Recognizing and Managing Posterior Cruciate Ligament Injuries
Posterior cruciate ligament (PCL) injuries usually result from automobile or sports collisions. When is nonoperative treatment the best option?
ABSTRACT: Physicians may be unfamiliar with posterior cruciate ligament (PCL) injuries because the PCL is injured far less frequently than the anterior cruciate ligament and the injury may have a subtle presentation. Contact sport athletes and persons involved in motor vehicle collisions often are affected. PCL injuries frequently occur in conjunction with damage to other capsuloligamentous structures of the knee. A comprehensive examination of the injured extremity must include evaluation of these and neurovascular structures. PCL-specific examination maneuvers include the posterior drawer test, posterior sag test, and quadriceps active test. The primary evaluation should include plain radiographs and MRI. The available data encourage nonoperative management for most grade 1 and 2 injuries, but isolated acute grade 3 injuries may require surgery. (J Musculoskel Med. 2012;29:106-111)
Physicians often are familiar with the clinical presentation and management of collateral ligament and anterior cruciate ligament (ACL) strains or ruptures because these injuries occur somewhat frequently in active persons. They may be less familiar with injuries of the posterior cruciate ligament (PCL), an important stabilizer of the knee. The PCL is injured far less frequently, and when it is disrupted in isolation the injury may have a subtle presentation that can elude even the experienced examiner. In addition, patients who sustain isolated PCL injuries may continue to function at a competitive level, symptoms may not develop until long after the inciting event, and the natural history of the isolated PCL-deficient knee remains unclear.
Recent biomechanical investigations have demonstrated that the PCL makes a major contribution to knee function and have suggested that chronic posterior instability may result in premature arthrosis. Therefore, the examining physician needs to arrive at a timely and accurate diagnosis and can do so by recognizing the common injury mechanisms and presenting symptoms and initiating the appropriate workup.
Current treatment guidelines suggest that low-grade PCL injuries may be managed without surgery and that most patients return to their preinjury function level. However, substantial controversy surrounds what constitutes optimal management of patients who sustain high-grade isolated PCL injuries. There is a paucity of data demonstrating that surgical intervention significantly alters long-term objective or subjective outcomes in this patient cohort.
In this article, we focus on familiarizing treating physicians with the mechanisms typically associated with PCL injury and the clinical evaluation of patients in whom PCL insufficiency is suspected. We also provide a discussion of the most current treatment options and a relevant algorithm predicated on existing data about nonoperative and surgical interventions.
ANATOMY
The PCL originates from the lateral border of the medial femoral condyle (MFC) and inserts about 1 cm below the joint line in a midline depression between the posterior aspects of the medial and lateral tibial plateaus. The ligament consists of 2 functional bundles: the anterolateral fibers are larger in cross-sectional area and tighten in knee flexion and become lax in extension; the posteromedial fibers are smaller and become tight in knee extension and deep knee flexion. Together, the anterolateral and posteromedial bundles act as the primary restraint to posterior translation of the tibia; the collateral ligaments and the posterolateral structures act as secondary restraints. Of note, the PCL is a secondary restraint to abnormal external rotation of the tibia in the setting of injury to the posterolateral structures of the knee.1
AT-RISK POPULATIONS AND MECHANISM OF INJURY
Two distinct patient populations are affected by PCL injuries: contact athletes and persons subject to high-energy trauma. The mechanism of injury, magnitude of ligament disruption, and time to presentation may vary greatly between these cohorts.
The mechanism of PCL injury often seen in centers that care for a large number of patients with trauma is motor vehicle collisions. Patients may experience a classic dashboard injury in which the proximal tibia of the flexed knee is subject to a posterior-directed force during impact. More often, high-energy collisions impart combined forces to the lower leg, resulting in disruption of multiple structures that support the knee; these collisions may produce a dislocation. Patients usually are evaluated acutely; the treating physician should maintain an appropriately high index of suspicion for PCL injury in this setting.
