Management of Plantar Fasciitis Evolving
Initial treatment of plantar fasciitis is based on finding ways to reduce stress applied to the plantar fascia. Surgery for plantar fasciitis may be indicated if prolonged attempts at nonoperative correction are unsuccessful.
ABSTRACT: Initial treatment of patients with plantar fasciitis is based on an understanding of the functions of the plantar fascia and the methods for reducing stress applied to it. The differential diagnosis of heel pain may be narrowed by carefully identifying the area of tenderness. There is little scientific evidence to indicate that traditional approaches to treatment substantially improve patients’ long-term outcome, but spontaneous improvement and resolution are common. A rational approach to treatment begins with identifying the possible causes of connective tissue irritation. If specific problems can be identified, a strategy designed to correct these factors should be planned. Surgical release is indicated for severe plantar fascial pain after prolonged attempts at nonoperative treatment. Many intriguing new approaches to treatment-resistant plantar fasciitis are under investigation. (J Musculoskel Med. 2012;29:16-20)
Heel pain, including that caused by plantar fasciitis, is a common reason why patients seek evaluation from a doctor. The impairment that results from heel pain often is a nuisance, and the pain can be so exquisite and disabling that it interferes with the patient’s recreational, work, and social activities. Initial treatment may be instituted by a variety of doctors, including family physicians, internists, physiatrists, orthopedists, and podiatrists.
Plantar fasciitis is a common and painful heel disorder. Initial treatment is centered on an understanding of the important functions of the plantar fascia and the methods for reducing the stress that is applied to it with daily activities. Exciting new treatment methods are on the horizon. In many cases, however, the high-grade scientific evaluation that is necessary for widespread application of these methods is not yet available. In this article, I provide an update on the latest approaches to the diagnosis and management of plantar fasciitis.
DIAGNOSIS
The Mechanics of the Arch
Arch mechanics are centered on the plantar fascia.1 The architecture of the midfoot bones has no inherent stability. Pressure applied to the forefoot in the absence of connective tissue support leads to shearing and displacement of the joints. The intrinsic plantar ligaments closely line the inferior surface of the midfoot (Figure 1). Although the integrity of the intrinsic ligaments is crucial to the posture of the arch, these ligaments do not have sufficient leverage or size to stabilize the midfoot against the magnitude of body weight.
FIGURE 1
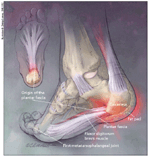
Hicks2 described the windlass model of arch stability. The plantar fascia inserts onto the forefoot into the plantar plates of the metatarsophalangeal joints and by extension into the base of the proximal phalanx of each toe. This causes the plantar fascia to tighten when the toes are dorsiflexed. The tightness accentuates and stiffens the arch at the end of the step (Figure 2). Because the first metatarsal head is the largest in diameter, the plantar fascia attached to the hallux tightens more; thus, the arch is more accentuated on the medial foot, causing the foot to invert.
FIGURE 2
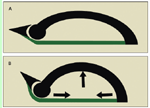
When combined with the force of forefoot pressure, the tension within the plantar fascia redirects the force along the axis of the bones. This redirection reduces shear stresses across the foot that would otherwise lead to stress fractures and premature arthritis in the midfoot.
This function is shared by the foot’s intrinsic muscles, which, like the plantar fascia, stabilize the arch by linking the heel to the toes. One study that evaluated arch function demonstrated a 3.2-mm drop in the height of the navicular from the floor when the intrinsic muscles were paralyzed in vivo.3 The health and conditioning of these muscles may be a factor responsible for the development of arch pathology and plantar fasciitis that is not well recognized.
Differential Diagnosis
Although plantar fasciitis is the predominant source of heel pain, a few of the less common reasons for heel pain also should be kept in mind (Table). The differential diagnosis of heel pain may be narrowed by carefully identifying the area of tenderness. Tenderness with stress fractures of the calcaneus usually is palpable circumferentially around the tuberosity of the calcaneus.
TABLE

Differential diagnosis for heel pain
Pain resulting from neuritis of branches of the posterior tibial nerve occurs medially and along the superior border of the intrinsic musculature or along the posteromedial aspect of the ankle. A percussion sign may elicit pain that radiates into the sensory distribution of the nerve, the plantar forefoot, or the heel.
Connective tissue damage in the plantar fascia usually is located somewhat discretely at the insertion of this structure along the anterior and medial aspect of the weight-bearing portion of the heel. The tenderness also may be appreciated at the central or lateral portion of the heel. In some cases, it may extend distally along the medial band into the longitudinal arch.
