10 Challenges in Treating Lupus
We have come a long way since the introduction of glucocorticoids for the treatment of systemic lupus erythematosus (SLE). But even with improved treatment and prognosis several challenges remain in the management of SLE. Here, we highlight the 10 most important challenges in treating patients with SLE.
10 most important challenges in treating patients with SLE. (©Blueringmedia,AdobeStock)
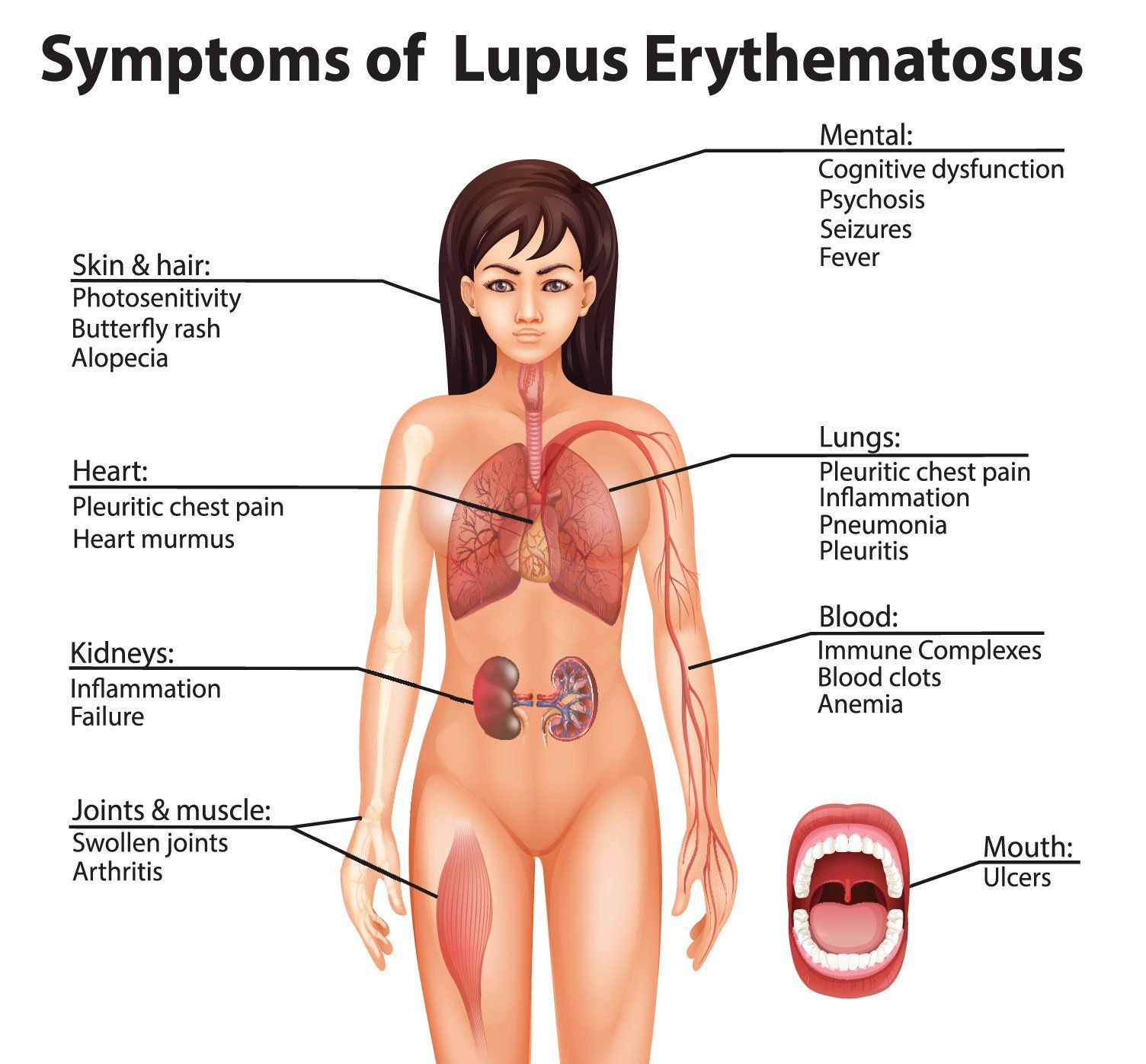
We have come a long way since the introduction of glucocorticoids for the treatment of systemic lupus erythematosus (SLE). A one-year survival rate of 50 percent has become a 10-year survival of 90 percent due to advances in treatment. Even with improved treatment and prognosis several challenges remain in the management of SLE.
In this article, we highlight the 10 most important challenges in treating patients with SLE as outlined by Laurent Arnaud, M.D., Ph.D., of Strasbourg, France, in a review published in Lupus Science & Medicine earlier this year.
1) Treat to target favoring disease remission (or low disease activity)
In 2016, a large international panel sought to define remission in systemic lupus erythematosus (SLE). The panel was able to agree on three principles:
- Remission should be a durable state.
- A validated index should be used.
- Distinction should be made between remission on and off therapy.
While at the same time the Asia Pacific Lupus Collaboration developed a Low Disease Activity State index, the challenge remains to validate whether these definitions are predictive of outcomes and ultimately used as targets in treat-to-target management of SLE.
2) Limiting the use of glucocorticoids
While glucocorticoids have played a major role in the improvement of systemic lupus erythematosus (SLE) prognosis, a large number of patients never discontinue glucocorticoids. Glucocorticoid dose predicts its overall exposure which can increase the risk of damage accrual even at low doses. Several challenges exist with regards to glucocorticoid treatment in SLE:
- Using a low dose glucocorticoid or a glucocorticoid free regimen should be discussed as a major target.