Athletes who participate in contact sports (eg, football, soccer, and rugby) also are at risk for PCL injury. Unlike the risk of ACL injury, the risk of PCL injury is greater than that in persons involved in noncontact sports that primarily involve pivoting and cutting.2
The typical PCL injury mechanism in contact athletes is a fall on a flexed knee with the foot in plantar flexion, which results in the proximal tibia striking the ground first. A common mechanism in football is knee hyperflexion with the presence of a posterior-directed force on the anterior tibia, which may occur when an opponent attempts to tackle the ball carrier and strikes the leg during high knee flexion.3 Isolated hyperflexion or hyperextension of the knee also may result in PCL injury.
Many athletes with PCL insufficiency have few symptoms and do not recall the mechanism of injury or may describe a seemingly trivial inciting event. Therefore, isolated PCL injury may remain undiagnosed in the acute period and the clinician should attempt to elicit the injury mechanisms when obtaining the history surrounding a seemingly innocuous knee injury.
CLINICAL EVALUATION AND DIAGNOSIS
History
Obtaining a thorough history often helps the physician delineate the magnitude and acuity of the inciting event. Although PCL injuries may occur in isolation, injuries that occur in conjunction with damage to other capsuloligamentous structures of the knee are more common in the setting of high-energy trauma. Patients often complain of significant knee pain and swelling and seek medical attention immediately.
In contrast, the presenting symptoms of an isolated PCL injury may be subtle and vague. In the acute period, patients may complain of mild pain in the back of the knee; stiffness; or pain with deep knee flexion, including squatting or kneeling. Patients who present in the chronic phase may complain of anterior knee pain, difficulty with ascending or descending stairs, and pain with sprinting or deceleration.4 Patients may recollect a specific traumatic event or describe a gradual onset of symptoms that may hinder athletic activity.
Physical Examination
A comprehensive examination of the injured extremity, essential for accurate diagnosis of PCL injuries, must include evaluation of the knee’s other critical supporting structures. In the acute phase, patients may walk with a slight limp or avoid terminal extension of the knee. The medial and lateral collateral ligaments should be palpated for tenderness. Varus and valgus testing should be performed at 30° of flexion to evaluate collateral integrity and at full extension to evaluate posteromedial and posterolateral structure integrity.5 The menisci should be evaluated with select provocative maneuvers; the examiner also may palpate for focal chondral lesions along the condyles.
When assessing the ACL, the examiner should appreciate the resting posture of the medial tibial plateau (MTP); it should be about 1 cm anterior to the MFC in the uninjured knee at 90° of flexion. A comparison should be made with the contralateral limb; without it, an increase in anteroposterior laxity may be falsely attributed to ACL insufficiency rather than PCL insufficiency.3
TABLE 1

Physical examination maneuvers in the diagnosis of posterior cruciate ligament injury
Testing
Numerous PCL-specific examination maneuvers have been described; the posterior drawer test is considered the most sensitive and specific (Table 1). This test is performed with the patient’s hip flexed to 45°, knee flexed to 90°, and foot in a neutral position. The examiner sits on the patient’s foot and places both hands behind the patient’s proximal tibia; with the thumbs on the patient’s anterior tibial plateau, the examiner applies a posterior-directed force to the tibia.
The examiner assesses the position of the MTP relative to the MFC. One to 5 mm of posterior translation (MTP anterior to MFC) represents a grade 1 injury, 6 to 10 mm of posterior translation (MTP flush with MFC) represents a grade 2 injury, and more than 10 mm of posterior translation (MTP posterior to femoral condyles) represents a grade 3 injury. Translation of more than 10 mm often is indicative of combined ligamentous injury and mandates careful examination of the other capsuloligamentous structures of the knee.
Other frequently used PCL-specific examination maneuvers include the posterior sag test (Godfrey test) and the quadriceps active test. The posterior sag test is performed with the patient’s hip flexed to 45° and knee flexed to 90°, with the foot resting on the examination table. When the PCL is disrupted, the tibia may appear to sag posteriorly. The quadriceps active test is performed with the patient supine and the knee flexed to 90°. The examiner stabilizes the foot, and the patient is asked to push it down the table. Contraction of the quadriceps muscle in a PCL-deficient knee results in an anterior shift of the tibia. A translation of more than 2 mm is considered a positive result for PCL disruption.
