causes, and initial treatment of hip and pelvis injuries in young adult and mature athletes. This first part focuses on the history, physical examination, and several diagnoses commonly seen in these athletes. In the second part, to appear in a later issue of this journal, we will take a closer look at some additional soft tissue injuries that may be seen in athletes who present with hip complaints.
PATIENT EVALUATIONAnatomy
The hip joint has a ball and socket configuration that allows for significant stability and mobility
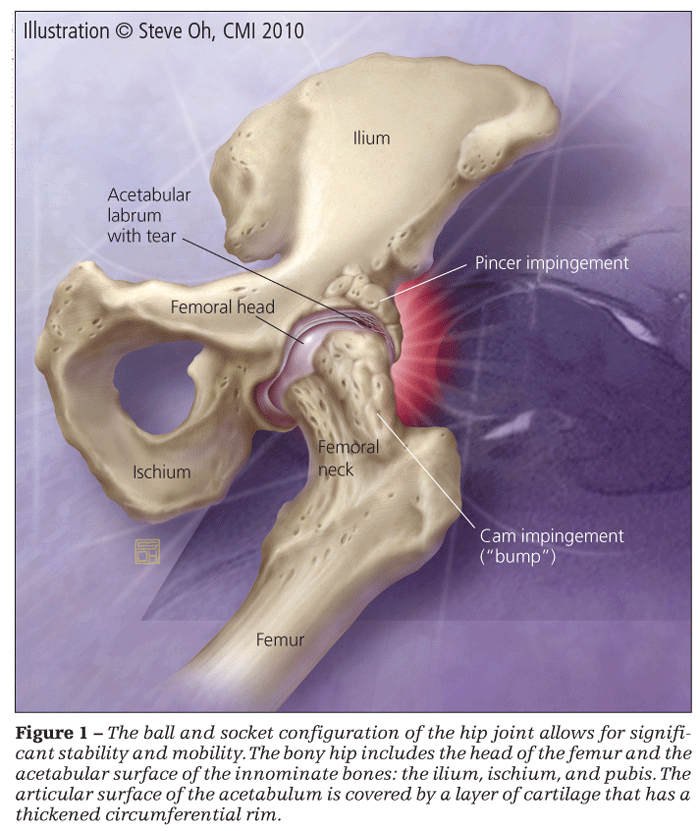
(Figure 1). The spherical area of articulation between the head of the femur and the acetabulum allows for significant pressure distribution in a weight-bearing joint that still can move extensively in 3 separate planes: frontal, sagittal, and transverse. Force across the joint ranges from 1.6 to 3.3 times body weight when a person walks and increases by up to 5 times body weight when a person runs.
The bony hip is composed of the head of the femur and the acetabular surface of the innominate bones. The acetabulum includes contributions from all 3 pelvic bones: the ilium, ischium, and pubis. The innominate bones articulate anteriorly at the symphysis pubis; the posterior portion of the pelvic girdle is completed by the sacrum (superiorly) and the coccyx (inferiorly).
The articular surface of the acetabulum is covered by a layer of cartilage that has a thickened circumferential rim, or labrum, that serves to deepen the acetabulum and bolster support of the femoral head. Additional stability is provided by 3 ligaments (iliofemoral, ischiofemoral, and pubofemoral) that surround the joint capsule and the small, less functional ligamentum teres, which is attached to the head directly.2 The femoral head is roughly two-thirds of a sphere that is covered in hyaline cartilage and connected to the femoral shaft by the neck. Typically, the junction of the femoral neck with the femoral shaft has an angle of 125° to 135°.3
Muscles in the joint area include those within the gluteal and lower lumbar regions and those that extend distally into the lower extremity. These muscles can be grouped by function around the hip joint: the iliopsoas and the quadriceps muscles control hip flexion; the gluteal muscles and the 3 muscles that make up the hamstrings perform extension; separate groups of muscles aid in the other hip motions (abduction, adduction, and internal and external rotation); and the gluteals, piriformis, and other smaller complementary muscles also aid in stability and movement of the proximal femur.2
In patients who have hip complaints, the source of pain often involves surrounding structures (the lower back and pelvis) rather than the hip joint. Therefore, it is important to maintain an awareness of these neighboring structures as well as of the articular hip.
