Managing Foot and Ankle Injuries in Athletes
Physicians who treat athletes with traumatic foot and ankle injuries should know when to order special imaging studies, determine whether injuries can be managed in the office or require referral, and return the athlete to sports activity quickly. For simple ankle sprains, plain x-ray films usually are not indicated; functional rehabilitation is a first-line treatment.
Traumatic injuries of the foot and ankle occur frequently in sports activity. In a review of injuries seen in a multispecialty sports clinic, 25% of 12,681 injuries that occurred in the 19 sports cited as most popular involved the foot and ankle.1 In addition, an estimated 20% to 35% of total time lost to injury in running and jumping sports can be attributed to ankle injuries.2
Physicians who treat athletes with traumatic injuries of the foot and ankle should keep in mind the following key points:
• Proper evaluation is important. Knowledge of when to order special imaging studies, such as stress x-ray films or MRI, should be incorporated into the diagnostic armamentarium.
• Cognizance of the more serious diagnoses is especially important. Determining which problems can be managed in the office and which ones require immediate referral to an orthopedic surgeon for operative management is prudent. Early treatment makes a crucial difference in the chances for success in surgery for acute fractures and ligament tears.
• Reviewing some of the less common problems, such as a navicular stress fracture or a Lisfranc sprain, is beneficial; if they are missed, significant disability may result.
• Treating athletes is more difficult than treating persons in the general population-the special challenge is to return the athlete to sports activity quickly without risking disability.
In this article, we review current diagnostic and management algorithms for the more common sports-related traumatic injuries of the foot and ankle. These include lateral ankle sprains; syndesmotic sprains; midfoot sprains; fifth metatarsal fractures; and stress fractures of the fibula, calcaneus, and navicular.
ANKLE SPRAINSDiagnosis
These are the most common foot and ankle injuries seen in athletes. Studies in Scandinavia have shown that ankle sprains account for up to 21% of sports-related injuries.3 The mechanism usually
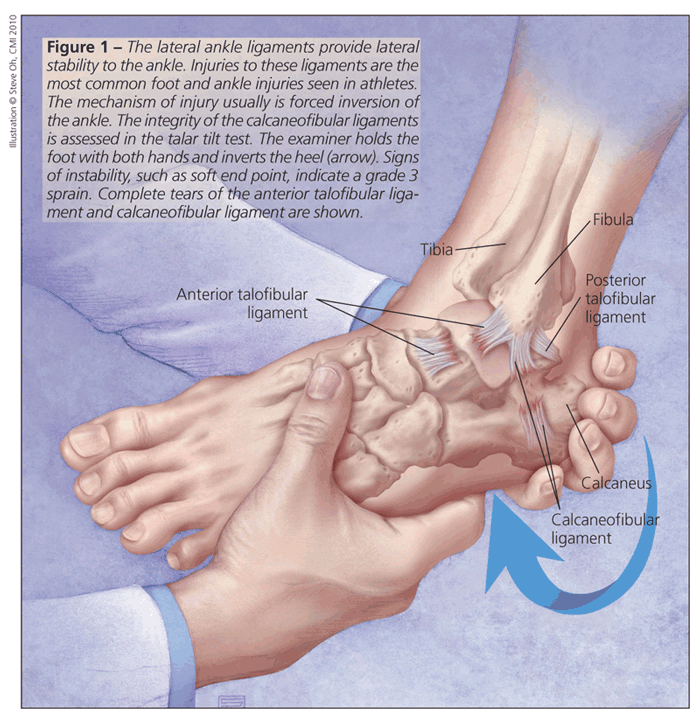
is forced inversion of the ankle, which tears 1 or more of the lateral ankle ligaments. These ligaments, which provide lateral stability to the ankle, are the anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (Figure 1).
Injuries can be classified in 3 grades. Grade 1 sprains involve a stretch or tear of the ATFL with no instability of the joint, grade 2 sprains consist of a compete tear of the ATFL with a partial or complete tear of the CFL, and grade 3 sprains include complete tears of both the ATFL and the CFL.4
Initial evaluation consists of a physical examination, which should include palpation over the fibular origin of the ATFL and the calcaneal insertion of the CFL. Swelling anterior or inferior to the malleolus should be differentiated from supramalleolar swelling, which may indicate fracture or syndesmotic injury.