A combined ligamentous injury, as suggested by more than 10 mm of posterior translation with the posterior drawer test, may include injury to the ACL or collateral ligaments and, frequently, the posterolateral corner complex. To help distinguish between isolated PCL injuries and injuries that involve the posterolateral corner, the examiner may use the tibial external rotation, or dial, test.
This test is performed with the patient in a prone position; an external rotation force is applied to both feet with the knee positioned at 30° and then 90° of flexion. A side-to-side difference of more than 10° is considered an abnormal test result. An increase of 10° or more of external rotation at 30° of knee flexion, but not at 90°, suggests an isolated posterolateral corner injury. Increased external rotation at both 30° and 90° of knee flexion suggests a combined PCL and posterolateral corner injury. In addition, the presence of a reverse pivot shift may be indicative of combined injury to the PCL and posterolateral corner.1 These results always should be compared with results from the contralateral limb because there is substantial variability of external rotation among patients.
Imaging
Plain radiography. If a PCL injury is suspected, the primary evaluation should include obtaining plain radiographs, such as standard weight-bearing anteroposterior radiographs at neutral and at 45° of flexion, as well as lateral and patellar views. These initial radiographs can provide a great deal of information, including the presence of arthritic changes, which are seen primarily in the patellofemoral and medial compartments of the chronically PCL-deficient knee.
Some authors have advocated the use of stress radiographs for evaluating PCL insufficiency. Posterior displacement in excess of 8 mm indicates complete insufficiency of the PCL; more than 10 mm of displacement has been associated with concomitant posterolateral corner injury.6
FIGURE 1
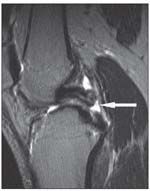
MRI. This modality can aid in the diagnosis of acute PCL injuries as well as help assess the integrity of other knee structures (Figure 1). In the acute setting, MRI has proved to be both highly sensitive and specific for making a diagnosis of PCL injury.7,8 However, chronic low-grade injuries may not be discernible via MRI; in some cases, the PCL-deficient knee may appear entirely normal on routine imaging. Therefore, the clinician must consider the collective data provided by the patient history, physical examination, and imaging modalities to arrive at a diagnosis for patients who present with a prolonged history of somewhat subtle symptoms of pain or instability.
MANAGEMENT
Nonoperative
The natural history of isolated PCL injury in regard to long-term objective and subjective outcomes remains unclear. Patients with acute isolated (grade 1 or 2) injury who have minimal complaints of instability or pain traditionally have been treated with physical therapy and observation. Most of these patients appear to return to their preinjury level of activity in the short term with little or no impairment in subjective knee function.9-13 However, long-term follow-up has yielded conflicting reports on overall outcome. Predicting which patients will have persistent instability and a poor result remains difficult.
Studies have shown that patellofemoral and medial compartment osteoarthritis evolve in many patients with isolated PCL injury and are associated with a corresponding deterioration in knee function.14,15 Conversely, in a prospective study of patients with isolated PCL injury, Shelbourne and Muthukaruppan12 demonstrated that subjective knee scores remain constant over time for the majority of patients. The authors noted that there was no correlation between subjective scores and grade of laxity or any identifiable factor that predicted a poorer outcome.
FIGURE 2
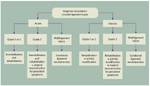
Operative
Although the available data encourage nonoperative management for most grade 1 and 2 injuries, isolated acute grade 3 injuries may require surgery (Figure 2). In addition, surgical intervention usually is required for chronic isolated grade 3 injuries that remain symptomatic despite conservative treatment and grade 3 PCL injuries that are combined with other knee ligament injuries.
Surgical techniques are evolving, and currently there is no consensus about the optimal one for PCL reconstruction. The most frequently used technique involves a single-bundle graft reconstruction placed in the femoral and tibial tunnels. Although this surgical technique has resulted in improvement in subjective function, objective improvements in knee laxity have been unsatisfactory.16,17
These poor results have prompted investigators to evaluate other methods of PCL reconstruction, including double-bundle techniques and approaches that avoid the use of a tibial drill tunnel by instead using a tibial inlay technique. Many surgeons have had reasonable results with these reconstructive approaches, and numerous laboratory studies have supported their biomechanical advantages.18-21 However, the small number of nonrandomized clinical comparisons that have attempted to evaluate these methods have not shown significant differences in the short-term subjective or objective outcomes for single- versus double-bundle femoral fixation methods or tibial inlay versus transtibial techniques of tibial fixation.
