Ulcers and Gangrene in the Hands and Feet of a 56-Year-Old Man
A 56-year-old man presented with a 1-week history of digital tip ulcers and ischemic gangrene. He alsoreported the recent onset of Raynaud phenomenon and diffuse joint pain.
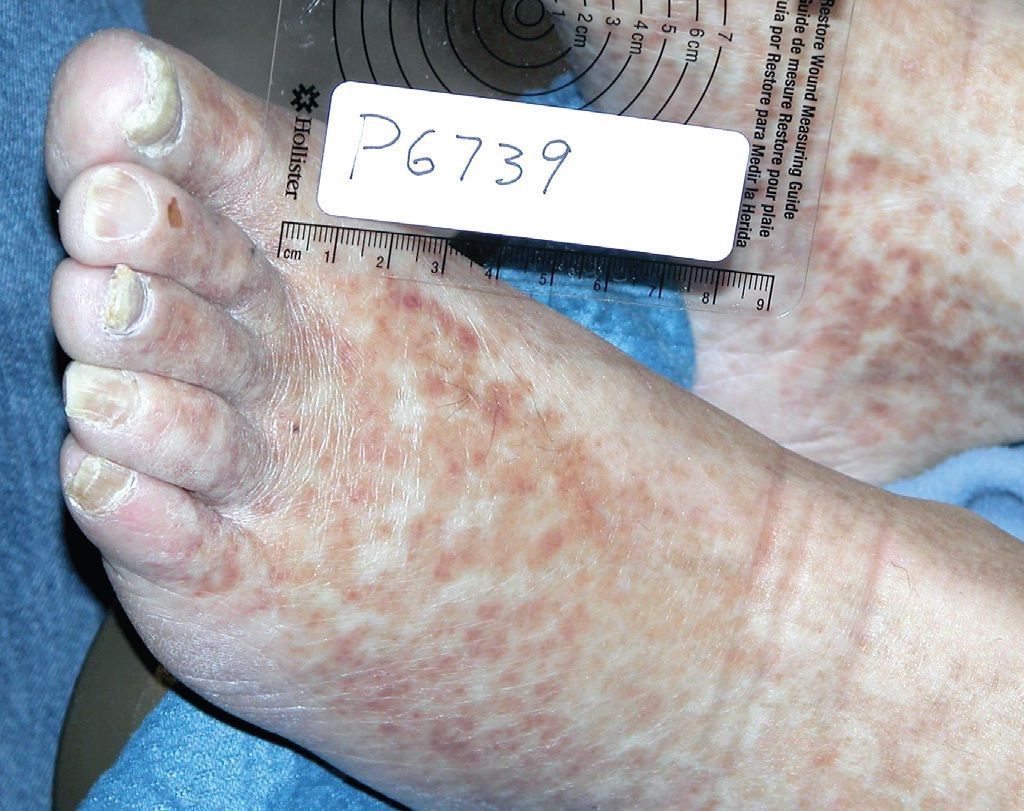
A 56-year-old man presented with a 1-week history of digital tip ulcers and ischemic gangrene. He also reported the recent onset of Raynaud phenomenon and diffuse joint pain.
His past medical history included diabetes, hypertension, and hepatitis C. The results of his physical examination were significant for palpable purpura (photograph, left) and necrotic fingertips (photograph, below).
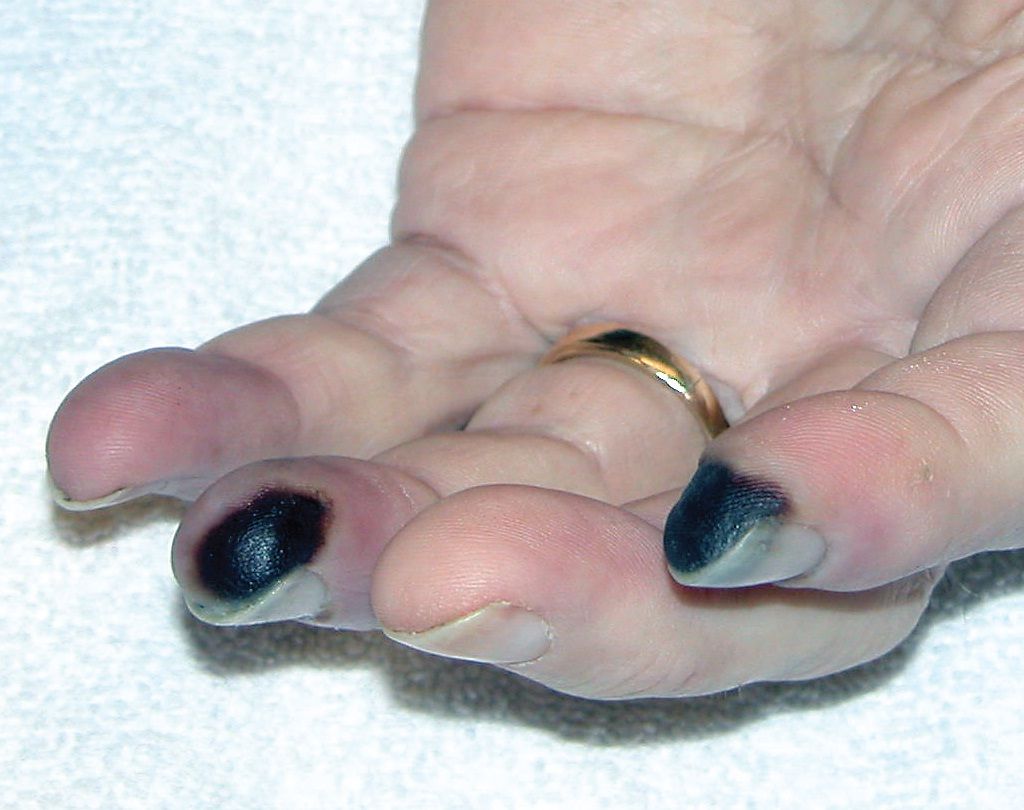
The results of serologic testing showed high titers of antinuclear antibody (ANA) (1:10,240 in speckled pattern; normal, negative), the presence of rheumatoid factor (RF) (1:320; normal, less than 1:80), and low levels of C4. The man’s erythrocyte sedimentation rate was elevated, and an active urinary sediment was present. A polymerase chain reaction (PCR) test for hepatitis C virus (HCV) generated more than 2 million copies, and the results of a type 2 (essential mixed) cryoglobulins assay were positive.
A limited arteriogram of the hands revealed multiple fixed digital artery occlusions without proximal disease.
What is your diagnosis?
(Find the answer on the next page.)
A diagnosis was made of cryoglobulinemic vasculitis in association with HCV infection.
Cryoglobulinemic vasculitis is an immune complex–mediated systemic vasculitis that involves small to medium-size vessels. Cryoglobulinemia is defined as the presence of circulating
immunoglobulins that precipitate at temperatures below 37°C and redissolve on rewarming.
According to cryoprecipitate composition, cryoglobulinemia is classified into 3 serologic subsets:
monoclonal cryoimmunoglobulinemia (type 1), composed of single monoclonal immunoglobulin; and mixed cryoglobulinemia, containing a mixture of polyclonal IgG and monoclonal (type 2) or polyclonal (type 3) IgM rheumatoid factor.Type 1 cryoglobulinemia, frequently associated with well-known hematologic disorders, usually is asymptomatic per se. Essential mixed cryoglobulinemia traditionally has been classified as systemic vasculitis.