History
Because the differential diagnosis of hip pain varies tremendously between the pediatric and adult patient populations, considering not only the patient's chronologic age but also his or her degree of physical maturation is critical. For example, the age range for apophyseal injuries spans prepubescence to age 30 years.
Often, knowledge of the mechanism of injury and the sport (and player's position) can help uncover the diagnosis. Inquiries should follow regarding the location of pain, radiation and duration of pain, exacerbating and relieving factors, and parasthesias. It is beneficial to ask patients to point to the area of maximum pain with one finger, because they often are tempted to describe larger, less specific distributions.
The patient's training regimen, past medical and surgical history, use of medications, and menstrual and dietary history should be explored. Patients also should be questioned about any previous injuries in the lower extremities (both ipsilateral and contralateral) because adaptations to deficits of the distal kinetic chain can contribute to hip pathology. In addition, because radicular pathology can masquerade as hip pain, low back injuries should be explored.
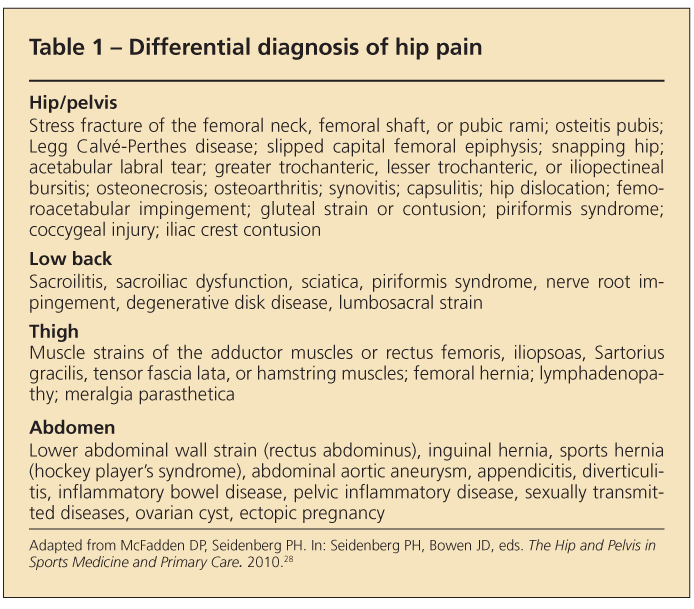
The hip may be considered responsible for a wide variety of disorders because of its frequent use, proximity to other anatomical features, and numerous pain referral patterns (Table 1). Therefore, the review of symptoms is broad. Groin and pelvic pathology that may be described as hip pain should be considered.
Inquiries about constitutional symptoms, including fever, chills, and weight loss, are important because metastatic bony lesions are common in the hip and pelvic regions.4 In addition, the examiner should inquire about signs of GI and genitourinary disorders, including sexually transmitted diseases (STDs).
Physical examination
The initial assessment includes vital sign measurements, particularly in the setting of high-energy trauma or suspected infectious causes. Often, paying careful attention to the patient's gait and standing posture uncovers diagnostic clues. A visual inspection can help identify muscular atrophy, pelvic obliquity (eg, leg length discrepancy, weak supporting musculature, or contractures), and significant scoliotic or lordotic curves.5
A thorough evaluation of the lumbosacral area is important to help distinguish hip pain from potential disk or nerve root disease. Depending on the history and clinical setting, it may be appropriate to perform a full abdominal and genitourinary examination to evaluate for hernia, nerve entrapment, STDs, and testicular/scrotal disorders. Palpation includes the musculature, bursal areas, apophyses, sacroiliac joints, and symphysis pubis.

Range of motion deficits can result from intra-articular pathology or musculotendinous strains. Table 2 shows the normal values for active range of motion. Passive range of motion should exceed active range of motion.
