Gout Attacks Intensify with Heart Failure
ACR Annual Meeting: Gout patients who are admitted to the hospital with worsening heart failure, go on to have gout attacks during hospitalization leading to longer hospital stays, researchers reported November 10 at the annual meeting of the American College of Rheumatology in Atlanta.
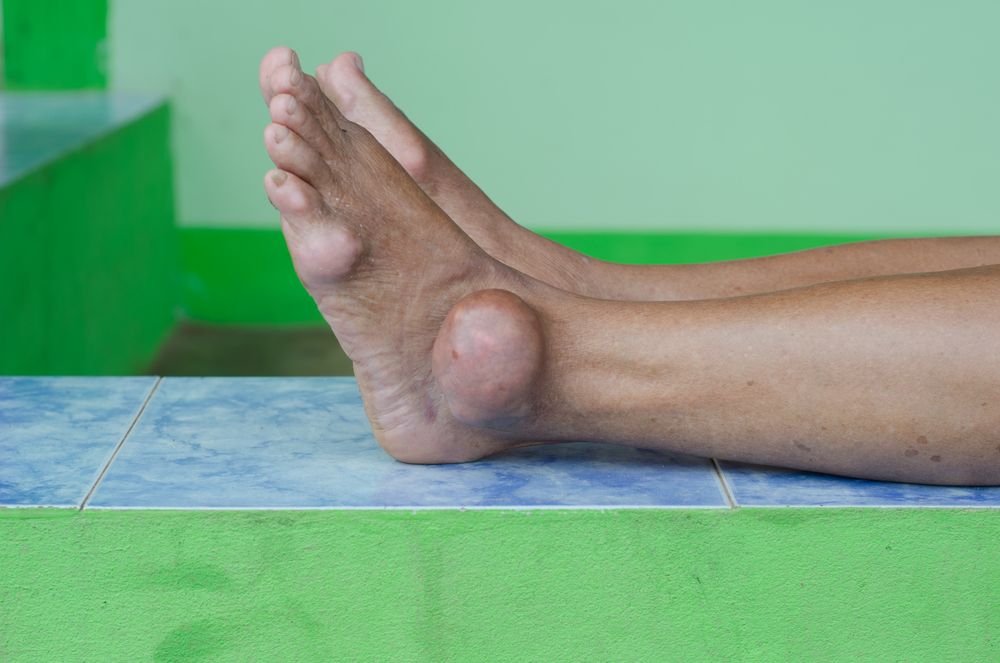
(Foot with gout. ©joloeiShutterstock.com)
Gout patients who are admitted to the hospital with worsening heart failure, go on to have gout attacks during hospitalization leading to longer hospital stays and higher use of healthcare resources, researchers reported November 10 at the annual meeting of the American College of Rheumatology in Atlanta.
Diuretics are sometimes recommended for heart failure patients, but they can lead to secondary hyperuricemia which can trigger a gout attack.
“Even though we know how to treat gout in the outpatient setting, there’s a lot of room for improvement in the prevention and treatment of inpatient gout flares,” said Estefania Gauto-Mariotti, MD, who presented the research. She is a postgraduate physician in the Internal Medicine Residency Program at the John H. Stroger Hospital of Cook County in Chicago.
Using data from the National Inpatient Sample, Dr. Gauto-Mariotti and colleagues used ICD-9-CM codes to identify patients admitted for a principal diagnosis of heart failure who then had a secondary diagnosis of acute gouty arthropathy during hospitalization.
The researchers identified 1,130,374 adults admitted for heart failure between 2009 and 2015; 4116, or 0.4%, had a gout attack during admission. Those who developed gout were younger (67.9 vs 61.7 years) and had a higher prevalence of alcohol abuse, iron deficiency anemia, coagulopathy, diabetes, and obesity (all p <0.05). Significant predictors of gout attack found with multivariate logistic regression analysis were chronic kidney disease (p<0.001), chronic alcohol use (p<0.004), obesity (p<0.0001), and dyslipidemia (p<0.001).
Compared with not having an attack, having a gout flare increased the risk of acute kidney injury (43.8% vs 22%, p<0.001). Gout attacks also lengthened hospital stays (6 days vs 4 days; p<0.001) and upped total hospital costs ($9,999 vs $6,941; p< 0.001), though only 8.9% of patients who had a gout attack received an intra-articular joint injection or arthrocentesis.
“The two-day difference in hospital stay has a major impact on resource utilization. Our findings indicate that higher costs aren’t due to gout-related interventions but to daily baseline costs that add up as hospital stays prolong,” said Gauto-Mariotti. “Gout exacerbation is a common finding in concomitant heart failure comorbidity; in spite of this, further research is needed to demonstrate objective data in terms of negative impacts on heart failure hospitalizations.”
REFERENCES
ABSTRACT 330 - “Acute Gout Attacks Among Patients Admitted Due to Heart Failure: Analysis of NIS Database,” Estefania Gauto-Mariotti, M.D., 9 a.m., Sunday, Nov 10. American College of Rheumatology 2019 annual meeting, Atlanta.