The diagnostic value of plain radiographs of the heel has been questioned.4 In practice, these studies rarely change treatment decisions. However, the use of radiographs in the management of musculoskeletal disorders has become so routine that some discussion with the patient about their appropriate use may be necessary to explain their omission. If the pain is not improving progressively or if invasive treatment is planned, radiographs certainly should be obtained to rule out extremely rare abnormalities that may alter the treatment plan, although the finding of a heel spur provides little help in selecting the best management of this disorder.
More advanced radiographic studies, such as MRI, CT, ultrasonography, and nuclear medicine, are rarely necessary and their use should be confined to cases in which there is confusion in the diagnosis. For example, fibromyalgia syndrome (FMS) is common in patients who present with heel pain,5 possibly making the physical examination results less reliable. Although surgery may be helpful for patients with FMS, a more aggressive radiological evaluation may be prudent in the selection of patients for surgical treatment.
Causes
Deterioration of the plantar fascia occurs for many reasons. Connective tissue deterioration is associated with many systemic factors that alter microcirculation within tissue, such as the patient’s age, arteriosclerosis, lipid abnormalities, tobacco abuse, and diabetes mellitus. Rheumatoid arthritis, ankylosing spondylitis, and other seronegative arthropathies can be associated with plantar fasciitis and other enthesopathies.
Some predisposing factors relate to the biomechanical environment of the ligament. Mechanical overload of the plantar fascia has been suspected to play a significant role in the development of plantar fasciitis. Several studies have identified associations of plantar fasciitis with obesity and poor ankle flexibility; both of these factors would be expected to add to the mechanical load of the forefoot.
The plantar fascia also may be damaged by direct impact on the heel through gait or repetitive trauma to or overloading of the front of the foot through gait abnormalities, posture, and other tendon contractures (eg, hamstring tendon contractures). Damage to other supporting structures that assist in arch stabilization may increase the stress on the plantar fascia; this may include injuries to the posterior tibial tendon or intrinsic plantar ligaments, resulting in acquired flatfoot deformity, or “fallen arches,” and instability caused by midfoot arthritis. The intrinsic musculature may be compromised in many ways, including weakness resulting from compressive or peripheral neuropathy and deconditioning because of the patient’s age or the use of overprotective footwear or arch supports.
TREATMENT
Conservative Approaches
There is little scientific evidence to indicate that traditional approaches to treatment substantially improve patients’ long-term outcome. The natural history of plantar fasciitis is unknown. Nearly all accepted conservative therapies yield a high success rate. As a result, large study sizes are necessary to identify statistically significant differences in effectiveness. However, studies of this size and quality are rare in clinical medicine.
A rational approach to management of plantar fasciitis begins with identification of the possible causes of the connective tissue irritation. If specific problems can be identified, a strategy designed to correct these factors should be planned.
If the discomfort from the plantar fasciitis is not severe, a good starting point is a program that includes weight loss, simple stretching exercises, and mechanical protection of the plantar fascia. Casting has been shown to be highly effective for severe pain.6 Although immobilization leads to deconditioning of the musculature and mechanical weakening of the plantar fascia, it seems to help resolve severe, acute pain.
Exercise therapy is an effective approach. Hamstring and Achilles contractures have been associated with the development of plantar fasciitis, and stretching programs have been a mainstay of treatment. Most programs focus on improving the flexibility of these muscles. Stretches that concentrate on the plantar fascia seem to increase the effectiveness of standard stretching programs over the short term.
Conditioning exercises for the foot help relieve stress on the plantar fascia by strengthening supporting structures. Although deep tissue massage techniques are used frequently, they have not been proved to be effective. Therapeutic ultrasound and other modalities have not been shown to be useful.
There has been a lot of experience with braces that maintain the ankle in a neutral or slightly dorsiflexed position at night, and several prospective trials have shown improvement with their use over several weeks.7,8 However, patients often do not tolerate these braces well while sleeping, especially in cases in which there is bilateral involvement.
NSAIDs are prescribed frequently for plantar fasciitis. Although they are ef-fective as a pain medication, they do little to accelerate recovery from plantar fasciitis.9 Pathology studies of surgical specimens show degeneration, fragmentation, and revascularization but little evidence of acute or long-term inflammatory changes.10
Corticosteroid injections are effective for relieving acute pain in patients with plantar fasciitis. Corticosteroids work by modulating the production of inflammatory and anti-inflammatory proteins within the cell. The long-term effect of these injections on plantar fascia is less well understood, and no or incomplete relief often is seen several days or weeks after the procedure. The injections are associated with rupture of the plantar fascia and atrophy of the fat pad of the heel and, thus, should be used judiciously.
Rocker-soled shoes reduce pressure on the forefoot and often help reduce plantar fascial pain. However, this comes at the expense of increased ankle motion, shoe weight, and instability. Arch supports are another effective method of treatment, but no clear increase in satisfaction is demonstrated with custom arch supports compared with less expensive prefabricated inserts. Whether these types of footwear changes are helpful preventive measures in otherwise healthy feet is uncertain.
