A case of arthritis, pulmonary nodules, and hilar adenopathy
After a trip to El Salvador, a woman experienced fever, malaise, and other symptoms. She had a history of a positive antinuclear antibodies test result, Raynaud phenomenon, and erythematous rash. The patient was hospitalized for pneumonia, and her symptoms persisted when she received antibiotics. Later her right ankle became red, swollen, and tender. Examination of the patient's extremities showed osteoarthritis changes.
During a 2-week trip to El Salvador, the patient drank bottled water and stayed in clean habitation but was in a rural environment. She was well until 9 days after she returned, when she experienced several symptoms-fever, malaise, a slight nonproductive cough, headache, and a stiff neck. After a few more days, the patient was hospitalized for pneumonia.
In this article, we describe an uncommon case that demonstrates the possibility of misdiagnosis resulting in a delay in appropriate treatment. The case also demonstrates the importance of being aware of CDC announcements and the information they provide.
Presentation
The patient, a 67-year-old white woman, presented with the symptoms on December 24, 2008, several days after her trip. She had a history of a positive antinuclear antibodies (ANA) test result, Raynaud phenomenon, and macular erythematous rash on her trunk and extremities.
On the basis of chest x-ray results, the patient was hospitalized for pneumonia 4 days later. She was treated with levofloxacin intravenously, followed by azithromycin administered orally. Because symptoms persisted throughout the antibiotic courses, the patient then was given a 10-day course of oral levofloxacin.
The patient then “felt well” until about 2 weeks later, when her right ankle became red, swollen, and tender. She was treated with indomethacin, which she reported “helped a bit with the pain,” but it did not reduce the swelling. The swelling of the right ankle worsened, and some swelling developed in both hands. The patient was admitted to a local hospital, given a corticosteroid (40 mg/d, followed by a 10-mg taper every 2 days), and then referred to our center's Section of Rheumatology.
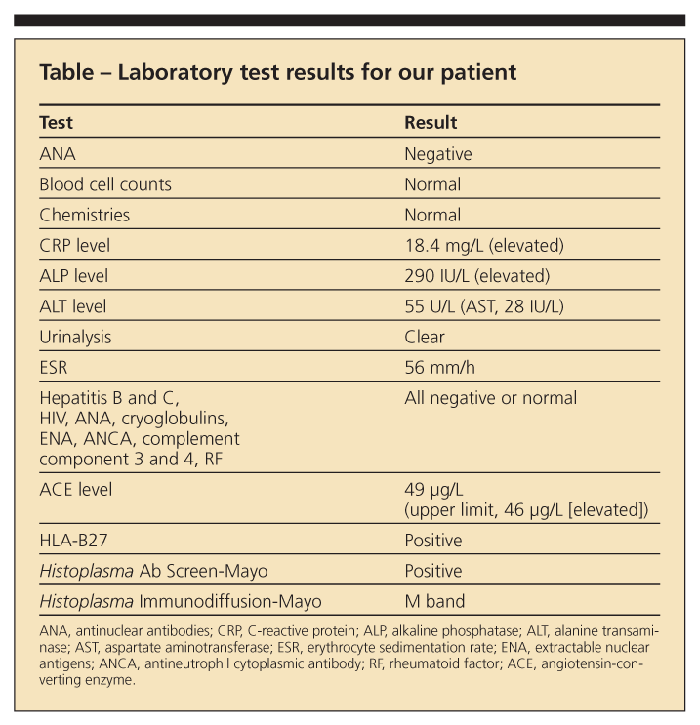
Laboratory tests during the patient's hospitalization (Table) revealed a normal complete blood cell count; negative blood cultures; a moderately elevated B-type natriuretic peptide level (451 pg/mL); urinalysis, 5 to 10 white blood cells per high-power field; erythrocyte sedimentation rate, 106 mm/h; and a positive ANA result of 1:40. The patient's alkaline phosphatase (ALP) level was as high as 558 IU/L; alanine transaminase (ALT) level, 110 U/L; and aspartate aminotransferase (AST) level, 137 IU/L. The results of more liver function tests done 10 days later were slightly better (ALP level, 494 IU/L; ALT level, 97 U/L; and AST level, 78 IU/L).
Assessment
The patient was awake and oriented. Her temperature was 36.9°C (98.5°F); pulse rate, 101; oxygen saturation level, 97%; and blood pressure, 148/94 mm Hg. She had a slightly scaly erythematous rash over her eyebrows. Neither alopecia nor scalp lesions were evident. She had mildly dry conjunctivae and a moist mouth, with no salivary or parotid gland enlargement. Her neck was supple, there was no lymph node enlargement, and her thyroid was not enlarged.
On examination, the patient's chest was clear. A heart examination revealed a systolic ejection murmur that was maximal at the apex, with an occasionally heard midsystolic click consistent with mitral valve prolapse. Abdomen findings were benign, with no organomegaly.
Examination of the extremities showed osteoarthritis changes, with no active synovitis in the hands; there was thenar atrophy consistent with carpal tunnel syndrome on the right. There also was mild crepitus in the right shoulder. The patient's right ankle was swollen and tender; there was erythema on the posterior aspect of her medial and lateral malleoli.
Differential diagnosis
Our initial impression was that the differential diagnosis included an infectious disease that the patient acquired while in El Salvador, perhaps a granulomatous disease, such as tuberculosis, histoplasmosis, or coccidioidomycosis.1,2 The second diagnostic possibility was that the patient had an existing autoimmune disease that flared because of the stress of travel. The rash was somewhat suggestive of systemic lupus erythematosus, although it also was compatible with dermatomyositis; both diagnoses would be compatible with the patient's Raynaud phenomenon and photosensitivity. The third possibility was reactive arthritis or a spondyloarthropathy, although it would be difficult to attribute all of her findings to any one of these diseases.