In more than 80% of patients, a causative role of HCV has been established; cryoglobulinemic vasculitis is present in up to 5% of patients with HCV.1 HCV has been recognized as both a hepatotropic and lymphotropic virus. Infection of lymphoid tissue may trigger a constellation of autoimmune and lymphoproliferative disorders in chronically infected patients.
The diagnosis in this patient was based on the presence of the typical clinical triad of palpable purpura, weakness, and arthralgias. Other prominent features were Raynaud phenomenon and multiorgan involvement (renal disease).
In addition to the cryocrit assay, other consistent laboratory abnormalities are hypo- complementemia, RF positivity from the cryoglobulins, and the presence of HCV RNA by PCR assay (highly specific). Serum autoantibodies, such as ANA, may be detected in more than half of patients who have cryoglobulinemic vasculitis.1
The complement system consists of at least 30 plasma and membrane proteins that provide an innate defense against microbes and an adjunct or “complement” to humoral immunity. The classic pathway is activated when IgM or IgG antibodies bind to antigens (eg, viruses, bacteria, or autoantigens). Components of the class pathway are designated by the letter C combined with a number (eg, C1 through C4).Activation of the complement system leads to the release of potent mediators of the inflammatory response.
Ninety percent of patients with cryoglobulinemic vasculitis are hypocomplementemic secondary to consumption, with C4 levels characteristically more depressed than C3 levels. The presence of RF and depressed levels of C4 in the serum and the occurrence of clinical features similar to those of rheumatoid arthritis or systemic lupus erythematosus often lead to misdiagnosis. Additional differential diagnoses to consider are other systemic vasculitides and Sjgren syndrome.