Patient assessment includes the anterior drawer test, which involves subluxation of the talus anterior to the tibia with the knee bent and the ankle plantarflexed. This test is used to measure anterior translation to judge the integrity of the ATFL (normal value, 2 to 9 mm).
The talar tilt test specifically examines the integrity of the CFL (see Figure 1). The examiner inverts the heel and checks for signs of instability, such as a soft end point. A positive talar tilt test result indicates a grade 3 sprain. This test is best performed under fluoroscopy with comparison to the contralateral side.
For simple sprains, plain x-ray films are frequently obtained but usually not indicated. The Ottawa Ankle Rules were developed to identify patients who require x-ray films in the acute setting. According to the rules, if a patient demonstrates tenderness at the tip of either malleolus, the inability to walk 4 steps, or pain at the base of the fifth metatarsal, then appropriate foot and ankle x-ray films should be ordered.
Stress radiographs and MRI scans usually are not needed in the acute setting, but they may help in the diagnosis of chronic ankle pain. We recommend MRI for acute injuries with medial ecchymosis and chronic sprains that are still symptomatic 4 months after injury. MRI is also helpful in the diagnosis of injuries or conditions that may mimic ankle sprains, such as syndesmotic ligament tears, osteochondral lesions of the talus, occult stress fractures, synovitis, adhesions, intra-articular loose bodies, chronic instability, anterolateral impingement, and peroneal tendon pathology.
Treatment
Functional rehabilitation is our first-line treatment for a patient with a simple ankle sprain. Treatment modalities such as long-term immobilization and surgical management have resulted in slower return to activity, higher cost, and more complications without better effectiveness.3
Our initial management includes RICE (Rest, Ice, Compression, and Elevation) and anti-inflammatories for pain control; use of crutches for grade 1 and 2 injuries is discouraged. A short period of immobilization and protective bracing is implemented next. Then early, active range of motion; proprioceptive training; peroneal strengthening; and sport-specific exercises are started. The athlete may return to sports activity after the pain has resolved and ankle strength is equal to that of the opposite side.
At Duke University Medical Center, the majority of grade 1 sprains are diagnosed and managed by trainers; referrals to orthopedists for these injuries are rare. Return to activity usually occurs after 3 to 5 days for grade 1 sprains and after 1 to 3 weeks for grade 2 sprains; it takes longer for grade 3 sprains, and ankle protection may be required for up to 6 months.
Referral to an orthopedic surgeon is indicated in the acute phase for injuries with severe laxity, fractured bone, or medial ecchymosis. In 10% to 20% of athletes, initial treatment is unsuccessful and orthopedic referral should be considered. Surgical procedures for chronic instability, such as the Brostrom-Gould repair, have had excellent results.5
SYNDESMOTIC INJURIESDiagnosis
There are several differences between simple lateral ankle sprains and distal syndesmotic, or high ankle, sprains. Syndesmotic injuries are less common and more easily misdiagnosed, and patients take much longer to return to sports activity.
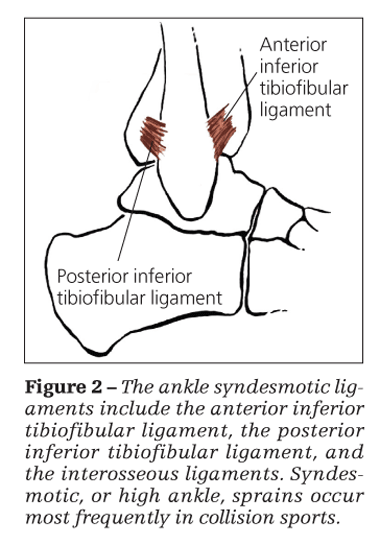
The ligaments that make up the distal syndesmosis are the anterior inferior tibiofibular ligament, the posterior inferior tibiofibular ligament, and the interosseous ligaments (Figure 2). Syndesmotic injuries occur most frequently in collision sports.6 The exact mechanism is not known and has not yet been reproduced in any cadaveric study. These injuries are referred to as high ankle sprains because the ligament damage is above, or higher than, the true ankle joint.
