Fewer Than Half of Psoriatic Arthritis Patients Report Obvious Side Effects
Many patients with psoriatic arthritis live with unacceptable levels of disease activity despite treatment, and patient-reported outcomes could provide useful treatment targets, shows a new study.
(©Snab,AdobeStock)
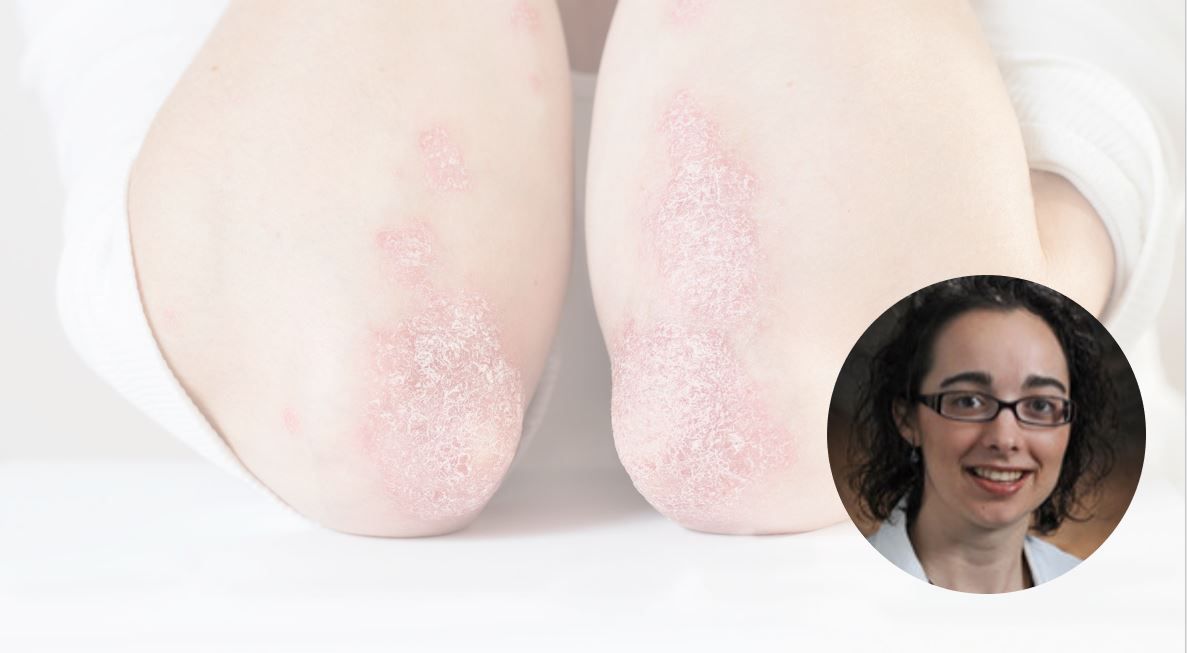
The burden and impact on quality of life of treatments for psoriatic arthritis and their failure to provide complete remission are not given enough attention by healthcare providers and greater use of patient reported outcomes measures could be used to highlight these issues and provide treatment targets, according to researchers reporting at the annual meeting of the American College of Rheumatology on Friday November 6.
Two studies presented by Alexis Ogdie-Beatty, M.D., MSCE, from the Perelman School of Medicine at the University of Pennsylvania, Philadelphia, highlighted many of the ongoing issues faced by patients treated for psoriatic arthritis.
“Physicians often consider adverse events when choosing therapies for psoriatic arthritis and rheumatoid arthritis but may give less attention to other ways in which treatments affect the well-being of patients, such as impacts on quality of life, barriers to access, and challenges with taking medications,” she said.
