Injection therapy for pelvic soft tissue conditions
Soft tissue musculoskeletal conditions are common causes of pelvic and lower extremity pain.
Soft tissue musculoskeletal conditions are common causes of pelvic and lower extremity pain. Injection therapy may provide relief in 2 of these conditions-piriformis syndrome and greater trochanteric pain syndrome (GTPS), or trochanteric bursitis-but a required step in the procedure for both conditions is identification of the greater trochanter of the femur. In this article, we describe the appropriate injection techniques.
Clinical syndromes
•Piriformis syndrome: The piriformis muscle lies deep in the gluteal region. It originates from the anterior sacral surface and then passes through the greater sciatic notch to insert on the greater trochanter of the femur, aiding in external rotation of the hip. Closely proximate to the piriformis is the sciatic nerve, although its relative position varies: its 2 major divisions (portions destined to be the tibial and common peroneal nerves) may both pass anterior and inferior to the muscle (in 85% of cases), split with either one (10% of cases) or both (fewer than 1% of cases) branches passing through the muscle, or split and encircle the muscle (2% to 3% of cases).1 Contraction or compression of the piriformis muscle can lead to an entrapment neuropathy of the sciatic nerve (piriformis syndrome).
Patients with piriformis syndrome may note paralumbar, sacral, buttock, and leg pain. Pain may radiate down the leg, suggesting lumbar sciatica; this accounts for about 5% of sciatica presentations. The pain may be aggravated by lifting or stooping, direct muscle compression from prolonged sitting on a hard surface, or excessive leg activities that require rotation of the hip. Examination may reveal pain and tenderness to deep palpation in the midbuttock just lateral to the sciatic notch. Straight-leg raising test results may be positive. Pain may be exacerbated with forced-passive-internal or resisted-external hip rotation.
Injection of the piriformis muscle can be challenging because of its proximity to the sciatic nerve and its anatomical variations. These factors increase the risk of inducing a sciatic nerve block. The risk must be discussed with the patient during the informed consent process.
•GTPS: There are 3 constant bursae surrounding portions of the anterior, lateral, and posterior regions of the greater trochanter; they serve to promote smooth gliding movements of the gluteal muscles and the tensor fascia lata. Pain in this region may arise from direct trauma or chronic pressure, from exaggerated movements of the gluteal muscles (especially the gluteus medius) and the tensor fascia lata over the trochanter, and from conditions that alter lower extremity biomechanics and thus gluteal muscle function. Radiographic evaluation of patients affected with trochanteric bursitis only rarely shows swelling of the bursae. MRI scans more frequently show degrees of gluteal muscular or insertion tears or tendinosis, hence the preferred term greater trochanteric pain syndrome.2,3
GTPS is more common in women than in men and is the most common cause of "hip pain" in older patients. Patients complain of pain that is over the lateral aspect of the hip that may radiate toward but rarely below the knee. It may be aching, intermittent, or chronic, and it may be exacerbated by prolonged standing, direct pressure (such as during sleep), or activities that lead to hip external rotation or abduction (such as leg crossing). Symptoms may be perceived as pain in the lower back region in some patients and as a nondermatomal-like paresthesia and numbness in the upper thigh.
Examination elicits point tenderness over the greater trochanter with variable degrees of tenderness over the upper third of the lateral and posterior thigh. Palpable warmth, swelling, and erythema usually are not observed. Passive internal rotation or resisted external rotation or abduction of the hip may reproduce the pain. Passive hip flexion and extension usually is painless, but acute trochanteric bursitis may limit passive motion.
Suggested supplies
•Ethyl chloride spray (if preferred for superficial anesthesia).
•3-mL syringe with 2 to 3 mL of 1% lidocaine for local anesthetic.
•10-mL syringe with 5 to 7 mL of 1% lidocaine admixed with 20 to 40 mg (0.5 to 1 mL) of a nonfluorinated corticosteroid (eg, methylprednisolone, 40 mg/mL).
•1.5-inch, 25-gauge needles for injection of anesthetic and corticosteroid-anesthetic mixture. For patients of large body habitus, have 3.5-inch 22-gauge spinal needles available.