Muscular strength testing should be performed on all the cardinal movements of the hip joint. These movements include flexion and extension, abduction and adduction, and internal and external rotation. In addition, because multiple nerves traverse the hip and pelvis to travel from the back to the groin and lower extremity, a thorough neurological examination of the lower extremities is an essential part of the evaluation.
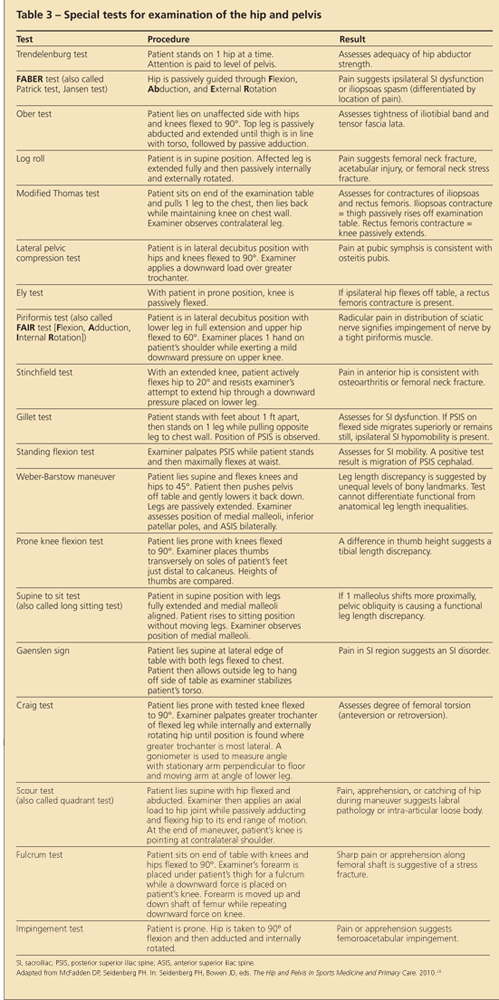
Then, special tests are used to narrow the differential diagnosis. In spite of the variability in the sensitivity, specificity, and inter-examiner reliability, these special tests can be helpful in augmenting the previously obtained historical and examination information. Table 3 summarizes some commonly used special tests for evaluation of the hip and pelvis.
Imaging
Evaluation of hip pain with imaging studies should include an anteroposterior (AP) x-ray view of the pelvis as well as AP and frog-leg lateral views of the affected hip.6 If pain is persistent and plain x-ray film results are normal, MRI can be valuable to further assess injury, especially in cases in which femoral neck stress fracture is suspected.6
MRI also can be helpful in assessment of musculotendinous injuries that are severe or show a poor response to conservative therapy. If intra-articular injury is suspected, magnetic resonance arthrography (MRA) may be helpful in the diagnosis; studies have shown a close correlation with surgical or pathological results.6 In situations in which MRI is not feasible, both bone scans and CT scans can be helpful in cases of suspected bony injury, but the lack of specificity in these modalities may limit their diagnostic value.
Musculoskeletal ultrasonography is becoming a more commonly used imaging modality in the hands of appropriately trained clinicians. This tool provides excellent static and dynamic views of the local anatomy. Bony pincer and Cam lesions often can be visualized. Areas of tendinopathy can be elucidated. Dynamically, tendinous culprits for snapping hip are easily demonstrated. This modality also is enabling physicians to perform ultrasonography-guided diagnostic and therapeutic injections in the outpatient setting.7,8
MANAGING SPECIFIC HIP
DISORDERS IN ATHLETESStress fractures
Femoral neck stress fractures must be considered in cases of unexplained hip pain. The risk of these injuries increases with abrupt increases in training regimen intensity, changes in running surface, use of inadequately cushioned footwear, presence of female athlete triad (the combination of disordered eating, amenorrhea, and osteoporosis), or other disorders that affect bone metabolism. Usually, the history includes a deep, aching pain on the affected side. Initially, patients say that the pain was noticeable only with extended weight-bearing activity but progressed to occur after less time and exertion.
If femoral neck stress fractures are not treated, a complete fracture of the femoral neck can occur. Because the femoral head has a limited blood supply that can be compromised by femoral neck fracture, osteonecrosis may result. Even fractures that do not progress to completion still can be at risk for this complication.