Surgery
Surgical release of the plantar fascia is indicated for severe plantar fascial pain after prolonged attempts at nonoperative treatment have been made. Usually, a portion (one-third to one-half) of the fascia is cut. The American Orthopedic Foot and Ankle Society and the American College of Foot and Ankle Surgeons have recommended 6 months of nonoperative management before this step is considered. The connective tissue may be released endoscopically (using a fiberoptic scope) or through an open approach. The ultimate results are comparable. In patients who have undergone excessive (more than 50%) fasciotomy, results have been poor.11 The progressive loss of the windlass effect may lead to a risk of midfoot pain and stress fractures in these patients.
Investigational Treatments
Many intriguing new approaches to treatment-resistant plantar fasciitis are under investigation. Although their effectiveness is questionable, many physicians are incorporating them into their practices. Because traditional treatment is time-tested and cost-efficient, evidence of clear superiority of these newer techniques is necessary before they should be accepted as mainstream treatments.
The machine used for managing musculoskeletal disorders with extracorporeal shock wave therapy (ESWT)-the application of high-intensity pulses of ultrasonic energy-was modified from designs that were used successfully to break up kidney stones. The FDA approved ESWT in 2000 for the treatment of patients with plantar fasciitis who did not improve with conservative therapy. The initial results of controlled studies indicated that such treatment is moderately effective and has few adverse effects, although it did require general or local anesthesia.
A later, well-publicized study disputed the findings of a beneficial effect with this treatment.12 Criticism of this report included patient selection (many of the subjects had pain for a brief period) and the low-energy technique used. Many well-controlled, blinded, randomized studies have since reported encouraging results.13-17 The results achieved with this procedure probably vary greatly with the device used and the amount of energy delivered. Interest in this treatment seems to be waning.
Botulism toxin injection has been used frequently for cosmetic purposes and in the management of neuromuscular disorders. Such injection also has been used off-label for musculoskeletal disorders, including lateral epicondylitis, low back pain, and plantar fasciitis. Injection into the plantar fascia has been shown to provide significant pain relief.18 Whether the mechanism of the pain relief involves paralysis of the irritated intrinsic muscles near the heel or a direct analgesic effect is not clear. Because the studies evaluating botulism toxin injection have been small and uncontrolled, endorsement awaits validation from larger, higher-quality investigations.
The use of autograft whole-blood injections has fallen out of favor, but currently there is considerable interest in the use of platelet-rich plasma (PRP) in the management of a wide variety of musculoskeletal complaints. This preparation is separated from whole blood after it has been centrifuged. The buffy coat layer, which contains the platelets, is isolated from the serum and red blood cells. However, there have been no good published studies to support the use of PRP.
Despite the lack of clear proven indications for PRP, its use in the community seems to be increasing. Some of the demand may be fueled by reports of high-profile athletes with various musculoskeletal injuries having received successful treatment with PRP. This treatment can be quite expensive and often is not covered by insurances. Although no published studies are available in peer-reviewed journals supporting the use of PRP in plantar fasciitis, one placebo-controlled study showed no significant effect in patients with Achilles tendinopathy.19
With radiofrequency microtenotomy-the perforation of tissue with a radiofrequency probe during surgical, percutaneous, or endoscopic exposure-the mechanical disruption is less than that with the use of plantar fasciotomy. This may reduce the possibility of midfoot pain, or “lateral column syndrome,” which complicates plantar fasciotomy postoperatively. Although radiofrequency microtenotomy has been available on the market for more than 10 years, the literature currently evaluating it consists of only small case series. Studies comparing the results of this procedure with those of more conventional surgical fasciotomy procedures are necessary before it can be recommended as an alternative. None are currently available.
LARGE, WELL-CONTROLLED TRIALS NEEDED
Although plantar fasciitis may lead to considerable and prolonged pain in a few cases, it often improves spontaneously. Therefore, large, well-controlled trials are necessary before new therapies should be adopted as standard practice. Although many promising treatments for plantar fasciitis are on the horizon, widespread use of these modalities should be reserved to controlled clinical trials until their usefulness is proved definitively.
References:
REFERENCES
1. Huang CK, Kitaoka HB, An KN, Chao EY. Biomechanical evaluation of longitudinal arch stability. Foot Ankle. 1993;14:353-357.
2. Hicks JH. The mechanics of the foot, part II: the plantar aponeurosis and the arch. J Anat. 1954;88:25-30.
3. Fiolkowski P, Brunt D, Bishop M, et al. Intrinsic pedal musculature support of the medial longitudinal arch: an electromyography study. J Foot Ankle Surg. 2003;42:327-333.