On physical examination, swelling may be present proximal to the lateral malleolus. Results of the talar tilt and anterior drawer tests are normal.
The squeeze test is performed by applying pressure in the patient’s midcalf to compress the fibula and tibia together; in an abnormal test result, ankle pain at the syndesmosis is elicited. The external rotation test is performed by externally rotating the foot with the knee held at 90° of flexion; in an abnormal test result, pain is elicited in the distal syndesmosis.
If a syndesmotic injury is suspected, we recommend ordering anteroposterior (AP), mortise, and lateral ankle x-ray views, as well as an external rotation stress view. MRI also can help in making this diagnosis.
Treatment
Syndesmotic injuries may be divided into 3 types. Type 1 injuries involve signs of syndesmotic sprain with normal x-ray findings. They may be managed with functional rehabilitation similar to the protocol used for simple sprains.
A type 2 injury is demonstrated by a tibiofibular clear space greater than 6 mm measured 1 mm above the joint seen in a stress x-ray view. Treatment consists of non–weight bearing in a short leg cast for 4 weeks followed by weight bearing in an immobilization boot for 4 more weeks.
Diagnosis of a type 3 injury is made by frank diastasis on the nonstress radiographs; immediate referral to an orthopedic surgeon for surgical stabilization is required. Return to play for type 1 and 2 injuries averages 8 to 12 weeks-twice as long as with a severe lateral ankle sprain.7,8
MIDFOOT SPRAINSDiagnosis
Midfoot, or Lisfranc, sprains usually are caused by a sudden rotation of a planted foot or an axial load on a plantarflexed foot. The classic mechanism involves a football player whose foot is planted with the toes extended and ankle plantarflexed. Another player falls and places an axial load directly on the heel.
Strong ligaments connect the second through fifth metatarsal bases (Figure 3). Because the base of the second metatarsal is recessed in relation to the first, no ligament connects these metatarsal
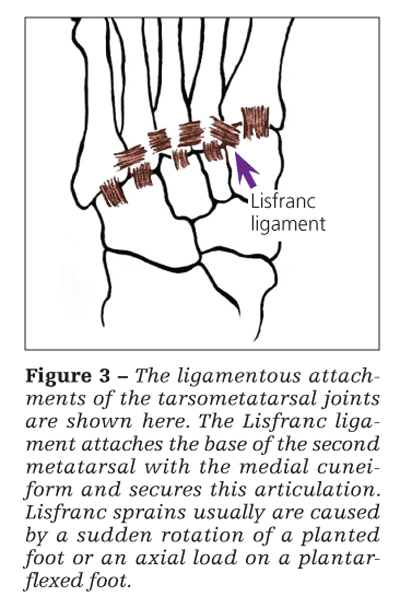
bases. The Lisfranc ligament attaches the base of the second metatarsal with the medial cuneiform and secures this articulation, which acts as the keystone to the tarsometatarsal joint complex. A high index of suspicion is needed because this diagnosis of ligament injury may be subtle in athletes.
On physical examination, the patient may exhibit mild swelling, pain with weight bearing, and an inability to perform a single heel rise or to run. Look for tenderness along the metatarsal bases, especially between the first and second bases. Severe subluxation or dislocation of the joint may manifest as a midtarsal prominence on the dorsum of the foot. Passive motion of the joint in any direction, including side-to-side compression of the midfoot, may elicit pain.
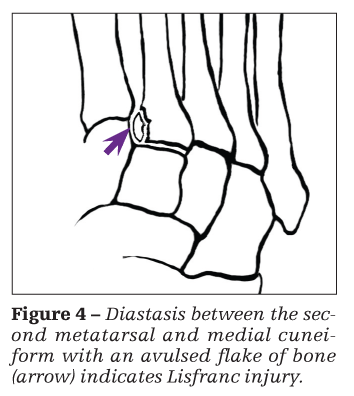
AP, lateral, and oblique weight-bearing x-ray views of the foot should be obtained for any athlete who has midfoot pain. Stress views are accomplished by weight bearing or passive abduction of the forefoot relative to the midfoot. Look for an avulsed flake of bone at the base of the second metatarsal or diastasis between the medial cuneiform and the second metatarsal (Figure 4). In addition, look for compression fractures of the cuboid and cuneiforms, which may also accompany this injury.
