Tissue engineering with platelet-rich plasma and stem cells: New frontier in rheumatology?
The ability to heal soft tissue injuries and regenerate cartilage is the Holy Grail of musculoskeletal medicine. With advances in cell biology and technology, practicing physicians now may accomplish more in this area than ever before: platelet-rich plasma (PRP) can be used for multiple soft tissue injuries, and autologous stem cells used in combination with PRP may be effective for tissue repair (eg, rotator cuff tears) as well as cartilage regenerative processes.
The ability to heal soft tissue injuries and regenerate cartilage is the Holy Grail of musculoskeletal medicine. With advances in cell biology and technology, practicing physicians now may accomplish more in this area than ever before: platelet-rich plasma (PRP) can be used for multiple soft tissue injuries, and autologous stem cells used in combination with PRP may be effective for tissue repair (eg, rotator cuff tears) as well as cartilage regenerative processes.
Much curiosity and excitement have surrounded the topic of tissue engineering recently. In this article, I address some key issues as they relate to rheumatologic disorders, based on anecdotal and uncontrolled experience. This experience clearly is not a substitute for randomized clinical trials, but they may be instituted in the not too distant future.
PLATELET-RICH PLASMA
Treatment with PRP allowed Pittsburgh Steelers wide receiver Hines Ward to play in Super Bowl XLIII this year even though he had a severe medial collateral ligament injury. Among the first to see and use PRP were practitioners of musculoskeletal medicine, particularly those skilled in prolotherapy. PRP has been used in a number of specialties but appears to have its greatest application in managing musculoskeletal injuries.1,2
PRP as a matrix graft
Large multicenter controlled studies of PRP are lacking, but there is enough anecdotal evidence to encourage its use as a "matrix tissue graft" to regenerate injured tissue, relieve pain, and reduce related dysfunction.3 The review of literature on this subject is frustrating for analytical physicians, such as rheumatologists; what makes it so is an astounding number of "labels" given to tissue grafts that makes comparison of studies difficult, if not impossible. In addition, practitioner skill in incorporating proper injection technique with ultrasonographic guidance is mandatory, but many physicians using PRP are not aware of this necessary ingredient or choose to ignore it.
Platelets contain 2 types of granules, a and dense. The a granules contain a variety of hemostatic proteins, cytokines, growth factors, chemokines, and adhesion molecules. Among these substances are transforming growth factor b (TGF-b) and basic fibroblast, platelet-derived, epidermal, vascular endothelial, and connective tissue growth factors.4 Dense granules have factors that lead to platelet aggregation. Platelet activation leads to granule content discharge. Proper preparation of the PRP allows platelets to aggregate and adhere to the site needed for tissue healing.
PRP is prepared using a special centrifugation technique that concentrates the platelets in a small volume of plasma. The platelets should not be activated until grafting occurs. A platelet-rich autologous tissue graft is formed by inducing platelet activation at the time of injection into the injured area. This is done by combining the PRP with calcium chloride and thrombin. The latter 2 ingredients combine with fibrin located within the platelet preparation to form an activated platelet matrix.
Stages of healing
Examination of the healing process is needed to understand what PRP does. The stages of healing-inflammation, proliferation, and remodeling-involve complex interaction of multiple types of cells.