4. Levy JC, Mizel MS, Clifford PD, Temple HT. Value of radiographs in the initial evaluation of nontraumatic adult heel pain. Foot Ankle Int. 2006;27:427-430.
5. Harvey CK. Fibromyalgia, part II: prevalence in the podiatric patient population. J Am Podiatr Med Assoc. 1993;83:416-417.
6. Gill LH, Kiebzak GM. Outcome of nonsurgical treatment for plantar fasciitis [published correction appears in Foot Ankle Int. 1996;17:722.] Foot Ankle Int. 1996;17:527-532.
7. Probe RA, Baca M, Adams R, Preece C. Night splint treatment for plantar fasciitis: a prospective randomized study. Clin Orthop Relat Res. 1999;368:190-195.
8. Powell M, Post WR, Keener J, Wearden S. Effective treatment of chronic plantar fasciitis with dorsiflexion night splints: a crossover prospective randomized outcome study. Foot Ankle Int. 1998;19:10-18.
9. Donley BG, Moore T, Sferra J, et al. The efficacy of oral nonsteroidal anti-inflammatory medication (NSAID) in the treatment of plantar fasciitis: a randomized, prospective, placebo-controlled study. Foot Ankle Int. 2007;28:20-23.
10. Lemont H, Ammirati KM, Usen N. Plantar fasciitis: a degenerative process (fasciosis) without inflammation. J Am Podiatr Med Assoc. 2003;93:234-237.
11. Brugh AM, Fallat LM, Savoy-Moore RT. Lateral column symptomatology following plantar fascial release: a prospective study. J Foot Ankle Surg. 2002;41:365-371.
12. Buchbinder R, Ptasznik R, Gordon J, et al. Ultrasound-guided extracorporeal shock wave therapy for plantar fasciitis: a randomized controlled trial. JAMA. 2002;288:1364-1372.
13. Metzner G, Dohnalek C, Aigner E. High-energy Extracorporeal Shock-Wave Therapy (ESWT) for the treatment of chronic plantar fasciitis. Foot Ankle Int. 2010;31:790-796.
14. Ibrahim MI, Donatelli RA, Schmitz C, et al. Chronic plantar fasciitis treated with two sessions of radial extracorporeal shock wave therapy. Foot Ankle Int. 2010;31:391-397.
15. Dogramaci Y, Kalaci A, Emir A, et al. Intracorporeal pneumatic shock application for the treatment of chronic plantar fasciitis: a randomized, double blind prospective clinical trial. Arch Orthop Trauma Surg. 2010;130:541-546.
16. Gerdesmeyer L, Frey C, Vester J, et al. Radial extracorporeal shock wave therapy is safe and effective in the treatment of chronic recalcitrant plantar fasciitis: results of a confirmatory randomized placebo-controlled multicenter study. Am J Sports Med. 2008;36:2100-2109.
17. Kudo P, Dainty K, Clarfield M, et al. Randomized, placebo-controlled, double-blind clinical trial evaluating the treatment of plantar fasciitis with an extracoporeal shockwave therapy (ESWT) device: a North American confirmatory study. J Orthop Res. 2006;24:115-123.
18. Huang YC, Wei SH, Wang HK, Lieu FK. Ultrasonographic guided botulinum toxin type A treatment for plantar fasciitis: an outcome-based investigation for treating pain and gait changes. J Rehabil Med. 2010;42:136-140.
19. de Jonge S, de Vos RJ, Weir A, et al. One-year follow-up of platelet-rich plasma treatment in chronic Achilles tendinopathy: a double-blind randomized placebo-controlled trial. Am J Sports Med. 2011;39:1623-1629.
RECOMMENDED READINGS
• League AC. Current concepts review: plantar fasciitis. Foot Ankle Int. 2008;29:358-366. This article provides an exhaustive review of all aspects of the treatment for patients with plantar fasciitis.
• Neufeld SK, Cerrato R. Plantar fasciitis: evaluation and treatment. J Am Acad Orthop Surg. 2008;16:338-346. This is a comprehensive review of the current literature and recommended plantar fasciitis treatments.
• Paoloni J, De Vos RJ, Hamilton B, et al. Platelet-rich plasma treatment for ligament and tendon injuries. Clin J Sport Med. 2011;21:37-45. A review of the literature on platelet-rich plasma (PRP) shows that there have been no high-quality studies about treatment and there is limited evidence to support the use of injections with PRP in the management of chronic tendinopathy.
• Rompe JD, Furia J, Weil L, Maffulli N. Shock wave therapy for chronic plantar fasciopathy. Br Med Bull. 2007;81-82:183-208. This review of shock wave therapy for plantar fasciitis notes a preponderance of well-designed studies showing favorable results and concludes that such therapy should be considered for plantar fasciopathy only after more common, accepted, and proven noninvasive treatments have not been successful.