Bone scanning may yield a diagnosis of the joints involved; we have found this to be very helpful.9 MRI rarely is needed and is indicated only for equivocal injuries.
Treatment
Sprains that have no diastasis on plain or stress x-ray films may be managed with anti-inflammatories and RICE. We recommend non–weight bearing for 4 to 6 weeks followed by progressive weight bearing in a short leg walking cast for 4 to 6 more weeks. However, we strongly recommend referring all patients with Lisfranc sprains to an orthopedic surgeon. An examination conducted under anesthesia may be needed to make the diagnosis, especially to accurately determine unstable injuries.
Sprains that involve diastasis on either plain or stress x-ray views require immediate surgical evaluation. Unstable injuries may progress to partial or total dislocation of the entire tarsometatarsal joint complex. Return to play is much longer than that with a simple ankle sprain (possibly 4 to 6 months). Upon return to play, we recommend that the athlete wear stiff-soled shoes with an orthosis. The athlete should be counseled that even after adequate treatment, low-grade midfoot pain may persist for years.
BASE OF THE FIFTH
METATARSAL FRACTURESDiagnosis and treatment
The Jones fracture is the most well-known proximal fifth metatarsal fracture, but avulsion fractures and diaphyseal stress fractures also should be recognized. In the physical examination, palpation elicits tenderness at the proximal fifth metatarsal. AP, oblique, and lateral x-ray views of the foot should be ordered.
In avulsion injuries, the fracture fragment is connected to the lateral plantar aponeurosis and usually is detached by a strong inversion force. Most of these fractures are nondisplaced; they may be managed symptomatically with weight bearing in stiff-soled shoes for 3 to 4 weeks. The fracture usually heals predictably with no residual disability.
A true Jones fracture occurs at the metaphyseal-diaphyseal junction (Figure 5); it usually is attributed to lateral tensile stresses from forced forefoot adduction. Often, the fracture is located 1.5
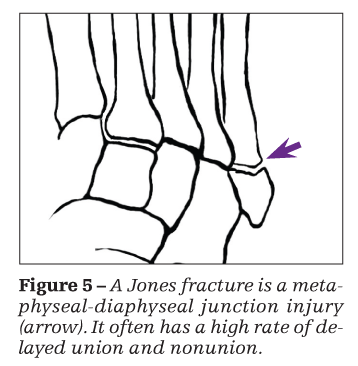
to 2 cm distal to the base and has a high rate of delayed union and nonunion, presumably because of compromised vasculature in this region.10
A recreational athlete who has a nondisplaced fracture may be treated with non–weight bearing in a short leg cast until there are clinical signs of healing, usually after 6 to 8 weeks. However, he or she must be informed that nonsurgical treatment results in a longer period before return to play because of multiple factors, which include a delayed union rate of between 25% and 66%, a nonunion rate of between 7% and 28%,11 a long-term refracture rate of 33%,12 and a longer interval of disuse atrophy.
Referral to an orthopedist for surgery is recommended for any athlete who has a Jones fracture. After the fracture has healed, we recommend that athletes wear a protective orthosis.
The third type of fifth metatarsal base fracture, a diaphyseal stress fracture, usually is associated with prodromal pain for several weeks before there is radiographic evidence of injury. However, MRI may reveal this injury before there is radiographic evidence.
Diaphyseal stress fractures respond poorly to conservative management. Referral to an orthopedist for surgical stabilization is recommended. Distal fractures of the fifth metatarsal do occur in athletes but usually are nondisplaced and rarely require surgical care.
STRESS FRACTURESDiagnosis
These overuse injuries often are seen in athletes who perform high-repetition, low-impact activities, such as running. The fractures occur when normal bone is subjected to a summation of subthreshold forces and the natural reparative response has been overloaded. Causative factors that should be considered include unequal leg lengths, varus knees, abnormal lower extremity alignment, cavus or planus foot deformities, poorly cushioned shoes, hard running surfaces and, in female athletes, hormonal imbalance.