During the inflammatory phase, which lasts about 2 or 3 days, the functions of platelets include adhesion, aggregation, clot retraction, coagulation, cytokine signaling, chemokine release, and growth factor release.5 Phagocytes are attracted. The first event after injury is hemostasis, followed by tissue regeneration. The average peripheral blood platelet count is about 200,000/μL. There is scientific evidence of bone and soft tissue healing enhancement at 1,000,000 viable platelets/μL.6
After the initial inflammatory phase, fibroblasts enter the site and begin the proliferative phase.7 This phase, which lasts 2 to 4 weeks, is mandatory for tissue repair. Fibronectin stimulates endothelial cells to start neovascularization. By the seventh day, fibroblasts are the most abundant cell; they are responsible for deposition of collagen and ground substance. Fibroblasts differentiate into myofibroblasts, and actin contracts to make the wound smaller.5
During the remodeling phase, which may last for up to 1 year, collagen strengthens and matures. Type III collagen is replaced with type I collagen, and neovascularity disappears.7
For autologous tissue grafts to function properly, 3 elements must be present: (1) an adequate number of platelets to concentrate to stimulate proliferation, (2) an adequate inflammatory response with production of signal proteins and adhesion molecules, and (3) a stable matrix.8 The site of pathology usually needs to undergo fenestration with a needle, which involves making multiple punctures with ultrasonographic guidance to induce an acute inflammatory reaction. Then PRP is infused, also with ultrasonographic guidance (Figure 1).
Figure 1–Ultrasonographic guidance is used for infusing platelet-rich plasma after tenotomy in a patient with peroneal tendinopathy.
Injuries that respond
Injuries that respond to PRP include enthesopathies, such as epicondylitis, plantar fasciitis, patellar tendinosis, Achilles tendinosis, peroneal and posterior tibial tendinopathy, and rotator cuff tendinopathy. PRP also has been used in other conditions, such as piriformis syndrome, obturator and gluteus medius insertional enthesopathy, and various forms of bursitis.
Contraindications to the use of PRP include thrombocytopenia or abnormal platelet function, hypofibrinogenemia, hemodynamic instability, septicemia, sensitivity to bovine thrombin, and anemia. In addition, patients should be counseled to discontinue NSAIDs and immunosuppressive drugs that could interfere with the inflammatory process. One treatment often is effective, but repeating the process 2 or 3 times at 4 to 6 weeks may be needed to optimize results.
After the procedure, patients may describe significant discomfort for 4 days but usually feel better by 10 to 14 days. Narcotic analgesics rather than NSAIDs should be prescribed for pain. Ice should be avoided.
The technology remains somewhat "shrouded in mystery." However, evidence from studies indicates that growth factors appear to play a significant role in the effectiveness of PRP.
STEM CELLS
A second phase of regenerative technique involves using PRP in tandem with stem cells. The use of biologic agents has led to the expectation of inducing remission in many patients with rheumatoid arthritis (RA), but an effective treatment for osteoarthritis (OA) remains elusive-ironic considering that RA is only about one-tenth as common as OA.9,10
Treatment for patients with OA has been aimed at symptom reduction, but a therapy that preserves and regenerates cartilage has not been demonstrated convincingly. To date, supplements (eg, glucosamine/chondroitin) and drugs (eg, minocycline) have been used with mixed results. Inhibition of matrix metalloproteinases and of various cytokines also is being studied. For patients in whom cartilage wear has been excessive, osteotomies and other interventions "buy time" until the need for joint replacement is evident.11
In sports medicine, a variety of methods have been used to repair cartilage lesions, including osteochondral grafting; microfracture procedures; and autologous chondrocyte implantation, sometimes with a scaffold matrix to deliver the cells.12,13 However, these techniques are limited to fixing focal lesions.14
Restoring articular cartilage
The major goal of stem cell therapy is restoration of diffuse diseased articular cartilage. The use of techniques aimed at harvesting the pluripotential power of embryonic stem cells (ESCs) or adult mesenchymal stem cells (MSCs) to differentiate into cartilage cells has led to a variety of strategies.15,16 ESCs probably have greater ability to multiply quickly but, theoretically, also have potential for unchecked growth (neoplasia). In addition, some groups have raised ethical concerns about the use of ESCs.
MSCs may be delivered via direct intra-articular injection or by the use of cell-seeded scaffolds.17 They can be obtained via donors. The advantage is an excellent concentration of stem cells (about 10 million to 50 million cells per specimen); the disadvantages are theoretical (rejection reactions and possible transmission of viral pathogens).