- Glucocorticoid management should be addressed as an important concern in future research with glucocorticoid tapering schemes, glucocorticoid-related adverse events, damage accrual and cumulative glucocorticoid doses being examined.
- Glucocorticoid doses should be managed using more objective tools such as the glucocorticoid cumulative dose, follow-up of disease activity and damage, and recording of glucocorticoid-related adverse events.
See "Deriving more comprehensive tools for the evaluation of disease activity" next page...
3) Deriving more comprehensive tools for the evaluation of disease activity
Do to multiple organs being involved in systemic lupus erythematosus (SLE), it is difficult to define disease activity as a whole. While several tools have been developed to assess the overall activity of the disease, in most cases the clinician has to form a judgment with regard to whether each manifestation is due to SLE or some other cause.
The authors believe that a more objective and reproducible measure of disease activity is needed and may include biomarkers and utilization of modern technology such as deep machine learning.
4) Developing more effective and better tolerated drugs
While drug therapy in systemic lupus erythematosus (SLE) has improved, several gaps remain in the care of SLE patients such as the progression of lupus nephritis to end-stage kidney disease.
For example, in lupus nephritis, a significant proportion of patients still progress towards end-stage kidney disease.
“Our group has recently published a systematic review (in the Annals of Rheumatic Diseases) of 74 targeted therapies for SLE, showing that we may expect great changes in the therapeutic tools available for SLE treatment,” the authors wrote. “We believe that current challenges are shifting from whether some new drugs will be available to the identification of the best strategy for the selection of the most adequate drug (or drug combination) at the patient level, to warrant a positive balance between efficacy and side effects. The need to investigate biomarkers that would allow adequate prediction of response to therapy remains high, but when solved will allow a more rational selection of the optimal
pharmacological agent within the broad pipeline of targeted therapies for SLE.”
These current challenges are shifting from whether new drugs will be available to identifying the best strategy for the selection of the most adequate drug, or drug combination, at the patient level.
Identifying strong biomarkers will allow a more rational selection of the optimal pharmacological agent.
5) Dissecting the heterogeneity of the disease at the molecular and genetic level
Both environmental and genetic factors play roles in the development and exacerbation of systemic lupus erythematosus (SLE). To date, a large number of nucleotide polymorphisms have been implicated in SLE however none of them have utility on their own in the diagnosis or treatment of patients.
An important challenge will be to develop an optimal genetic model for patients’ sub-stratification using multiomics to better personalize medicine for patients with SLE
6) Identifying relevant biomarkers for individualized treatment
Matching the right treatment to the individual patient remains a challenge in SLE. Traditional markers such as anti-double-stranded-DNA fall short and should give way to multiomics, which utilize high-throughput tools such as next-generation sequencing and computerization of data, to open the door for an integrated and personalized treatment approach.
Non-coding RNAs, owing to being tissue-specific regulators of gene expression, may emerge as important makers of flares in SLE. It remains a challenge to develop a holistic approach to SLE, a challenge that will require a specialized interface between all providers.
See "Managing fertility and pregnancy" next page....
7) Managing fertility and pregnancy
Pregnancy remains a significant challenge in women with systemic lupus erythematosus (SLE). We as clinicians have to improve the outcomes of pregnancy in patients with aPL and/or anti-SSA/B antibodies.
The overall prognosis of pregnancy in SLE is better when the disease has been in remission for at least six months, or one year for nephritis with a low organ damage score.
Strong predictors of complications during pregnancy with SLE include: Active SLE at the time of conception and/or positivity for lupus anticoagulant or triple positivity, use of antihypertensive treatments, and low platelet count.
Finally, clinicians should be aware that pregnancy complications can mimic SLE flares and anti-phospholipid antibodies can lead to both maternal and fetal adverse events.
8) Managing comorbidities
Late cardiovascular morbidity and mortality have increased along with overall systemic lupus erythematosus (SLE) patient survival. One challenge here is that measures validated for determining cardiovascular disease risk are based on North American populations and may not be adapted from the general population to patients with SLE.
Infections remain an serious comorbidity with SLE. Vaccines should be used provided immunosuppressive therapy does not contraindicate use.
Osteoporosis can be significant in SLE patients especially with glucocorticoid treatment. Anti-osteoporotic treatment should be considered.
9) Improving the network of care
More light should be shed on rare diseases like systemic lupus erythematosus (SLE). We need to improve early diagnosis while limiting diagnosis uncertainty. Training of new clinicians should included recognition of rare diseases and education should be provided to practicing caregivers, patients, and their families alike. Global awareness should be the goal.
10) Favoring a holistic approach
All aspects of the patient with SLE should be addressed. Patient reported outcome measures can facilitate holistic treatment and lead to better quality of life. Just as organ damage is a concern, so should fatigue, depression, pain, sleep disturbance and obesity be.
Better trials are needed in an effort to find non-pharmacological interventions aimed at treating the whole patient. Finally, individual factors such as race, smoking, and socioeconomic background should be taken into consideration when developing a plan for patients with SLE.
REFERENCE
Renaud Felten, Flora Sagez, Pierre-Edouard Gavand, et al. “10 most important contemporary challenges in the management of SLE.” Lupus Science & Medicine 2019;6:e000303. DOI:10.1136/ lupus-2018-000303