Often, physical examination reveals anterior hip pain with internal and external rotation and abnormal log roll and Stinchfield test results. Because these fractures may have devastating sequelae, an extremely low threshold is used for pursuing imaging and subsequent treatment. Weight bearing should be stopped until this diagnosis is ruled out.
Imaging consists of plain x-ray films (AP and frog-leg views), but often initial results are normal. Therefore, additional investigation is mandated. Historically, bone scans have been considered the gold standard. Because they lack specificity, however, MRI has proved more beneficial in most cases.9
Appropriate treatment varies with the location and degree of the fracture. For fractures that occur on the inferior aspect (compression side) of the femoral neck and involve less than 50% of the neck, conservative therapy with progressive weight bearing and activity may be considered. For fractures that involve more than 50% of the neck on the compression side and any fracture on the tension (distraction) side, immediate orthopedic evaluation for surgical repair is required.10
Slipped capital
femoral epiphysis
A common source of hip pain in growing adolescents, slipped capital femoral epiphysis (SCFE) results from posterior displacement of the proximal femoral physis. Although both the disorder and the risk factors associated with it have become more widely recognized, the diagnosis still is frequently overlooked or delayed.11
The risk factors for SCFE include obesity, male sex, rapid linear growth, and adolescent age. Although most cases occur after age 9 years in females and age 11 years in males, some cases have been recorded in patients as young as 5 years.12 Often, early cases of SCFE are associated with an underlying endocrine disorder.13
The diagnosis should be suspected in any young athlete who walks with a limp. Patients may describe pain that is located anywhere from the groin to the knee. However, pain is not always associated with this disorder; it may be noted simply as an ache within the broad region of the hip and thigh. If symptoms are present, usually they worsen with physical activity. Typically, the process is gradual and insidious, and any association with acute injury or trauma is rare.3
A determination of the acuity of the injury is important in the physical examination. In chronic slips, the affected leg often shows a tendency toward external rotation with limited and, possibly, painful internal rotation that may be more notable as the hip is brought into flexion. In acute slips, the leg is classically in a position of extension, adduction, and external rotation. Usually, patients note pain with flexion, abduction, and internal rotation.14
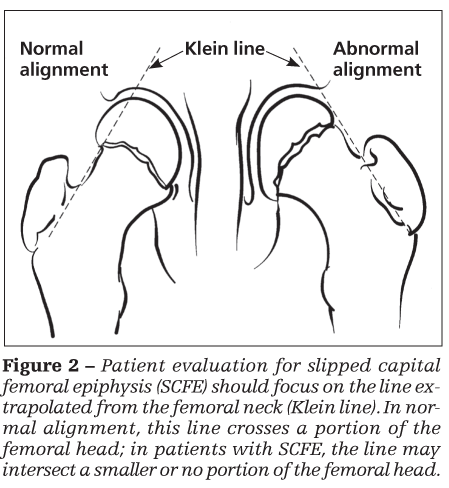
Radiographs are crucial in making the diagnosis. AP, lateral, and frog-leg views of the hip should be obtained.15 Comparison views are critical for full evaluation, especially given the possibility of bilateral disease. On an AP view, evaluation should focus on the line extrapolated from the femoral neck (Kline line) (Figure 2). In normal alignment, this line crosses a portion of the femoral head; in patients with SCFE, the line may intersect a smaller or no portion of the femoral head.
Frog-leg views can further illustrate the slip. Early slips may show only widening and blurring at the epiphysis. If the examiner has a high comfort level and experience, ultrasonography can be a useful diagnostic tool.16 If plain x-ray film results are equivocal, MRI or bone scanning can be helpful in the evaluation.
If SCFE is suspected, the patient should be placed immediately in a comfortable, non–weight-bearing position until the diagnosis is confirmed or ruled out. If imaging studies suggest slip, or if clinical suspicion is high regardless of the study results, immediate evaluation by an orthopedic surgeon is warranted.
