Wrist Pain and Hyperpigmentation in a 55-Year-Old Man
A 55-year-old American Indian truck driver presentedwith a 2-day history of right wrist swelling and pain. He denied previous trauma to the wrist or having performed unusual activities.
A 55-year-old American Indian truck driver presented with a 2-day history of right wrist swelling and pain. He denied previous trauma to the wrist or having performed unusual activities. He did not have fever or chills. His medical history was significant for hypercholesterolemia; obstructive sleep apnea; and degenerative arthritis of the shoulders, spine, and knees.
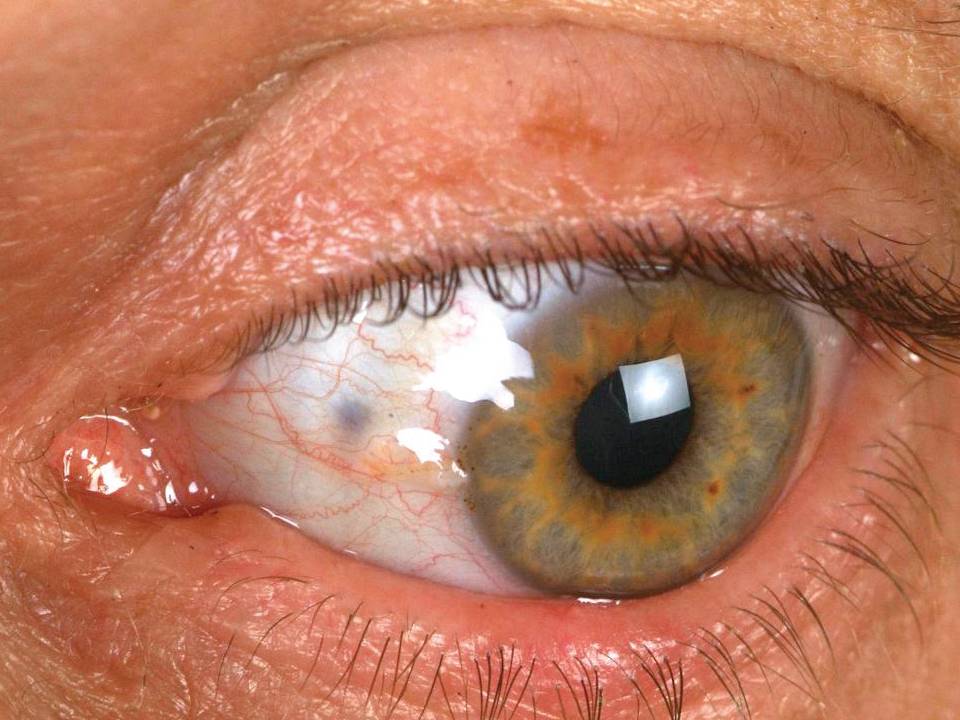
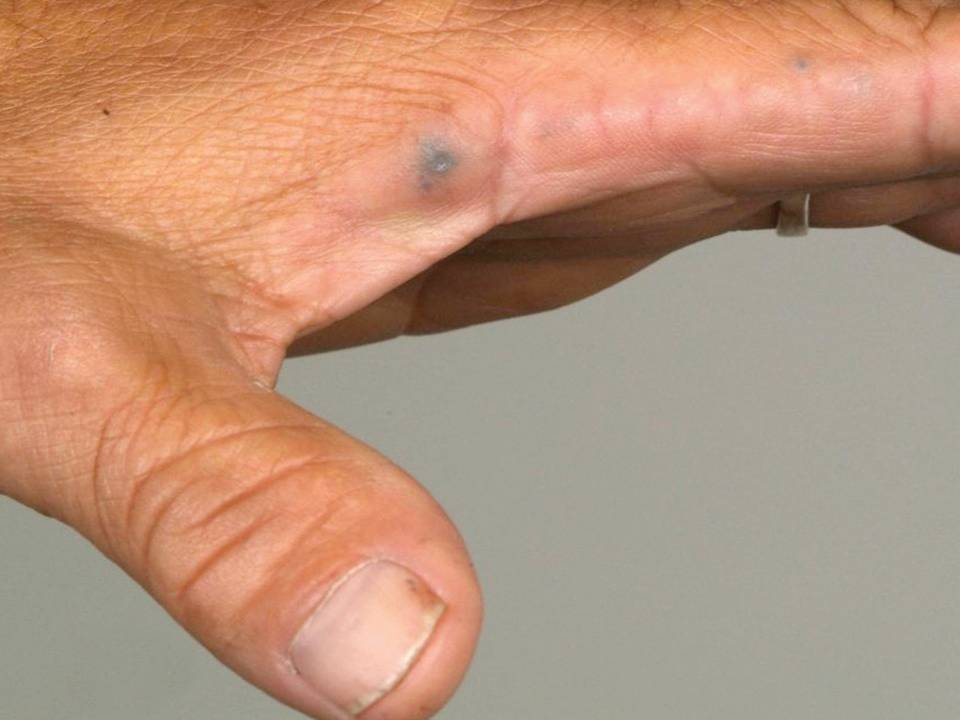
On physical examination, the man’s right wrist appeared swollen; it was tender to touch with limited flexion and extension because of the pain and swelling. The patient also had limited bilateral shoulder abduction and forward flexion without pain. There was limited lumbar flexion and extension without findings of radiculopathy. Other findings included hyperpigmentation of the left conjunctiva (photograph, above left), both pinnae, and both hands (photograph, above right).
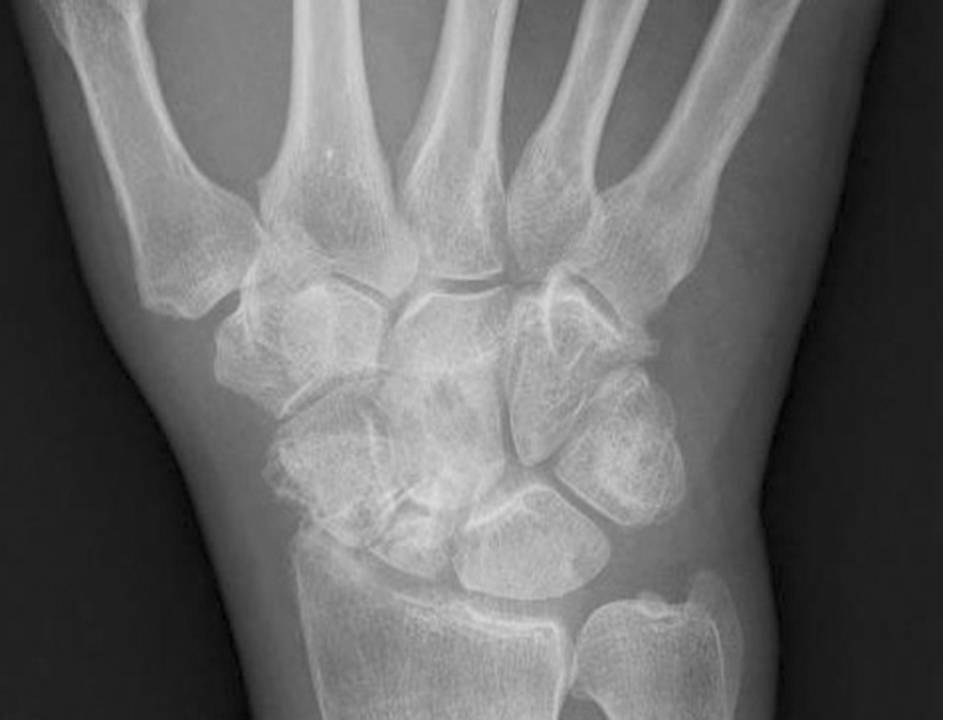
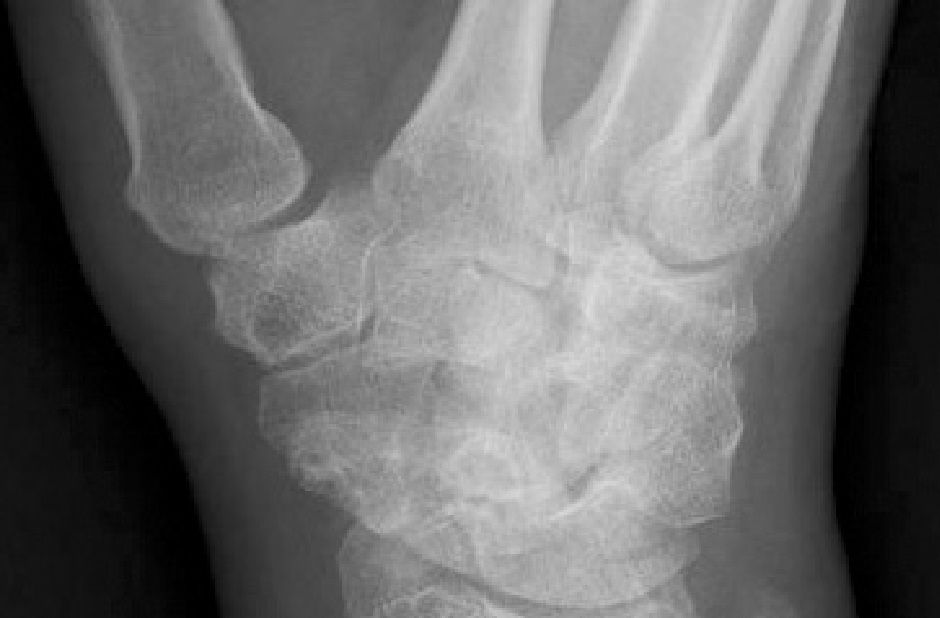