Further long-term randomized studies are warranted to evaluate these surgical methods and answer 2 pertinent questions. They are: (1) Does reconstructive surgery significantly alter the natural history of the PCL-deficient knee? and (2) Does one of the commonly used methods of PCL reconstruction provide a distinct clinical advantage over the others?
Recent in vivo kinematic data have suggested that although PCL reconstruction may improve rotational and anteroposterior translation, reconstruction does not restore mediolateral tibial translation or patellar tilt, changes that may influence the well-documented development of medial and patellofemoral compartment arthrosis in this setting.22 Recent systematic reviews have evaluated isolated PCL clinical outcomes and also have shown that patients will make a predictable return to recreational and athletic activity, although reconstruction does not restore normal stability, and it does not prevent degenerative osteoarthritis.23
TABLE 2

Nonoperative rehabilitation for patients with posterior cruciate ligament injury
Rehabilitation
The recommended treatment for patients with isolated PCL injuries is a rehabilitation regimen predicated on early immobilization of the knee and progressive strengthening of the quadriceps musculature (Table 2). In the initial phase of injury, 2 weeks of protected weight bearing is advocated, possibly with the knee immobilized in slight flexion. This position effectively limits posterior translation of the tibia and reduces strain on the anterolateral bundle of the PCL, allowing it to assume a physiological position.3 This regimen typically is followed with passive and active range of motion exercises of the knee as well as quadriceps strengthening exercises to counteract posterior tibial translation. Patients usually can expect to resume sports activity in 4 to 12 weeks postinjury.
Postoperative rehabilitation is focused on relieving graft tension until adequate healing has occurred.3 This is accomplished by bracing the knee in slight flexion for 3 or 4 weeks, allowing only partial weight bearing, and limiting flexion. Unopposed hamstring exercises should be avoided. Flexion is achieved initially with passive exercises and then quadriceps strengthening and proprioceptive training. Athletes usually may resume full activity 9 to 12 months after surgery.3
CONCLUSION
Well-designed clinical studies describing the long-term function of the PCL-deficient knee and the optimal mode of treatment are unavailable. The rehabilitation protocol should focus on a physical therapy program that encourages quadriceps strengthening to resist posterior translation of the tibia and allow for healing of the ligament at its functional length. Patients should be advised that for some isolated grade 3 PCL injuries and combined ligament injuries, how surgical reconstruction ultimately affects the long-term function of the knee remains uncertain. Future research will focus on identifying patients who are at risk for deterioration in knee function after PCL injury and defining the best methods for restoring function and stability to them through nonoperative or operative means.
References:
REFERENCES
1. Petrigliano FA, Suero EM, Lane CG, et al. Posterior cruciate ligament and posterolateral corner deficiency results in a reverse pivot shift. Clin Orthop Relat Res. 2011 Aug 27; [Epub ahead of print].
2. Schulz MS, Russe K, Weiler A, et al. Epidemiology of posterior cruciate ligament injuries. Arch Orthop Trauma Surg. 2003;123:186-191.
3. Margheritini F, Rihn J, Musahl V, et al. Posterior cruciate ligament injuries in the athlete: an anatomical, biomechanical and clinical review. Sports Med. 2002;32:393-408.
4. Petrigliano FA, McAllister DR. Isolated posterior cruciate ligament injuries of the knee. Sports Med Arthrosc. 2006;14:206-212.
5. Allen CR, Kaplan LD, Fluhme DJ, Harner CD. Posterior cruciate ligament injuries. Curr Opin Rheumatol. 2002;14:142-149.
6. Sekiya JK, Whiddon DR, Zehms CT, Miller MD. A clinically relevant assessment of posterior cruciate ligament and posterolateral corner injuries: evaluation of isolated and combined deficiency. J Bone Joint Surg. 2008;90A:1621-1627.
