A Decade to Diagnose axSpA
Delays in diagnosing axSpA are troubling, write the authors of a report in the journal Rheumatology. Delays of up to 10 years have been reported. Not all physicians may be familiar with the signs and symptoms of axSpA.
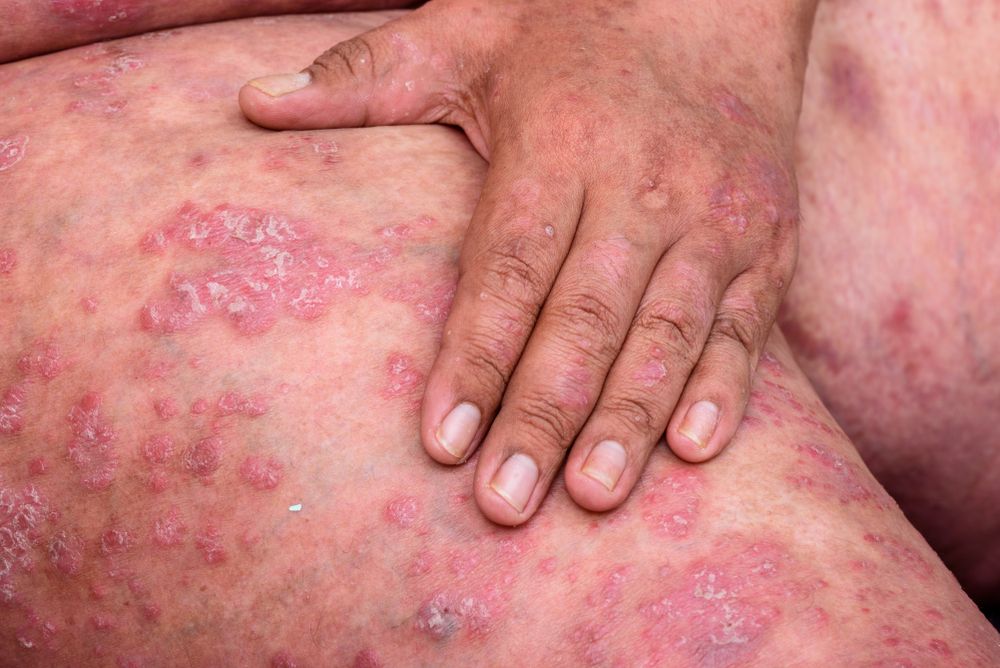
It is not unusual for cases of axSpA to be diagnosed about 10 years after symptoms manifest, a new report shows. Psoriasis is one of those symptoms. Do you know the others? (©SweetheartStudioShutterstock.com)
In a recent article published in the journal Rheumatology, Imke Redeker and colleagues in Germany report that even with recent advances in diagnosing axial spondyloarthritis (axSpA), diagnostic delays are still too long.
Axial spondyloarthritis is a term that encompasses both ankylosing spondylitis and nonradiographic axial spondyloarthritis-which is essentially early stage ankylosing spondylitis before structural damage, such as sacroiliitis or spinal syndesmophyte, is visible radiographicly.
Delays in diagnosing axSpA can be as long as five to 10 years after onset. The authors write that early diagnosis of axSpA is crucial for initiation of optimal treatment.
The Assessment of SpondyloArthritis International Society (ASAS) diagnostic criteria suggest that physicians rely less on plain radiographic changes to identify changes in bone to make a diagnosis. Magnetic resonance imaging of the sacroiliac joint may lead to an earlier diagnosis and treatment.
The authors of the report sought to determine the extent of diagnostic delays in axSpA.
THE STUDY
Data for this study were obtained from the Linking Patient-Reported Outcomes with CLAIms data for health services research in Rheumatology (PROCLAIR) network. PROCLAIR is a randomized sample of patients in Germany with asSpA. All subjects received questionnaires where they relayed the date of SPA-related symptom onset and the date of diagnosis.
Both univariate and multivariate analyses were performed looking at age at symptom onset; HLA-B27 status; presence of psoriasis, uveitis or inflammatory bowel disease as well as educational level.
2,082 respondents consented to participate with 1,776 confirming the date of symptom onset and 1,677 further supplying the date of axSpA diagnosis as well. Ultimately, this cohort of 1,677 respondents was included in the final analysis.
Younger women with psoriasis who did not carry the HLA-B27 gene were more likely to experience the longest diagnostic delay of more than five years. In addition, patients with higher educational levels were often diagnosed later than those with lower educational levels.
Diagnostic delay was not significantly different between patients diagnosed between 1996 and 2001 and those diagnosed between 2006 and 2015 uncovering a lack of improvement over time. Multivariate analysis confirmed the relationship between young age, psoriasis, female gender, and lack of HLA-B27 genotype with longer diagnostic delays in axSpA.
See the next page for an analysis by Dr. Weiss.
TAKE-HOME POINTS FOR CLINICIANS AND FINAL THOUGHTS
The authors found a mean diagnostic delay of 5.7 years with a median of 2.3 years for axSpA. The authors found no real improvement over time even with advances in diagnostic modalities and refined criteria.
The authors point out that more time may be needed to observe an improvement in the diagnostic delay related to the focus on early diagnosis provided by the Assessment of Spondyloarthritis International Society classification criteria published in 2009.
HLA-B27 screening may be an important obstacle to early diagnosis since primary care physicians may use it when patients present with early symptoms of axSpA. This study found that HLA-B27 negativity lead to a lower probability of being referred to a rheumatologist as well as a lower likelihood of being diagnosed with axSpA.
Women often have non-radiographic disease earlier, which may account for the greater delay in diagnosis of axSpA when compared to men.
Psoriasis, a manifestation of axSpA, is often diagnosed by a dermatologist who may not refer these patients to a rheumatologist for further evaluation leading to the delays seen in diagnosing axSpA in patients presenting with skin manifestations.
Younger patients may experience delays in diagnosis of axSpA due to the myriad of other functional reasons they may have for back pain.
Persistent delays in diagnosing axSpA are troubling, the authors wrote. This research highlights the challenges rheumatologists face even with steady advances in diagnosis and treatment. One such hurdle is a less than streamlined referral process.
Currently, the referral model uses the primary care physician as a gatekeeper of sorts where patients present with symptoms leaving it up to them to sort them out among an often large number of differential diagnoses. The authors suggest, and I agree, that referral strategies should be developed triggering notifications to specialists in rheumatology when patients present with symptoms of axSpA to primary care clinicians and dermatologists.
ABOUT THE AUTHOR
Gregory M. Weiss, M.D., is a cardiothoracic anesthesiologist practicing in Virginia. He is a frequent contributor to Rheumatology Network.
REFERENCE
Imke Reeker, Johanna Callhoff, Falk Hoffmann, et al. Determinants of diagnostic delay in axial spondyloarthritis: an analysis based on linked claims and patient-reported survey data. Rheumatology, kez090, https://doi.org/10.1093/rheumatology/kez090
Axial Spondyloarthritis Defined, AJMC, December 2018.