Laboratory study results showed a normal complete blood cell count and metabolic profile. The patient’s uric acid level was 2.2 mg/dL (normal range, 4.8 to 8.7 mg/dL). X-ray films of the patient’s right wrist (anteroposterior [AP] and oblique views, bottom left and right, respectively) showed radiocarpal osteoarthrosis without evidence of chondrocalcinosis.
What is your diagnosis? How would you confirm this diagnosis?
(Find the answer on the next page.)
The patient’s acute right wrist pain could have been the result of crystal-induced arthritis, overuse tenosynovitis, or infectious arthritis. However, the wrist x-ray films did not show evidence of chondrocalcinosis, the patient’s uric acid level was low, and an attempt to aspirate the right wrist did not yield fluid.
The findings of hyperpigmented lesions and a history of multiple-site osteoarthritis suggested an underlying systemic condition. After further questioning, the patient gave a history of having dark urine on standing. In addition, he said that he was informed that black materials were seen in his left shoulder joint during arthroscopic surgery in 1995.These findings are most consistent with ochronosis secondary to alkaptonuria.
Sir Archibald Garrod first described alkaptonuria in 1908 as an inborn error of metabolism.1 It is a rare disorder caused by mutations in the homogentisic acid (HGA) oxidase gene and a deficiency of homogentisate1,2-dioxygenase. Alkaptonuria results in an accumulation of HGA in the soft tissues and cartilage. In addition, it is excreted in large amounts in the urine. HGA is oxidized to benzoquinones; this process forms melanin-like polymers and causes hyperpigmentation of the soft tissues and darkening of urine on standing.
Typically, patients with alkaptonuria present with stiffness and loss of mobility in the large joints during the fourth decade of life. Physical findings include knee effusions and flexion contractures, shoulder and hip arthritis, and progressive lumbar rigidity. Usually, the small peripheral joints are spared. Nonarticular features (eg, hyperpigmentation of the pinnae, sclerae, and axillar and groin areas) also are observed. Clinically significant outcomes include degenerative joint disease of the large joints, such as the hips and knees; renal and prostatic stones; cardiac valve involvement; and coronary artery calcification. Patients who have advanced degenerative joint disease usually have good outcomes with total joint replacement surgery.