Complications of delay in diagnosis or treatment (osteonecrosis and chondrolysis) can be devastating. Treatment is universally surgical, ranging from the placement of a single screw in mild slips to realignment and osteotomy in severe cases.17
It is extremely important to monitor the opposite hip in a patient who presents with SCFE. At the time of diagnosis, 20% of patients have evidence of the condition bilaterally. SCFE will develop in the opposite leg by 12 to 18 months in an additional 20% to 30% of patients.18
Osteitis pubis
Initially, this diagnosis was better known in postoperative patients who had undergone bladder or prostate surgeries; however, now it is also recognized in athletes. Typically, patients describe a gradual progression of discomfort and pain in the midline directly over the pubic symphysis. They may note radiation of the pain into the groin or abdomen or along the medial aspect of the thigh. In chronic and progressive cases, abdominal muscle spasm may occur and, eventually, result in significant gait disturbance.
The origin of this disorder is not well understood. Theories include supporting muscular weakness with secondary degeneration of the symphysis, fatigue fracture of the pubis, osteonecrosis, and osteochondritis dissecans. Although it was assumed in the older literature that this disorder results from pelvic infection, newer studies have shown that osteitis pubis caused by infection is extremely rare.19
Physical examination reveals tenderness directly over the pubic symphysis. Passive abduction, resisted adduction,3 and the lateral compression test also elicit pain.
Diagnosis can be aided by obtaining plain x-ray films, which may show a widening of the pubic symphysis and either bony resorption or sclerosis at the bony edges.12 Bone scanning confirms the diagnosis by showing increased uptake at the pubic symphysis.
Usually, treatment is conservative, consisting of NSAIDs, active rest, wearing compression shorts, and avoidance of eliciting activities. In small studies, local corticosteroid injection has been shown to offer a mild benefit. In severe cases of osteitis pubis, various surgical strategies can be pursued.20
Snapping hip syndrome
In this disorder, athletes experience a “snapping” sensation when the hip is flexed and extended. Descriptions of snapping must be clarified as to whether the snap is noted over the lateral (external) or anterior (internal) hip.
In cases of external snapping, the usual cause is an iliotibial band (ITB) that is snapping over the greater trochanter of the femur. To assess the ITB as the cause of external snapping hip, place the patient on his unaffected side. As the upper hip is moved from extension to flexion, a palpable “pop” may be noted as the ITB slides from a posterior to an anterior position. Pressure should be placed over the greater trochanter to hold the ITB in the posterior position.3 Musculoskeletal ultrasonography can be used to confirm the cause of the snapping. If the patient is otherwise asymptomatic, no treatment is necessary.
The friction from the overriding ITB may cause inflammation of the greater trochanteric bursa, with or without the presence of snapping. In cases of direct trauma or increased tension of the overriding tissue, the bursae easily can become inflamed; this inflammation is noted as tenderness that is reproduced with direct pressure or increasing strain.
In cases of greater trochanteric bursitis, tenderness is reproduced with external rotation and adduction of the hip. Exacerbating factors may include leg length discrepancy, excessive foot pronation, weak hip abductors, and persistent stance alteration (constant running on the same side of a cambered road or in the same direction on a small track).3
Initial therapy for patients with greater trochanteric bursitis or symptomatic snapping hip should consist of active rest, stretching, ice, and NSAIDs. Patients with chronic or severe bursitis may benefit from corticosteroid injection. If a long course of conservative therapy is ineffective, patients may be evaluated for possible Z-plasty of the ITB and excision of the greater trochanteric bursa.3
Of note, some patients once thought to have greater trochanteric bursitis on examination later were found under ultrasonographic evaluation to lack inflammation of the bursa. Instead, they were found to have gluteus medius tendinosis.
Internal snapping hip can be caused by a variety of lesions. The snap may be accompanied by pain at the hip or the knee as the hip is moved into flexion or extension. Although many cases may involve a relatively benign overlapping of muscle body or tendon on a bony prominence, it is also important to note that a clicking sensation may be the manifestation of an intra-articular derangement (eg, osteochondromatosis, loose bodies, labral damage, or subluxation).21 Clinical examination revealing a click and a history suggesting symptoms of locking are more indicative of labral or acetabular damage.