Diagnostic procedure
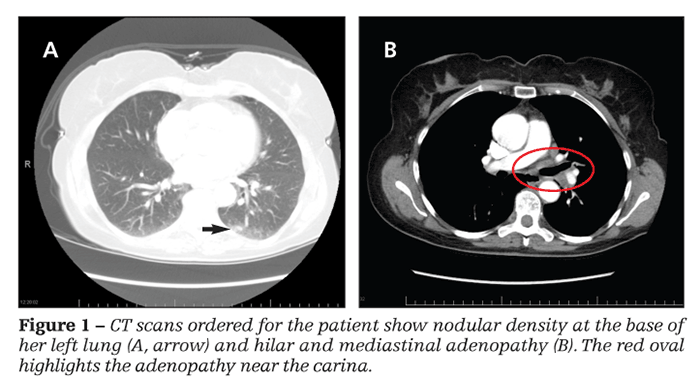
Aspiration of the patient's right ankle produced no fluid. CT scans of her abdomen and chest were ordered (Figure 1), along with x-ray films of her right ankle and both hands.
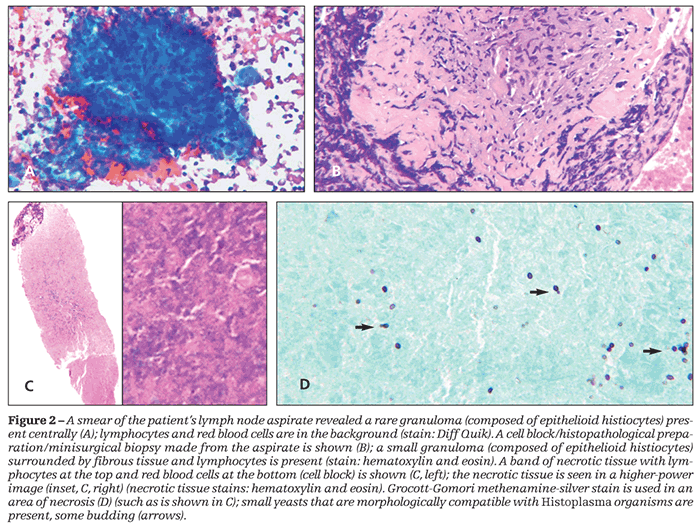
An endobronchial ultrasound-guided fine-needle aspiration biopsy of the paratracheal and hilar lymph nodes was performed with a cytopathologist on site (Figure 2). Histoplasma Ab Screen-Mayo and Histoplasma Immunodiffusion-Mayo laboratory tests were requested (see Table).
Diagnosis
On the basis of the patient's history of travel to El Salvador; clinical presentation; and endobronchial ultrasonography, CT, histopathology, and laboratory test results, a diagnosis of histoplasmosis was made. Additional information was provided by the CDC in the Morbidity and Mortality Weekly Report.3
A fungal disease caused by Histoplasma capsulatum, histoplasmosis may be acquired from soil contaminated with bird or bat droppings. The disease occurs worldwide and is one of the most common pulmonary and systemic mycoses in the United States. However, histoplasmosis is rare among international travelers returning from areas in which it is endemic.
In February and March 2008, the Pennsylvania and Virginia departments of health investigated a cluster of respiratory illnesses among 3 mission groups that had traveled to El Salvador separately to renovate a church. Of 33 travelers in the 3 groups for whom information was available, 20 (61%) met the case definition for histoplasmosis. A greater risk of illness was seen in persons who reported sweeping and cleaning outdoors (relative risk [RR], 2.1; 95% confidence interval [CI], 1.3-3.6), digging (RR, 2.6; CI, 1.1-6.1), or working in a bird or bat roosting area (RR, 1.8; CI, 1.3-2.4).
The findings emphasize the need for travelers and persons who are involved in construction activities to use personal protective equipment and decrease dust generation when working in areas in which histoplasmosis is endemic. Clinicians should consider histoplasmosis as a possible cause of acute respiratory or influenza-like illness in travelers returning from such areas.
It is especially important to consider histoplasmosis in patients with HIV infection, those with solid organ transplants, and those who are receiving tumor necrosis factor α–blocking therapy (adalimumab, infliximab, etanercept). Although this patient presented with somewhat typical hilar adenopathy, pulmonary infiltrates, arthritis, and constitutional symptoms, the clinical manifestations of histoplasmosis are protean. They include a whole range of dermatological findings (eg, erythema nodosum, papules, plaques, ulcers, and pustules), GI findings (eg, bleeding from ulcerative lesions or masses), adrenal insufficiency similar to other granulomatous diseases (eg, tuberculosis), and pleomorphic CNS diseases (eg, meningitis, focal granulomatous disease, or encephalitis).
Treatment
On February 16, 2009, after test results came back positive for H capsulatum, the patient was treated with itraconazole, 200 mg, 3 times a day for 3 days, then 200 mg/d for 6 to 12 weeks. She made a full recovery, except in her right ankle, which remained swollen. That was thought to be the result of reactive arthritis; the patient responded to sulfasalazine and achieved a full recovery.
References:
References1. Panackal AA, Hajjeh RA, Cetron MS, Warnock DW. Fungal infections among returning travelers. Clin Infect Dis. 2002;35:1088-1095.
2. Freedman DO, Weld LH, Kozarsky PE, et al; GeoSentinel Surveillance Network. Spectrum of disease and relation to place of exposure among ill returned travelers [published correction appears in N Engl J Med. 2006; 355:967]. N Engl J Med. 2006;354:119-130.
3. Outbreak of histoplasmosis among travelers returning from El Salvador-Pennsylvania and Virginia, 2008. MMWR. 2008;57:1349-1353.