•Alcohol wipes, povidone-iodine, or chlorhexidine for sterilization.
•Sterile hemostat (optional).
•Nonsterile or sterile gloves.
•Gauze pads and adhesive bandage.
Surface anatomy
•Piriformis syndrome: The midbelly of the piriformis lies lateral to the sciatic notch, about halfway along a line that joins the posterior superior iliac spine and the greater trochanter of the femur.
•GTPS: The insertion sites of the gluteal muscles and the trochanteric bursae lie along the lateral and posterior portions of the greater trochanter of the femur.
Patient position and needle placement
•Piriformis syndrome: Place the patient in a prone position and draw a line from the posterior superior iliac spine to the greater trochanteric prominence on the lateral hip. The midpoint of this line is the point of needle insertion.
•GTPS: Place the patient in the lateral position, hips and knees slightly flexed, with the affected hip pointing upward. Palpating from the midthigh cephalad, insert the needle at the point of maximal tenderness over the bony trochanteric prominence.
Procedure
•Piriformis syndrome: For all needle insertions, instruct the patient to tell you if you induce a radiating paresthesia down the leg. After proper skin sterilization, anesthetize the skin and needle tract using a 25-gauge, 1.5-inch needle. Direct the needle toward the umbilicus to its full depth, injecting lidocaine along the path. In very thin patients, the periosteum of the ilium may be reached and should be numbed. Preload the 10-mL syringe with the corticosteroid-anesthetic mixture.
If the periosteum was reached during anesthesia, then a 25-gauge needle also may be used for injecting the corticosteroid mixture: insert the needle into the periosteum, then withdraw it by 3 to 5 mm and inject the contents of the syringe. If the periosteum was not reached during anesthesia, then a spinal needle is used for injecting the corticosteroid mixture: with the stylet in, insert the needle to its full depth, withdraw the stylet and attach the syringe, then inject. If spinal needle contact is made with the periosteum, withdraw the stylet and attach the syringe, then withdraw the needle by 3 to 5 mm before injecting the syringe contents.
•GTPS: After proper skin sterilization, anesthetize the skin and needle tract using a 25-gauge, 1.5-inch needle (Figure). In thin patients, the periosteum of the trochanter may be reached and should be numbed. Preload the 10-mL syringe with the corticosteroid-anesthetic mixture.
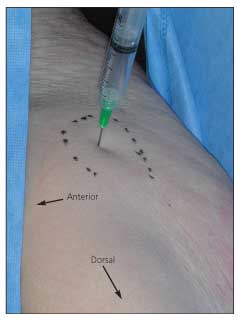
Figure – Injection of the left trochanteric bursal region is shown in this cadaver photograph. In the lateral position with the patient’s hip and knee slightly flexed, the needle enters at the point of maximal tenderness over the bony trochanteric prominence (outlined in black) at a 90° angle to the skin.
If the periosteum was reached during anesthesia, then a 25-gauge needle also may be used for injecting the corticosteroid mixture: insert the needle into the periosteum, then withdraw it by 2 to 3 mm and inject the contents of the syringe. If the periosteum was not reached during anesthesia, then a spinal needle is used for injecting the corticosteroid mixture: with the stylet in, insert the needle to make contact with the periosteum. Withdraw the stylet and attach the syringe, then withdraw the needle by 2 to 3 mm and inject the syringe contents. For patients with a history of lateral thigh radiation of pain, one-half to two-thirds of the syringe contents are injected at the trochanter and the remainder is distributed distally in a fan pattern into the deep lateral thigh without removing the needle from the skin.
References:
References1. Travell JG, Simons DG. Piriformis and other short lateral rotators. In: Travell JG, Simons DG, eds. Myofascial Pain and Dysfunction: The Trigger Point Manual. Vol 2. Baltimore: Williams and Wilkins; 1992:201.
2. Shbeeb MI, Matteson EL. Trochanteric bursitis (greater trochanteric pain syndrome). Mayo Clin Proc. 1996;71:565-569.
3. Alvarez-Nemegyei J, Canoso JJ. Evidence-based soft tissue rheumatology: III: trochanteric bursitis. J Clin Rheumatol. 2004;10:123-124.