Synovitis Common in Osteoarthritis
Synovitis is common in osteoarthritis, new research shows. The study suggests the need for a shift in treatment paradigms that target structural disease progression rather than just alleviating pain.
(©AlilaMedicalMediaShutterstock.com)
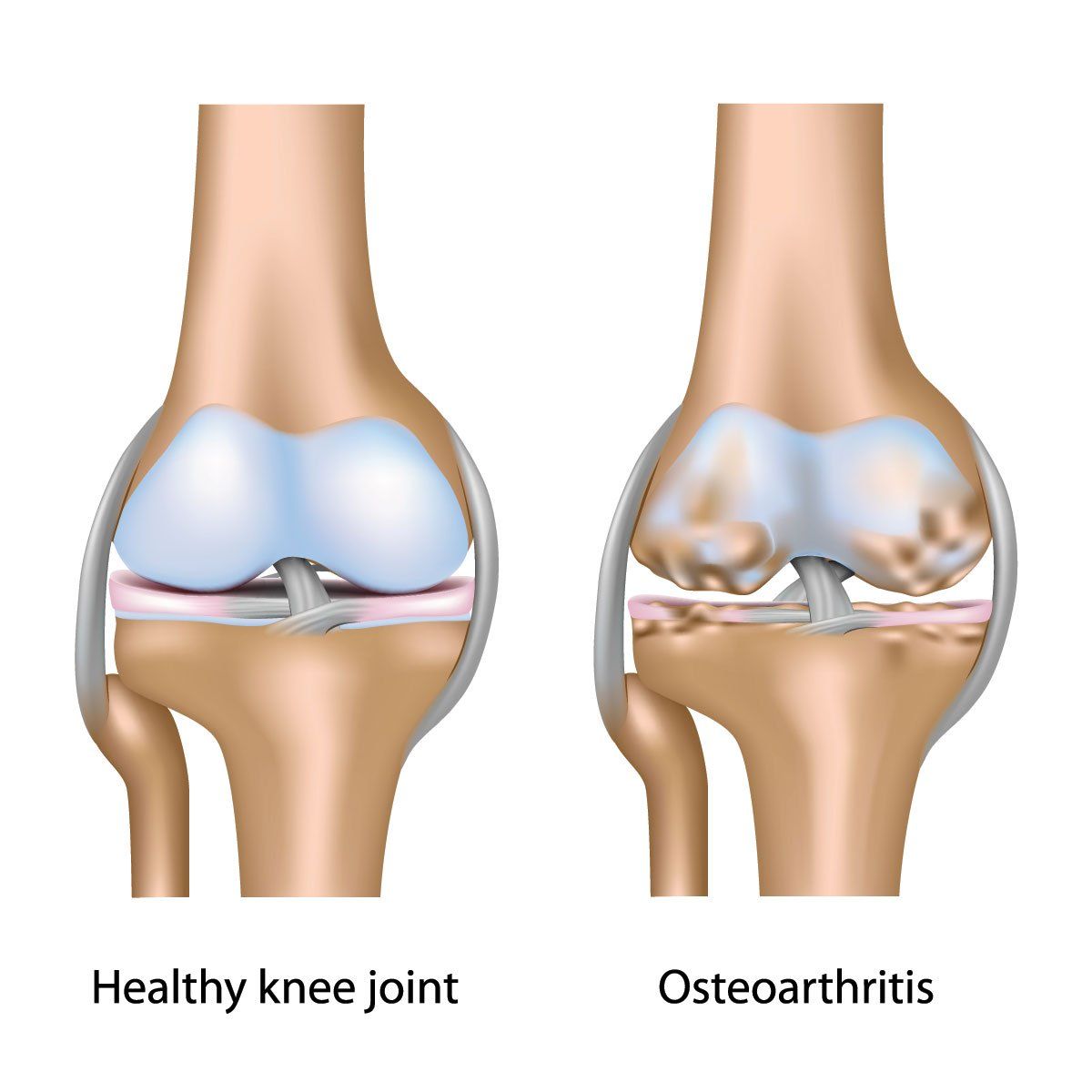
Osteoarthritis (OA) has long been held to be a disease of aging whereby time and overuse of joints cause deterioration of the associated bones and cartilage, promoting the belief that nothing could be done to prevent it. It was in the early 1980s that synovial inflammation was first recognized as a feature of OA, and more recent magnetic resonance imaging (MRI) and ultrasound (US) technologies have contributed mounting evidence of an early inflammatory process that may provide new opportunities for intervention.
In a review just published in Arthritis Research and Therapy, Mathiessen and Conaghan1 found that synovitis is common in OA, and more importantly, suggests the need for a shift in treatment paradigms that target structural disease progression rather than just alleviating pain.
Synovial connective tissue lines the major joints and tendons of the body. As bone cartilage breaks down and releases debris into synovial fluid, an influx of leukocytes triggers increased production of T-cell lymphocytes and particularly macrophages that have been implicated in the immune activation of OA. As pro-inflammatory mediators are produced in response to the joint damage, a constant feedback loop is created that escalates pain and inflammatory damage over time.
New imaging technologies have allowed for observation of synovial hypertrophy and changes to synovial fluid levels and enhancements that correspond to previously recognized histological inflammation known to be involved in OA. The current review pointed to several recent studies documenting synovial hypertrophy and effusion or inflammation in patients with OA of the knee, and which corresponded to histological findings, as well as similar studies of the hand and fingers.
Synovial inflammation has been consistently linked to increased OA pain due to heightened responsiveness of peripheral nociceptor neurons. This pattern creates an enhanced sensitivity to and perception of pain, the authors suggested. An important question facing researchers, however, was whether synovitis independently influences OA progression, which the authors felt was supported by several recent papers. “There is strong evidence that synovitis is associated with further worsening of OA structure,” they reported, concluding that at least some patients receiving current analgesic therapies with anti-inflammatory properties may also experience structural benefits that reduce disease progression.
REFERENCE
1. Mathiessen A, Conaghan PG. Synovitis in osteoarthritis: current understanding with therapeutic implications. Arthritis Res Ther 2017 Feb 2;19(1):18. doi: 10.1186/s13075-017-1229-9.