Ultrasonography-guided intra-articular diagnostic injection can be helpful in confirming hip joint pathology.8 The use of MRA also may be helpful in the diagnosis.6 In cases in which imaging results are equivocal or further intervention is anticipated, arthroscopy may be required for appropriate diagnosis and subsequent treatment; radiological studies have been noted to have limitations in this area.22
A history of locking is more suggestive of a labral tear or loose body; internal snapping without functional deficit is suggestive of the iliopsoas tendon catching on various structures within the anterior region of the hip (eg, the femoral head [most probable], iliopectineal ridge and bursa, and bony growths on the medial aspect of the lesser trochanter). Snapping of the iliopsoas tendon can be elicited by having the patient lie supine and flex the hip and knee, abduct and externally rotate the hip, and then extend the leg. This also may be assessed dynamically using musculoskeletal ultrasonography.
If the history, examination, and any subsequent imaging results suggest that the injury is not articular, conservative therapy is appropriate. This may consist of stretching, activity modification, and avoidance of activities that exacerbate the snapping. In refractory cases, surgery might be considered to perform a release of the iliopsoas tendon.12
Hip osteoarthritis
Although arthritis is thought to occur less frequently in athletes than in the general population, there is evidence to suggest that athletes are more at risk for osteoarthritis (OA) of the hip than their more sedentary counterparts. In a study that controlled for obesity, smoking, and other potential confounders, longtime sports participation was shown to increase the risk of hip arthritis almost 5-fold.23 However, this result runs contrary to the consensus; other epidemiological study results have suggested that moderate-load exercise is protective, as well as therapeutic, in many cases of mild to moderate OA.24
Hip OA is the progressive and chronic breakdown of the cartilaginous surface of the femoral head and the acetabulum. As the wear continues, the patient notices worsening pain with weight bearing, gait disturbance, and decreasing range of motion. Often, these findings are elicited on examination. Patients often note worsened pain with internal rotation of the hip; also, the Trendelenburg test result may be abnormal.25 The radiological findings include joint-space narrowing, subchondral sclerosis, subchondral cysts, and osteophytosis.26
Treatment of athletes with OA includes oral analgesics, stretching, and strengthening of muscular deficits. Chondroprotective agents may be considered. Viscosupplementation of hip OA is showing promising results,7 but its use currently is off-label.
Femoroacetabular
impingement (FAI)
This condition results from impingement of the anterior femoral head-neck junction against the anterosuperior labrum. Recognition of and familiarity with this condition is imperative because it is thought to lead to premature hip OA. Clinically, patients present with groin pain or pain over the greater trochanter; they may even complain of a grinding sensation. Pain is worse with hip flexion and internal rotation; prolonged sitting also aggravates the condition. The impingement test result often is positive. FAI can be visualized on plain radiographs, musculoskeletal ultrasonograms, CT scans, MRI, or MRA. Treatment for symptomatic patients is surgery.7
References:
References
1. Scopp JM, Moorman CT 3rd. The assessment of athletic hip injury. Clin Sports Med. 2001;20:647-659.
2. Jenkins DB, Hollinshead WH. Hollinshead's Functional Anatomy of the Limbs and the Back. Philadelphia: WB Saunders Co; 1998:246.
3. Nuccion S, Hunter D, Finerman G. Hip and pelvis. In: DeLee J, Drez D, Miller MD, eds. Orthopaedic Sports Medicine: Principles and Practice. Vol 2. Philadelphia: WB Saunders Co; 2003:1444, 1447, 1448, 1466.
4. Hage WD, Aboulafia AJ, Aboulafia DM. Incidence, location, and diagnostic evaluation of metastatic disease. Orthop Clin North Am. 2000;31:515-528, vii.