The final avenue is the use of autologous MSCs, which are obtained from bone marrow harvested at the iliac crest. The marrow specimen is then concentrated to isolate the MSCs. The number of stem cells obtained may not quite reach the concentration obtained from the donor approach, but there is no danger of rejection reaction.
The major problem with autologous MSCs is that patients with OA tend to be older. Some evidence indicates that their MSCs may not proliferate and differentiate as well as younger MSCs.17 In addition, OA may occur as a result of metabolic defects that autologous stem cells may share. However, studies have indicated that enough MSCs with adequate cartilage growth potential can be isolated from patients with OA, regardless of their age.18 Therefore, the results suggest that the therapeutic use of MSCs for regeneration of cartilage in patients with OA is feasible.
Direct intra-articular injection of MSCs is, technically, the simplest approach to their use in OA; such injection has been evaluated in studies that demonstrate healing potential.19 Another option is to use a scaffold in which stem cells are suspended. Scaffolds need to be made of biodegradable and biocompatible materials. Various scaffolds with natural or synthetic materials have been used.20 Whether the type of cartilage created with stem cell therapy is hyaline or fibrocartilage is a concern.20
STEM CELLS AND PRP COMBINED
A synergy between stem cells and PRP has been described.21 At our center, we have begun to study the combination intensively.
Stem cells have tyrosine kinase receptors on the cell surface. Growth factors released from activated platelets bind to cell membranes to activate genes controlling mitosis. Signal transduction occurs once growth factors bind to receptors. Secondary messenger proteins are activated and enter the nucle-us of the stem cell. Expression of genes triggers cell division.
In theory, inducing stem cells to proliferate and regenerate new cartilage should be possible, given the proper environment. Multiple studies have demonstrated that this is a potentially feasible option for managing OA.8 One study even demonstrated that a minimally invasive stem cell procedure could be superior to microfracture.22
Because effective disease-modifying and structure-improving treatments for OA are scarce, we are investigating a combined autologous stem cell–PRP approach to knee OA. We harvest bone marrow from the iliac crest and concentrate, and we isolate a stem cell concentrate consisting of 1 million to 5 million cells. We also draw peripheral blood to obtain the PRP.
The area for consideration is prepped sterilely. Using ultrasonographic needle guidance with local anesthetic, we "irritate" the area of concern with either a needle or trochar, depending on the specific site. Once enough local injury has been established, alternating infusions of stem cell concentrate and PRP are given, along with a tissue-activating agent, which helps a gel scaffold to be formed (Figure 2).
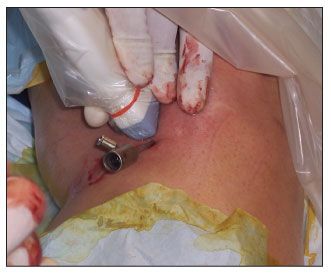
Figure 2– Stem cells may be used with platelet-rich plasma (PRP) for the management of osteoarthritis (OA). A trochar is in place for fenestration and introduction of stem cells and PRP for OA of the knee.
Currently, we are measuring patient response using both subjective measures (eg, Western Ontario and McMaster Universities Index, patient and physician visual analog scale scores) and objective measures (eg, 50-foot walk, ultrasonographic measurement of cartilage thickness, skier's-view knee films). The preliminary results are very encouraging.
The combination of PRP with stem cells could increase the biological property of stem cells but also could decrease it. However, the evidence to date indicates that growth factors from PRP are stimulatory to stem cell replication and division. In addition, the combination of stem cells with TGF-b may lead to scar tissue. However, scar tissue is not necessarily a bad thing, particularly in that it indicates healing rather than ongoing damage.
References:
References1. Gamradt SC, Rodeo SA, Warren RF. Platelet-rich plasma in rotator cuff repair. Tech Orthop. 2007;22:26-33.
2. Mishra A, Pavelko T. Treatment of chronic elbow tendinosis with buffered platelet-rich plasma. Am J Sports Med. 2006;34:1774-1778.