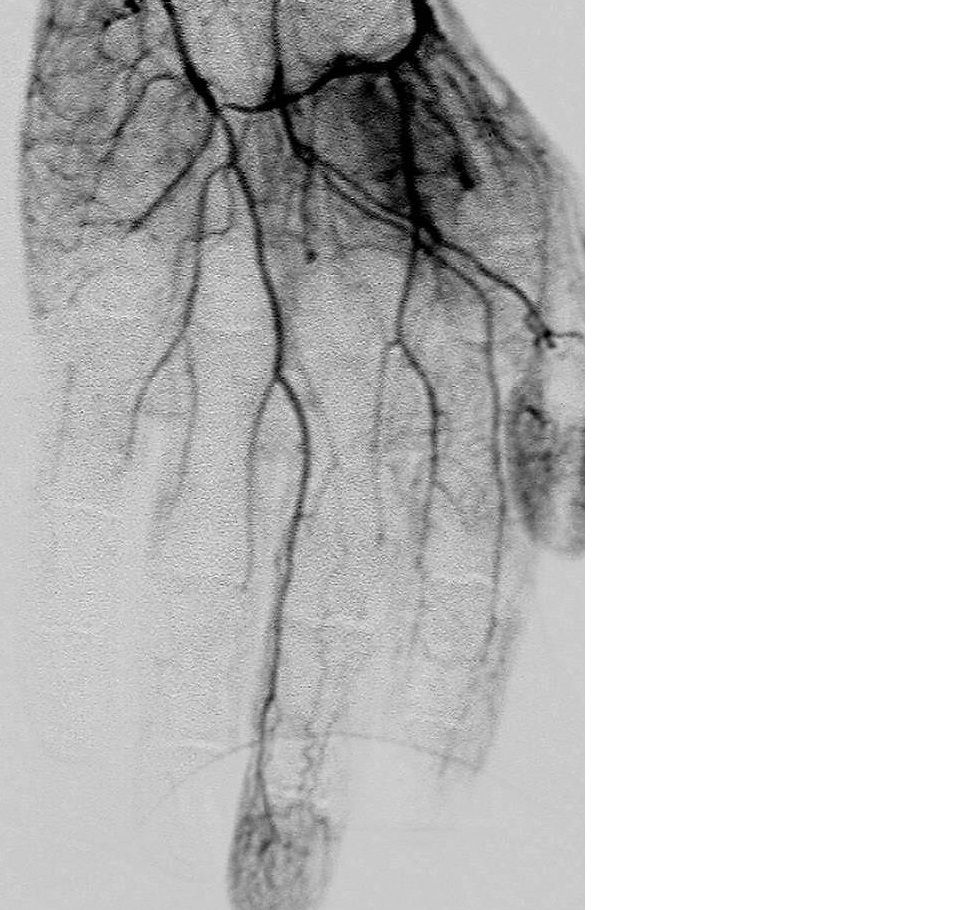
The multiple fixed digital artery occlusions in the arteriogram (left) suggested a vasospastic disorder or vasculitis. Nonreversibility by intra-arterial nitroglycerine suggests atherosclerosis, Buerger disease, vasculopathy, or immune complex vasculitis.
An attempt at HCV eradication should be made in all cases of HCV-associated cryoglobulinemic vasculitis. Treatment of patients with chronic HCV infection involves interferon alpha alone or, preferably, in combination with ribavirin. For relief of symptoms, antiviral treatment leads to an initial clinical response rate of about 75%.2
Traditionally, corticosteroids have been the firstline intervention. Patients with mild polyarthritis often respond to low doses of corticosteroids with or without hydroxychloroquine. Aggressive therapy in idiopathic mixed cryoglobulinemia is reserved primarily for patients with acute severe disease manifested by progressive renal failure, distal necroses requiring amputation, or advanced neuropathy. In such patients, plasmapheresis (to remove the circulation cryoglobulins) has been used with corticosteroids and cyclophosphamide to prevent new antibody formation. More recently, rituximab (monoclonal anti-CD20 antibody) has been used successfully in patients with cryoglobulinemic vasculitis without significant adverse effects.
In this patient, high-dose oral prednisone (1 mg/kg) was started in addition to HCV antiviral therapy. His disease stabilized immediately; there was no more visceral involvement or new digital ulcerations. His digital ulcers healed gradually, and prednisone was tapered over the following year. He did not require any aggressive therapies, such as plasmapheresis or cytotoxic drugs. On follow-up, his arthralgias and Raynaud phenomenon have remained well controlled and there has been no new palpable purpura.
This case was submitted by Samar Gupta, MD, clinical instructor of internal medicine and rheumatology at the University of Colorado Health Sciences Center School of Medicine, Department of Veterans Affairs Medical Center, Cheyenne,Wyoming.
References:
1. Ferri C, Mascia MT. Cryoglobulinemic vasculitis. Curr Opin Rheumatol. 2006;18:54-63.2. Vassilopoulos D, Calabrese LH. Hepatitis C virus infection and vasculitis: implicationsof antiviral and immunosuppressive therapies. Arthritis Rheum. 2002;46:585-597.