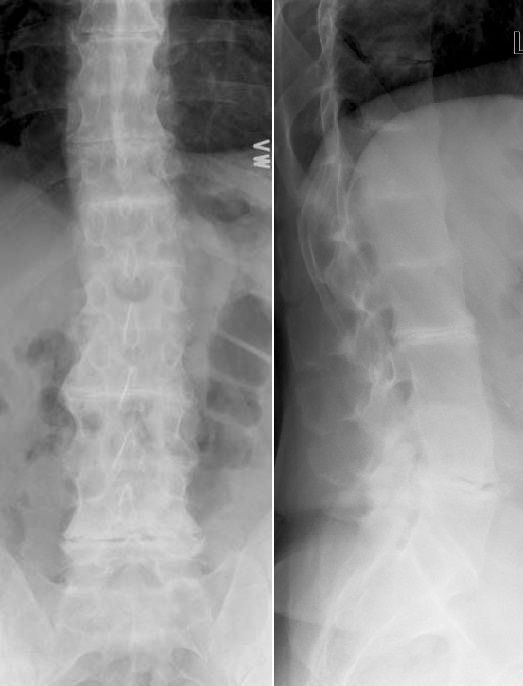
AP (above left) and lateral (above right) x-ray views of the patient’s spine showed characteristic changes. These included diffuse obliteration of all lumbar intervertebral disk spaces associated with prominent calcification of the disks and end-plate sclerosis throughout the lumbar spine. Osteophyte formation is notably absent.
These classic radiographic findings, together with the physical findings of limited range of motion of the lumbar spine and shoulder, hyperpigmentation of the skin and conjunctiva, and a history of black urine on standing, confirmed the diagnosis of ochronosis resulting from alkaptonuria in our patient. Other available diagnostic tests include quantification of urinary or serum HGA using either chromatography or specific enzymatic methods and oxidation by Benedict-Hopkins-Cole reagent or molybdate (Briggs test).
Some medications may produce skin hyperpigmentation and confuse the diagnosis. Reported cases include hyperpigmentation caused by carbolic acid dressings, quinacrine, hydroquinone, amiodarone, and minocycline.3
The traditional recommendation for patients with alkaptonuria is diet modification and restricting use of phenylalanine and tyrosine. However, this approach often is difficult to maintain and there are no clinical trials to support its long-term benefit. The NIH is investigating a new drug, nitisinone (2-[2-nitro-4-trifluoromethylbenzoyl] - 1, 3 cyclohexanedione), as a therapeutic agent for patients with alkaptonuria. Nitisinone inhibits 4-hydroxyphenylpyruvate dioxygenase, the enzyme that produces HGA. Early data showed that this agent significantly reduces urinary HGA excretion and improves symptoms of joint pain.4 A larger clinical trial is under way.
Our patient was treated with oral colchicine and ibuprofen. Symptomatic improvement was seen during the subsequent 2 weeks. During follow-up, the patient required occasional intra-articular corticosteroid injections for knee pain. Currently, his overall pain is controlled reasonably well with diclofenac. In addition, he is participating in an NIH clinical trial for alkaptonuria treatment.
This case was submitted by Thitinan Srikulmontree, MD, an attending physician in rheumatology, and Tangada P.Sudha Rao,MD, chief of the rheumatology section and associate professor of medicine, at Virginia Commonwealth University Health System in Richmond. They are also affiliated with the Hunter Holmes McGuire VA Medical Center, also in Richmond.
References:
1. Prasad C, Galbraith PA. Sir Archibald Garrod and alkaptonuria-‘story of metabolic genetics’. Clin Genet. 2005;68:199-203.2. Phornphutkul C, Introne WJ, Perry MB, et al. Natural history of alkaptonuria. N Engl J Med. 2002;347:2111-2121.3. Suwannarat P, Phornphutkul C, Bernardini I, et al. Minocycline-induced hyperpigmentation masquerading as alkaptonuria in individuals with joint pain. Arthritis Rheum. 2004;50;3698-3701.4. Suwannarat P, O’Brien K, Perry MB, et al. Use of nitisinone in patients with alkaptonuria. Metabolism. 2005;54:719-728.