Paget Disease Presenting as a Chronic Symmetrical Polyarthritis
J.S. is a 69-year-old woman who presented with bilateral knee pain that she had had for 5 years.
ABSTRACT:This patient's symptoms were attributed to osteoarthritis initially and then to rheumatoid arthritis. She had a history of asymptomatic Paget disease of bone. Physical examination revealed tenderness, swelling, and crepitation in both knees. Chondrocalcinosis was seen on pelvic, knee, and hand x-ray films; the sacroiliac joints were normal. This is typical of calcium pyrophosphate dihydrate (CPPD) crystal deposition disease. Because it was thought that Paget disease of bone played a role in CPPD disease development, treatment was aimed at both conditions. With this regimen, the symptoms resolved. It may be hypothesized that Paget disease played a role in the development of CPPD disease in this patient and management of Paget disease may lead to control of the associated CPPD disease symptoms.
J.S. is a 69-year-old woman who presented with bilateral knee pain that she had had for 5 years. Her symptoms had been attributed to osteoarthritis (OA) initially and then to rheumatoid arthritis (RA). She had a history of asymptomatic Paget disease of bone for which she was not being treated. Chondrocalcinosis was seen on pelvic, knee, and hand x-ray films, and her sacroiliac joints were normal, typical of calcium pyrophosphate dihydrate (CPPD) crystal deposition disease. Paget disease of bone was thought to have played a role in CPPD disease development in this patient; therefore, treatment was aimed at both conditions. In this article, we discuss the hypothesis that in some patients, management of Paget disease may help control symptoms of associated CPPD disease.
Case Report
J.S. described her bilateral knee pain as a severe dull pain that did not worsen at any time during the day. The pain was associated with morning stiffness and swelling and caused impairment in her performance of activities of daily living. She reported good pain relief with NSAIDs and intra-articular corticosteroid knee injections.
The patient's initial diagnosis of OA was changed to RA 1 year ago after her rheumatoid factor was found to be positive (titer, 1:2). At the time of presentation, she was not receiving disease-modifying antirheumatic drugs but occasionally was using ibuprofen for relief of her knee pain.
The diagnosis of Paget disease of bone had been made incidentally 10 years earlier, when J.S. underwent a head CT scan for another reason. A nuclear bone scan showed focal uptake in the skull, T8 and L5 vertebrae, and sacrum. J.S. was not offered treatment for Paget disease at the time of diagnosis because she was asymptomatic.
Our physical examination of J.S. revealed tenderness, swelling, and crepitation in both knees. There was no warmth or erythema of the knees, and range of motion and muscle strength were normal. Rash and hepatosplenomegaly were absent.
Laboratory test results were normal for thyroid function and negative for hepatitis B and C. Also normal were uric acid; parathyroid hormone; antinuclear, anti-dsDNA, and Lyme antibody; and complement levels. Serum alkaline phosphatase levels were elevated, with a value of 132 U/L (normal, 35 to 104 U/L). The bone-specific alkaline phosphatase level was elevated at 23.7 U/L (normal, 0 to 21.3 U/L).
FIGURE 1
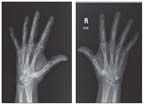
X-ray films of both of the patient's hands show chondrocalcinosis of the triangular fibrocartilage.
X-ray films of the patient's pelvis, sacroiliac joints, knees, feet, and hands were obtained. The pelvic x-ray film showed chondrocalcinosis in both hip joints and the pubis symphysis. The sacroiliac joints were normal. In the knee joints, there was severe chondrocalcinosis bilaterally involving the articular fibrocartilage. X-ray films of the patient's hands showed chondrocalcinosis of the triangular fibrocartilage (Figure 1). These radiographic findings were typical of CPPD disease.
FIGURE 2
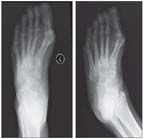
Shown are calcifications in the left midfoot dorsally that were aspirated using ultrasonographic guidance.
No evidence of RA was seen with ultrasonographic examination of the patient's hands and feet. Granular material was seen in the left midfoot (Figure 2). This material was aspirated; positively birefringent, rhomboid, needle-shaped crystals revealed with examination of the aspirate under the microscope were in keeping with a diagnosis of CPPD disease.
Therapy with colchicine, 0.6 mg bid, was started; it was tolerated but without any clinical response. The dosage was lowered to once daily after a few days because the patient had diarrhea, and therapy was stopped 6 weeks later because of a lack of efficacy. Two weeks after the start of therapy with colchicine, therapy with a bisphosphonate, risedronate, 30 mg/d for 2 months, was started to manage the Paget disease and attempt to stop the progression and pain associated with the CPPD disease. There was significant improvement in pain and swelling of the knees and feet within the first few weeks. After 2 months, the dosage was increased to 35 mg/wk for 4 weeks. Therapy with risedronate was stopped because the patient lacked insurance and could not afford it and she felt much better. She remained asymptomatic 3 months later. J.S. experienced great pain relief with this treatment regimen and had no more knee swelling.
