Hand Pain and Swelling in a 63-Year-Old Woman
A 63-year-old woman presented with a 2-year history of bilateral hand pain and stiffness that had worsened in recent months. The pain was most severe in the fingers and was associated with morning stiffness that lasted 30 minutes. There was loss of full range of motion in some finger joints.
A 63-year-old woman presented to our rheumatology clinic with a 2-year history of bilateral hand pain and stiffness. The pain was most severe in the fingers and was associated with morning stiffness that lasted 30 minutes. The symptoms had worsened over the past few months, and there was loss of full range of motion in some finger joints.
The woman’s past medical history was unremarkable. She had experienced menopause about 15 years earlier. She reported that her mother had had similar problems with her hands. The patient
denied smoking and alcohol use. She was an avid traveler and enjoyed hiking and scuba diving.
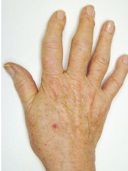
Physical examination showed prominent bony enlargements of multiple proximal interphalangeal (PIP) and distal interphalangeal (DIP) joints bilaterally; some were tender to palpation. There was no synovitis, nail pitting, or onycholysis (see photo above). The patient could not make a complete closed fist.

Laboratory test results showed an erythrocyte sedimentation rate (ESR) of 20 mm/h (normal range, 0 to 20 mm/h) and a C-reactive protein level of less than 0.4 mg/dL (normal range, 0 to 0.8 mg/dL). Rheumatoid factor (RF) was absent, and anticyclic citrullinated peptide (anti-CCP) antibody was 0 units (normal range, 0 to 20 units).
A complete blood cell count was obtained at another institution; the results were normal. An x-ray film of the hand showed joint-space narrowing in all the interphalangeal joints with erosions at the second through fifth PIP joints.
What is your diagnosis?
(Find the answer on the next page.)
The patient had erosive osteoarthritis (EOA), a somewhat uncommon condition of unknown origin.1 Typically, EOA affects the hands of postmenopausal middle-aged women, producing abrupt pain, swelling, and tenderness of the DIP and PIP joints.
EOA is a severe and debilitating condition that initially may be mistaken for an inflammatory arthropathy. There are no well-established diagnostic criteria for EOA; diagnosis is based on clinical assessment and characteristic radiographic findings.
Patients with EOA typically present with complaints of hand pain, tenderness, erythema, and
warmth and with morning stiffness of less than 30 minutes’ duration. Patients may also experience nocturnal throbbing paresthesias.The symptoms appear to be more persistent than the symptoms in OA.
Although the distribution of the arthritis mainly involves the PIP and DIP joints, the first metatarsophalangeal joint also is commonly affected; the hips, shoulders, and toes are rarely involved.2 The disease often leads to joint deformities that may be clinically indistinguishable from those involving inflammatory arthropathies.1 In some cases, the progression of EOA leads to instability and ankylosis of the DIP and PIP joints that are seen almost exclusively in this disease.3

Radiographic findings show joint-space narrowing followed by a sharply marginated defect in the central surface of the bone that sometimes is associated with a “crumbling erosion.” Progression leads to a “gull wing” deformity that is the result of marginal sclerosis and osteophytes of the distal side of the joints. On the proximal side, a characteristic “sawtooth”erosion most often leads to ankylosis. Although the presence of erosions is a hallmark for diagnosis of EOA, bony proliferations may be absent.1
In the early stage of EOA, the synovium reveals an intense proliferative change as is seen in rheumatoid arthritis (RA), with lymphocyte aggregates, hypertrophy, and hyperplasia. As the disease progresses, a noninflammatory phase appears, which includes fibrosis and cartilage degeneration that is more consistent with OA.1
Numerous studies have demonstrated that EOA is a unique entity, separate from the other inflammatory arthropathies (eg, RA), and probably is a subset of OA. However, whether there is a relationship between EOA and OA is controversial. The most notable difference between EOA and OA is in the presence of radiographic erosions. Generalized OA exhibits flares at the onset of involvement of each joint; typically, EOA involves several joints simultaneously, is characterized by more inflammatory episodes, and may persist for many years.1
Of the inflammatory arthropathies, EOA most resembles psoriatic arthritis (PsA) clinically and radiographically. Both conditions preferentially affect the DIP joints. In PsA, however, usually there is involvement in other sites, particularly the spine and sacroiliac joints. In addition, erosions are marginally located with coexistent periostitis in PsA but not in EOA.
Radiographic findings in EOA, particularly the sparing of the metacarpophalangeal joints, usually
are sufficient to differentiate between it and RA. In addition, serologic markers that are specific for RA, such as anti-CCP antibody, are absent in EOA.
Other conditions that may resemble EOA include arthropathies associated with endocrine diseases and diseases induced by crystal deposition. Laboratory studies (eg, anti-CCP antibody,RF, complete blood cell count, basic metabolic panel, and ESR) usually yield results that are unremarkable in EOA and help exclude these conditions.
The therapeutic approach to EOA has been varied, and the results often are disappointing. Regimens of NSAIDs have been tried, with limited effectiveness. Joint injections with corticosteroids may offer temporary relief, but the need for subsequent injections in multiple affected joints precludes their routine use. Results of treatment with glucosamine/chondroitin
sulfate and hydroxychloroquine have been mixed. Surgical intervention-including synovectomy and arthrodesis-may offer the best results.1
The patient was given hydroxychloroquine, 200 mg twice daily, in addition to the acetaminophen, 1000 mg twice daily, that she was already taking. A follow-up is scheduled in a few months.
This case was submitted by Juan Contreras, MD, department of internal medicine, and Michelle Eisenberg, MD, and Prashanth Sunkureddi,MD,division of rheumatology, at the University of Texas Medical Branch in Galveston
References:
1. Punzi L, Ramonda R, Sfriso P. Erosive osteoarthritis. Best Pract Res Clin Rheumatol. 2004;18:739-758. 2. McKendry RJ. Nodal osteoarthritis of the toes. Semin Arthritis Rheum. 1986;16: 126-134. 3. Belhorn LR, Hess EV. Erosive osteoarthritis. Semin Arthritis Rheum. 1993;22:298-306.