7. Gross ML, Grover JS, Bassett LW, et al. Magnetic resonance imaging of the posterior cruciate ligament: clinical use to improve diagnostic accuracy. Am J Sports Med. 1992;20:732-737.
8. Vaz CE, Camargo OP, Santana PJ, Valezi AC. Accuracy of magnetic resonance in identifying traumatic intraarticular knee lesions. Clinics (Sao Paulo). 2005;60:445-450.
9. Fowler PJ, Messieh SS. Isolated posterior cruciate ligament injuries in athletes. Am J Sports Med. 1987;15:553-557.
10. Parolie JM, Bergfeld JA. Long-term results of nonoperative treatment of isolated posterior cruciate ligament injuries in the athlete. Am J Sports Med. 1986;14:35-38.
11. Shelbourne KD, Davis TJ, Patel DV. The natural history of acute, isolated, nonoperatively treated posterior cruciate ligament injuries: a prospective study. Am J Sports Med. 1999;27:276-283.
12. Shelbourne KD, Muthukaruppan Y. Subjective results of nonoperatively treated, acute, isolated posterior cruciate ligament injuries. Arthroscopy. 2005;21:457-461.
13. Shino K, Horibe S, Nakata K, et al. Conservative treatment of isolated injuries to the posterior cruciate ligament in athletes. J Bone Joint Surg. 1995;77B:895-900.
14. Boynton MD, Tietjens BR. Long-term followup of the untreated isolated posterior cruciate ligament-deficient knee. Am J Sports Med. 1996;24:306-310.
15. Keller PM, Shelbourne KD, McCarroll JR, Rettig AC. Nonoperatively treated isolated posterior cruciate ligament injuries. Am J Sports Med. 1993;21:132-136.
16. Lipscomb AB Jr, Anderson AF, Norwig ED, et al. Isolated posterior cruciate ligament reconstruction: long-term results. Am J Sports Med. 1993;21:490-496.
17. Wang CJ, Chen HS, Huang TW. Outcome of arthroÂscopic single bundle reconstruction for complete posterior cruciate ligament tear. Injury. 2003;34:747-751.
18. Markolf K, Davies M, Zoric B, McAllister D. Effects of bone block position and orientation within the tibial tunnel for posterior cruciate ligament graft reconstructions: a cyclic loading study of bone-patellar tendon-bone allografts. Am J Sports Med. 2003;31:673-679.
19. Markolf KL, Zemanovic JR, McAllister DR. Cyclic loading of posterior cruciate ligament replacements fixed with tibial tunnel and tibial inlay methods. J Bone Joint Surg. 2002;84A:518-524.
20. McAllister DR, Markolf KL, Oakes DA, et al. A biomechanical comparison of tibial inlay and tibial tunnel posterior cruciate ligament reconstruction techniques: graft pretension and knee laxity. Am J Sports Med. 2002;30:312-317.
21. Oakes DA, Markolf KL, McWilliams J, et al. BioÂmechanical comparison of tibial inlay and tibial tunnel techniques for reconstruction of the posterior cruciate ligament: analysis of graft forces. J Bone Joint Surg. 2002;84A:938-944.
22. Gill TJ, Van de Velde SK, Wing DW, et al. TibioÂfemoral and patellofemoral kinematics after reconstruction of an isolated posterior cruciate ligament injury: in vivo analysis during lunge. Am J Sports Med. 2009;37:2377-2385.
23. Kim YM, Lee CA, Matava MJ. Clinical results of arthroscopic single-bundle transtibial posterior cruciate ligament reconstruction: a systematic review. Am J Sports Med. 2011;39:425-434.
RECOMMENDED READINGS
The authors suggest the following sources for readers seeking more information:
• Margheritini F, Mariani PP. Diagnostic evaluation of posterior cruciate ligament injuries. Knee Surg Sports Traumatol Arthrosc. 2003;11:282-288. The focus in this article is on strategies for initial diagnosis of posterior cruciate ligament injury.
• Wind WM Jr, Bergfeld JA, Parker RD. Evaluation and treatment of posterior cruciate ligament injuries: revisited. Am J Sports Med. 2004;32:1765-1775. This is an excellent comprehensive review of the current literature on posterior cruciate ligament injury.