3. Marx RE, Carlson ER, Eichstaedt RM, et al. Platelet-rich plasma: growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;85:638-646.
4. Kevy SV, Jacobson MS. Comparison of methods for point of care preparation of autologous platelet gel. J Extra Corpor Technol. 2004;36:28-35.
5. Crane D, Everts PA. Platelet rich plasma (PRP) matrix grafts. Pract Pain Manage. 2008;8:12-26.
6. Weibrich G, Hansen T, Kleis W, et al. Effect of platelet concentration in platelet-rich plasma on peri-implant bone regeneration. Bone. 2004;34:665-671.
7. Kumar V, Abbas A, Fausto N. Acute and chronic inflammation. In: Kumar V, Abbas A, Fausto N, eds. Robbins and Cotran Pathologic Basis of Disease. 7th ed. Philadelphia: WB Saunders; 2005:47-86.
8. Nöth U, Steinert AF, Tuan RS. Technology insight: adult mesenchymal stem cells for osteoarthritis therapy. Nat Clin Pract Rheumatol. 2008;4:371-380.
9. Elders MJ. The increasing impact of arthritis on public health. J Rheumatol Suppl. 2000;60:6-8.
10. Brooks PM. Impact of osteoarthritis on individuals and society: how much disability? Social consequences and health economic implications. Curr Opin Rheumatol. 2002;14:573-577.
11. Günther KP. Surgical approaches for osteoarthritis. Best Pract Res Clin Rheumatol. 2001;15:627-643.
12. Bartlett W, Skinner JA, Gooding CR, et al. Autologous chondrocyte implantation versus matrix-induced autologous chondrocyte implantation for osteochondral defects of the knee: a prospective, randomised study.J Bone Joint Surg. 2005;87B:640-645.
13. Bentley G, Biant LC, Carrington RW, et al. A prospective, randomised comparison of autologous chondrocyte implantation versus mosaicplasty for osteochondral defects in the knee. J Bone Joint Surg. 2003;85B:223-230.
14. Steinert AF, Ghivizzani SC, Rethwilm A, et al. Major biological obstacles for persistent cell-based regeneration of articular cartilage. Arthritis Res Ther. 2007;9:213.
15. Ferng AS, Ferguson CW, Szivek JA. Inducing cartilage regeneration with stem cells for treatment of osteoarthritis patients. FASEB J. 2008;22:819.1.
16. Jorgensen C, Noel D, Apparailly F, Sany J. Stem cells for repair of cartilage and bone: the next challenge in osteoarthritis and rheumatoid arthritis. Ann Rheum Dis. 2001;60:305-309.
17. Murphy JM, Dixon K, Beck S, et al. Reduced chondrogenic and adipogenic activity of mesenchymal stem cells from patients with advanced osteoarthritis. Arthritis Rheum. 2002;46:704-713.
18. Scharstuhl A, Schewe B, Benz K, et al. Chondrogenic potential of human adult mesenchymal stem cells is independent of age or osteoarthritis etiology. Stem Cells. 2007;25:3244-3251.
19. Murphy JM, Fink DJ, Hunziker EB, Barry FP. Stem cell therapy in a caprine model of osteoarthritis. Arthritis Rheum. 2003;48:3464-3474.
20. Nesic D, Whiteside R, Brittberg M, et al. Cartilage tissue engineering for degenerative joint disease. Adv Drug Deliv Rev. 2006;58:300-322.
21. Massberg S, Konrad I, Schürzinger K, et al. Platelets secrete stromal-derived factor 1a and recruit bone marrow-derived progenitor cells to arterial thrombin in vivo. J Exp Med. 2006;203:1221-1233.
22. Knutsen G, Engebretsen L, Ludvigsen TC, et al. Autologous chondrocyte implanatation compared with microfracture in the knee. A randomized trial. J Bone Joint Surg. 2004;86A:455-464.