Discussion
CPPD disease occurs when CPPD crystals are deposited in articular and periarticular tissue. Chondrocalcinosis, a pathological and radiological term, describes the deposition of these crystals within cartilage. Pseudogout describes a severe acute attack that resembles an exacerbation of gout.1
Although CPPD disease is an idiopathic process, metabolic diseases have been linked to it etiologically (eg, hyperparathyroidism, hemochromatosis, hypomagnesemia, and hypophosphatemia).2 In addition, 3.4% of patients with CPPD disease have been reported to also have Paget disease.3 Whether this association is a product of chance or Paget disease has a true role in the manifestation of CPPD disease is unclear.
Paget disease of bone occurs when there is increased bone turnover on focal areas of the skeleton.4 In a 1980 review of 290 cases, Altman5 found that 83% of patients with this condition had 1 or more rheumatologic disorders; the most common was back pain caused by OA.
Radi and associates6 described an unusual frequency of 42% of cases of chondrocalcinosis in Paget disease in 1970. Doury and colleagues7 and Boussina and coworkers8 reexamined the relationship between Paget disease and chondrocalcinosis in 1975 and 1976, respectively, both concluding that it is a matter of chance. However, the incidences of chondrocalcinosis in Paget disease found in the Doury and Boussina studies were markedly different, 1.9% and 13.6%, respectively. Because variation in the reported incidence of chondrocalcinosis in Paget disease is wide, further work clearly is needed to examine this relationship.
We speculated that J.S.'s Paget disease played a role in the development of her CPPD disease. Therefore, bisphosphonate therapy was started to manage the Paget disease even though it was asymptomatic.9 Seeing J.S. remain pain-free after bisphosphonate therapy was started provided evidence that Paget disease and CPPD disease may be related etiologically.
The decision to manage J.S.'s Paget disease was made after other potential causes of CPPD disease, such as hypomagnesemia, hyperparathyroidism, and hemochromatosis, were excluded. In 1992, Jones and associates10 examined individual case reports of those 3 diseases in CPPD disease to determine whether managing them leads to improvement in the CPPD disease.
The 3 diseases have a significant association with CPPD disease. In patients who have both hypomagnesemia and CPPD disease, magnesium replacement leads to resolution of CPPD disease symptoms. However, management of hyperparathyroidism does not result in disease regression or symptom improvement in CPPD disease. In the single case study of hemochromatosis in CPPD disease, initial treatment resulted in symptom improvement of CPPD disease, but there was worsening of symptoms and disease progression 1 year later. It may be concluded from the case reports that managing the underlying etiological disease process helps or has no effect on the management of CPPD disease.
Because the effect of managing Paget disease on CPPD disease was unknown, we decided to treat J.S. with bisphosphonates. J.S. responded well to the management of CPPD disease, leading us to conclude that patients with Paget disease and CPPD disease may benefit from management of Paget disease, including asymptomatic Paget disease.
Conclusion
Analysis of J.S.'s case can lead one to hypothesize that Paget disease played an etiological role in the development of CPPD disease in this patient. Also, in some patients, management of Paget disease, even if asymptomatic, can lead to symptom control of the associated CPPD disease.
References:
REFERENCES
1. Bencardino JT, Hassankhani A. Calcium pyrophosphate dihydrate crystal deposition disease. Semin Musculoskelet Radiol. 2003;7:175-185.
2. Announ N, Guerne PA. Diagnosis and treatment of calcium pyrophosphate crystal-induced arthropathy [in German]. Z Rheumatol. 2007;66:573-574, 576-578.
3. Hamilton EB. Diseases associated with CPPD deposition disease. Arthritis Rheum. 1976;19(suppl 3):353-357.
4. Ralston SH, Langston AL, Reid IR. Pathogenesis and management of Paget's disease of bone. Lancet. 2008;372:155-163.
5. Altman RD. Musculoskeletal manifestations of Paget's disease of bone. Arthritis Rheum. 1980;23:1121-1127.
6. Radi I, Epiney J, Reiner M. Chondrocalcinosis and Paget's disease of bone [in French]. Rev Rhum Mal Osteoartic. 1970;37:385-388.
7. Doury P, Delahaye RP, Leguay G, et al. Diffuse articular chondrocalcinosis and Paget's disease [in French]. Rev Rhum Mal Osteoartic. 1975;42:551-554.
8. Boussina I, Gerster J, Epiney J, Fallet GH. A study of the incidence of articular chondrocalcinosis in Paget's disease of bone. Scand J Rheumatol. 1976;5:33-35.
9. Whyte MP. Clinical practice: Paget's disease of bone. N Engl J Med. 2006;355:593-600.
10. Jones AC, Chuck AJ, Arie EA, et al. Diseases associated with calcium pyrophosphate deposition disease. Semin Arthritis Rheum. 1992;22:188-202.