5. Magee DJ. Hip. In: Magee DJ, ed. Orthopedic Physical Assessment. 3rd ed. Philadelphia: WB Saunders Co; 1997:460.
6. Bencardino JT, Palmer WE. Imaging of hip disorders in athletes. Radiol Clin North Am. 2002;40:267-287, vi-vii.
7. Mulvaney SW. A review of viscosupplementation for osteoarthritis of the hip and a description of an ultrasound-guided hip injection technique. Curr Sports Med Rep. 2009;8:291-294.
8. Sofka CM, Saboeiro G, Adler RS. Ultrasound-guided adult hipinjections. J Vasc Interv Radiol. 2005;16:1121-1123.
9. Shin AY, Morin WD, Gorman JD, et al. The superiority of magnetic resonance imaging in differentiating the cause of hip pain in endurance athletes. Am J Sports Med. 1996;24:168-176.
10. Brukner P, Bradshaw C, Bennell K. Managing common stress fractures: let risk level guide treatment. Phys Sportsmed. 1998;26:39-47.
11. Kocher MS, Bishop JA, Weed B, et al. Delay in diagnosis of slipped capital femoral epiphysis. Pediatrics. 2004;113:e322-e325.
12. Bandyopadhyay S, Teach SJ. Slipped capital femoral epiphysis in a 5½-year-old obese male. Pediatr Emerg Care. 1999;15:104-105.
13. Wells D, King JD, Roe TF, Kaufman FR. Review of slipped capital femoral epiphysis associated with endocrine disease. J Pediatr Orthop. 1993;13:610-614.
14. Perron AD, Miller MD, Brady WJ. Orthopedic pitfalls in the ED: slipped capital femoral epiphysis. Am J Emerg Med. 2002;20:484-487.
15. Bloomberg TJ, Nuttall J, Stoker DJ. Radiology in early slipped capital femoral epiphysis. Clin Radiol. 1978;29:657-667.
16. Reynolds RA. Diagnosis and treatment of slipped capital femoral epiphysis. Curr Opin Pediatr. 1999;11:80-83.
17. Busch MT, Morrissy RT. Slipped capital femoral epiphysis. Orthop Clin North Am. 1987;18:637-647.
18. Nasin CS, Nasin MC. Hip and pelvis injuries in childhood. In: Seidenberg PH, Bowen JD, eds. The Hip and Pelvis in Sports Medicine and Primary Care. New York: Springer Science+Business Media; 2010:149-170.
19. Fricker PA, Taunton JE, Ammann W. Osteitis pubis in athletes: infection, inflammation or injury? Sports Med. 1991;12:266-279.
20. Holt MA, Keene JS, Graf BK, Helwig DC. Treatment of osteitis pubis in athletes: results of corticosteroid injections. Am J Sports Med. 1995;23:601-606.
21. Canale ST, Campbell WC. Campbell's Operative Orthopaedics. 10th ed. St Louis: Mosby, Inc; 2003:890.
22. McCarthy JC, Busconi B. The role of hip arthroscopy in the diagnosis and treatment of hip disease. Orthopedics. 1995;18:753-756.
23. Vingard E, Alfredsson L, Goldie I, Hogstedt C. Sports and osteoarthrosis of the hip: an epidemiologic study. Am J Sports Med. 1993;21:195-200.
24. Buckwalter JA, Lane NE. Athletics and osteoarthritis. Am J Sports Med. 1997;25:873-881.
25. Altman R, Alarcon G, Appelrouth D, et al. The American College of Rheumatology criteria for the classification and reporting of osteoarthritis of the hip. Arthritis Rheum. 1991;34:505-514.
26. Gupta KB, Duryea J, Weissman BN. Radiographic evaluation of osteoarthritis. Radiol Clin North Am. 2004;42:11-41.
27. Seidenberg PH. Adult hip and pelvis disorders. In: Seidenberg PH, Bowen JD, eds. The Hip and Pelvis in Sports Medicine and Primary Care. New York: Springer Science+Business Media; 2010:115-147.
28. McFadden DP, Seidenberg PH. Physical examination of the hip and pelvis. In: Seidenberg PH, Bowen JD, eds. The Hip and Pelvis in Sports Medicine and Primary Care. New York: Springer Science+Business Media; 2010:9-36.