Physical examination may reveal swelling and tenderness over the bone, as well as an antalgic gait. Plain x-ray films should be ordered of the foot or ankle, depending on the area of suspicion. X-ray film results may be normal for 3 to 4 weeks after symptoms begin. If early confirmation is needed, bone scanning and MRI results usually are abnormal in the first 1 to 2 days of symptoms.
Navicular stress fractures are more common than once thought, although the incidence probably still is less than 1% of stress fractures of the lower extremity. Patients complain of pain in the
dorsum of the midfoot or in the medial arch.
On examination, pain in the navicular usually is elicited if the patient stands on his tiptoes. In addition to plain radiography, we recommend CT scanning because the amount of fracture displacement can be measured correctly and a bipartite navicular can be ruled out.
Treatment
For nondisplaced navicular fractures with minimal comminution, we recommend non–weight bearing in a short leg cast for 6 weeks. A CT scan may confirm healing, and the athlete usually

returns to play 6 to 12 weeks after cast removal.
Displaced or comminuted fractures require surgical fixation. However, we recommend that all patients with navicular stress fractures be referred to an orthopedic surgeon for surgical evaluation. After return to play, it is recommended that the athlete wear a semirigid longitudinal arch support in his athletic shoes.
Stress fractures of the distal fibula, calcaneus, and second to fifth metatarsal shafts usually are managed nonoperatively. A reduction in activity level allows most of these fractures to heal reliably; cast immobilization usually is not necessary.
Patients with metatarsal stress fractures should wear stiff-soled shoes until symptoms resolve, usually after 4 to 6 weeks. A soft heel cushion is recommended for calcaneal stress fractures until resolution, usually 6 to 8 weeks. With conservative treatment, fibular stress fractures frequently resolve in 4 to 6 weeks. For an athlete who has severe symptoms or is noncompliant, we recommend weight bearing in a short leg walking cast until symptoms resolve.
At this point, the athlete may make the transition to a stirrup brace.
References:
References
1. Garrick JG. The frequency of injury, mechanism of injury, and epidemiology of ankle sprains. Am J Sports Med. 1977;5:241-242.
2. Mack RP. Ankle injuries in athletics. Clin Sports Med. 1982;1:71-84.
3. Kannus P, Renström P. Treatment for acute tears of the lateral ligaments of the ankle: operation, cast, or early controlled mobilization. J Bone Joint Surg. 1991;73A:305-312.
4. Baxter DE. Traumatic injuries to the soft tissues of the foot and ankle. In: Mann RA, ed. Surgery of the Foot. 5th ed. St Louis: Mosby; 1986:456-472.
5. Keller M, Grossman J, Caron M, Mendicino RW. Lateral ankle instability and the Brostrom-Gould procedure. J Foot Ankle Surg. 1996;35:513-520.
6. Gerber JP, Williams GN, Scoville CR, et al. Persistent disability associated with ankle sprains: a prospective examination of an athletic population. Foot Ankle Int. 1998;19:653-660.
7. Arendt E, ed. Ankle soft tissue injuries. In: Orthopaedic Knowledge Update: Sports Medicine 2. Rosemont, IL: American Academy of Orthopaedic Surgeons; 1999:373-377.
8. Hopkinson WJ, St Pierre P, Ryan JB, Wheeler JH. Syndesmosis sprains of the ankle. Foot Ankle. 1990;10:325-330.
9. Nunley JA, Vertullo CJ. Classification, investigation, and management of midfoot sprains: Lisfranc injuries in the athlete. Am J Sports Med. 2002;30:871-878.
10. Smith JW, Arnoczky SP, Hersh A. The interosseous blood supply of the fifth metatarsal: implications for proximal fracture healing. Foot Ankle. 1992;13:143-152.
11. Title CI, Katchis SD. Traumatic foot and ankle injuries in the athlete. Orthop Clin North Am. 2002;33:587-598.
12. Quill GE Jr. Fractures of the proximal fifth metatarsal. Orthop Clin North Am. 1995;26:353-361.