Dr. Ogdie and colleagues looked at patients’ perspectives on the treatment burdens of the most commonly used therapies―methotrexate and TNF inhibitors―through interviews with 24 patients with rheumatoid arthritis and 25 patients with psoriatic arthritis. Nine types of treatment burdens were identified by the patients, who were aged 45-85 years and mostly female side effects, managing side effects, psychological, daily functioning, taking medications, accessing medications, economic impact, work, and family planning/breastfeeding.
Fewer than half of patients reported seeking or receiving medical attention to address side effects, despite the majority of those on methotrexate having to take steps to manage nausea, fatigue, mouth sores, or hair loss which impacted on their quality of life, daily functioning and work. Three-quarters of patients taking TNF inhibitors experienced difficulties accessing, paying for, or taking them.
Discontinuing medication because of lack of effectiveness was more common among patients with psoriatic arthritis than those with rheumatoid arthritis.
It is common for patients with psoriatic arthritis in the United States to fail to achieve remission, and unacceptable symptom states are often accompanied by depression and impaired social interaction, showed another study presented by Dr. Ogdie, which was based on survey data from The National Psoriasis Foundation (NPF).
Data on 801 patients reporting a diagnosis of psoriatic arthritis from a healthcare provider and who had completed the Psoriatic Arthritis Impact of Disease 9 (PsAID-9) revealed that six in ten (59.6%) experienced an unacceptable level of disease activity (PSAID >4). Those with a significant level of unacceptable disease activity were significantly more likely than those with acceptable levels to report depression (2.56 [SD 2.00] vs 0.08 [SD 1.25], p≤.0010 and inability to participate in social activities (mean T-scores 44.56 [SD 6.83] vs 55.46 [SD 6.99], p≤.001).
Greater awareness of treatment burdens experienced by patients with psoriatic arthritis, which were rarely addressed in clinical trials or observational studies, might help healthcare providers better support patients with any medication-related challenges that they encountered, Dr. Ogdie said.
Several different composite instruments can be used to define low disease activity and remission targets for treatment in patients with psoriatic arthritis, but another study highlighted that many patient-reported outcomes (PROs) correlate well with these measures so could also be used.
Using composite indices as the reference standards, the research team which included Dr. Ogdie, compared the performance of various patient-reported outcomes measures, including Patient-Reported Outcomes Measurement Information System (PROMIS) instruments, EULAR Psoriatic Arthritis Impact of Disease (PSAID12), and Routine Assessment of Patient Index Data 3 (RAPID3), in 227 patients.
Compared to patients with low disease activity patients in remission had significantly more favorable PROMIS Physical, PROMIS Mental, PROMIS Fatigue, and PSAID12 scores, and correlations with the composite indices were strong for PROMIS GH physical health (r=0.65- 0.69) and PSAID12 (r=-0.77- 0.79).
Use of patient reported outcomes to measure low states of disease activity should be considered for additional treatment targets in psoriatic arthritis, said Juliette Yedimenko from the Cleveland Clinic, Cleveland, who presented the findings. “RAPID3 Near-Remission may be the most rigorous PRO criteria (including only the lowest states of disease activity), while PSAID Patient Acceptable State may identify a broader range of low states of disease activity,” she added.
___________________
REFERENCES
ABSTRACT 0148. “Perspectives on Treatment Burden for Methotrexate and TNF-inhibitors Among Psoriatic Arthritis and Rheumatoid Arthritis Patients: A Qualitative Study.” The annual meeting of the American College of Rheumatology. 9:00 AM, Friday, Nov. 6, 2020.
ABSTRACT 0166. “Prevalence and Impact of Unacceptable Symptom State Among Patients with Psoriatic Arthritis: Results from the National Psoriasis Foundation’s 2019 Annual Survey.” The annual meeting of the American College of Rheumatology. 9:00 AM, Friday, Nov. 6, 2020.
ABSTRACT 0169. “Patient-Reported Outcomes Differentiate Between Remission and Low Disease Activity in Psoriatic Arthritis.” The annual meeting of the American College of Rheumatology. 9:00 AM, Friday, Nov. 6, 2020.